Volume 10, Issue 1 (Jan & Feb 2020)
J Research Health 2020, 10(1): 27-34 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Shayeghian Z, Amiri P, Hajati E, Gharibzadeh S. Moderating Role of Alexithymia in Relationship Between Perceived Social Support, Diabetes-Related Quality of Life, and Glycated Hemoglobin in Patients With Type 2 Diabetes. J Research Health 2020; 10 (1) :27-34
URL: http://jrh.gmu.ac.ir/article-1-1352-en.html
URL: http://jrh.gmu.ac.ir/article-1-1352-en.html
1- Research Center for Social Determinants of Endocrine Health and Obesity, Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
2- Research Center for Social Determinants of Endocrine Health and Obesity, Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences, Tehran, Iran. ,amiri@endocrine.ac.ir
3- Research Centre for Emerging and Reemerging infectious diseases, Pasteur Institute of Iran, Tehran, Iran.; Department of Epidemiology and Biostatistics, Pasteur Institute of Iran, Tehran, Iran.
2- Research Center for Social Determinants of Endocrine Health and Obesity, Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences, Tehran, Iran. ,
3- Research Centre for Emerging and Reemerging infectious diseases, Pasteur Institute of Iran, Tehran, Iran.; Department of Epidemiology and Biostatistics, Pasteur Institute of Iran, Tehran, Iran.
Full-Text [PDF 615 kb]
(1206 Downloads)
| Abstract (HTML) (3083 Views)
Full-Text: (941 Views)
Introduction
Type 2 Diabetes Mellitus (T2DM) is among the most prevalent chronic diseases and a major public health problem [1]. It has a high prevalence of approximately 6.8 in different regions of Iran [2] and 8.5 in the world [3]. Moreover, T2DM plays a substantial role in the patient’s quality of life [4]. The quality of life impacts adherence to medical treatment and self-management, including self-care activities and medicines taking [5]. Moreover, how a patient takes care of self influences glycated hemoglobin levels (HbA1c; as a reliable indicator for diabetes) [6]. Additionally, some studies indicated that other factors, like social and emotional parameters, affect these relationships [7]. Among social factors, perceived social support has a considerable role in this area [8, 9].
The perceived social support is the perception and actuality that one is cared for, has assistance available from other people, and that one is part of a supportive social network, such as a spouse, relatives or religious institutions, etc. [10]. The perceived social support, as an effective factor, protects people from biopsychological diseases [11, 12]. Additionally, as a “stress buffer,” it positively affects the health status of individuals through health protection against the harmful effects of stressful events and the reduction of the adverse effects of chronic illness [13]. Consequently, it directly and positively affects the quality of life [14]. In a meta-analysis study, Wang, Wu, and Liu investigated 182 studies in this field. They found that social support is a strong predictor of health in the patient’s life [15]. In addition to social support, one of the strongest predictors of optimal performance and improved health in diabetes patients is emotional competence, and especially emotion regulation [16]; previous studies have mentioned less than two issues of quality of life and social support.
Alexithymia is defined as the disability and difficulty in the cognitive processing of emotional information and emotion regulation. Alexithymia has three dimensions, as follows: difficulty in identifying feelings (DIF), difficulty in describing feelings (DDF), and externally oriented thinking (EOT); underlies the disease and is a sophisticated factor in managing some physical conditions [7]. People with alexithymia, overestimate normal physical feeling, misinterpret the physical symptoms of emotional arousal, demonstrate emotional helplessness by physical complaints, and seek to treat physical symptoms by therapeutic procedures [17].
The importance of considering the role of alexithymia in the mechanisms of development and maintenance of chronic diseases is increasing. This is because alexithymia characteristics (difficulty in identifying and describing feelings) is a significant risk factor for psychosomatic disorders [18]. Motan et al. argued that alexithymia is strongly related to the biopsychological health status of patients [19]. This is because the ability to perception and regulation of emotions leads to better management of chronic diseases [7]. Housiaux et al. also documented that alexithymia had a significant and positive association with glycated hemoglobin in people with diabetes; i.e. higher scores on the difficulty in the verbal descriptions of feelings are related to higher levels of glycated hemoglobin [7].
Numerous studies also reported that alexithymia is related to a low quality of life in different medical diseases, especially diabetes [20-22]. Alexithymia leads to a decreased perception of the quality of life by reducing the perceived social support and limiting social networks, and consequently, by creating defects in social skills [11]. The lack of ability to recognize and describe the feeling leads to decreased individual perception of social support. Moreover, the individual has deficits in recognizing the emotions of others and responding to them appropriately [23].
Studies revealed the effect of social support on the quality of life and glycated hemoglobin in patients with T2DM. Moreover, alexithymia impacts the process and severity of diabetes; therefore, it is expected to influence the relationship between social support and quality of life in patients. The present study determined the role of alexithymia on the relationship between social support, quality of life, and glycated hemoglobin in patients with T2DM. According to previous studies on the health moderators, it is hypothesized that alexithymia moderates the relationship between social support, quality of life, and glycated hemoglobin in T2DM.
methods
This was an analytical cross-sectional study. One hundred patients with T2DM (60% females) were selected by convenience sampling method between February 2013 and January 2014 from the Endocrine Clinic at Labbafinejad Hospital in Tehran City, Iran. The inclusion criteria were the age range of 40 to 60 years and providing an informed consent form. Exclusion criteria were hospitalization, diabetes complications (e.g. nephropathy or neuropathy, and emergency surgery). Free-of-charge blood tests were provided as an incentive for all study participations. This study was approved by the Ethics Committee of Shahid Beheshti University of Medical Sciences.
All study participants completed 4 questionnaires, including socio-demographic characteristics form, Multidimensional Scale of Perceived Social Support (MSPSS), The Audit of Diabetes-Dependent Quality of Life (ADDQoL), and Toronto Alexithymia Scale (TAS-20).
Multidimensional Scale of Perceived Social Support (MSPSS)
This is a 12-item self-report scale that assesses total perceived social support and its dimensions (family, friends, and significant others’ support) [24]. The scale’s psychometric properties are well established abroad with the coefficients of internal consistency of .85-.91 and test-retest reliabilities of 0.72-0.85 [25]. In Iran, the reliability coefficients for the total scale and each of its dimensions has been reported to be acceptable, 0.91, 0.87, and 0.83, and 0.89, respectively [26].
The Audit of Diabetes-Dependent Quality of Life (ADDQoL)
ADDQoL assessed the quality of life of people with diabetes and reflects how every aspect of diabetes affects the patient’s life [27]. This specific scale has 19 items. Each item is scored on a 5-point scale, and the scoring is from +1 (positive effect) to -3 (negative effect). Moreover, to normalize the values and for the ability to compare the raw scores of quality of life, the score rank of each person must be multiplied by its importance [28]. This scale has appropriate validity and reliability [29]. Its calculated Cronbach’s alpha coefficient was equal to 0.91 for the Persian version and 0.69 in retesting (P˂0.001), suggesting its desirable reliability [30]. In the present study, its Cronbach’s alpha coefficient was obtained as 0.95.
Toronto Alexithymia Scale (TAS-20)
This is a 20-item self-report scale [31]. Each item is evaluated on a 5-point Likert-type scale (from 1 to 5). Five items are reverse scored. This scale has three dimensions. Seven items for Difficulty Identifying Feelings (DIF), which assesses the respondent’s ability to identify feelings, and to distinguish between feelings and bodily sensations of emotional arousal (e.g. “I am often confused about the emotions I feel”) Five items belong to Difficulty Describing Feelings (DDF), which reflects difficulty in communicating feelings with other people (e.g. “I can easily describe my feelings”) Eight items are dedicated to Externally Oriented Thinking (EOT) style, which estimates the degree to which respondents are more concerned with external, objective events than their inner psychological states (e.g. “I prefer to solve problems rather than describing them”). In samples of adult Iranian populations, reliability coefficients for total scale alexithymia scores, and its three factors were 0.85, 0.82, 0.75, and 0.72, respectively [32].
Glycated Hemoglobin Measurement (HbA1c)
Hemoglobin A1C provides an average value of blood glucose control over the past 2 to 3 months. It is an important blood test that suggests how well diabetes is being controlled. The normal range of glycated hemoglobin in healthy subjects is 4%-7% and the American Diabetes Association has defined levels <7% as appropriate glycemic control. High levels of glycated hemoglobin indicate poor control of blood glucose [33]. In this study, glycaemic hemoglobin values were measured using the HPLC method and DS5 HbA1c measurement system (Hb gold).
The Kolmogorov–Smirnov test was used for the distribution of continuous variables. Normally-distributed data were expressed by mean and standard deviation, and categorical data were expressed by frequency (percentage). The Independent Samples t-test was used to compare the mean score difference of continuous variables in two genders. Furthermore, the Chi-squared test was used to compare categorical data. To evaluate the role of alexithymia in the relationship between perceived social support, diabetes-related quality of life, and quality of life, two hierarchical multiple regression analyses were calculated, as follows:
In the first analysis, the diabetes-related quality of life was considered the criterion variable; first, social support was entered as the predictor variable, followed by the main effect alexithymia (second step) and interaction alexithymia × social support (third step). In the second analysis, HbA1c was the criterion variable; first, social support was entered as a predictor variable, followed by the main effect alexithymia (second step) and interaction alexithymia × social support (third step). All obtained data were analyzed in SPSS.
Results
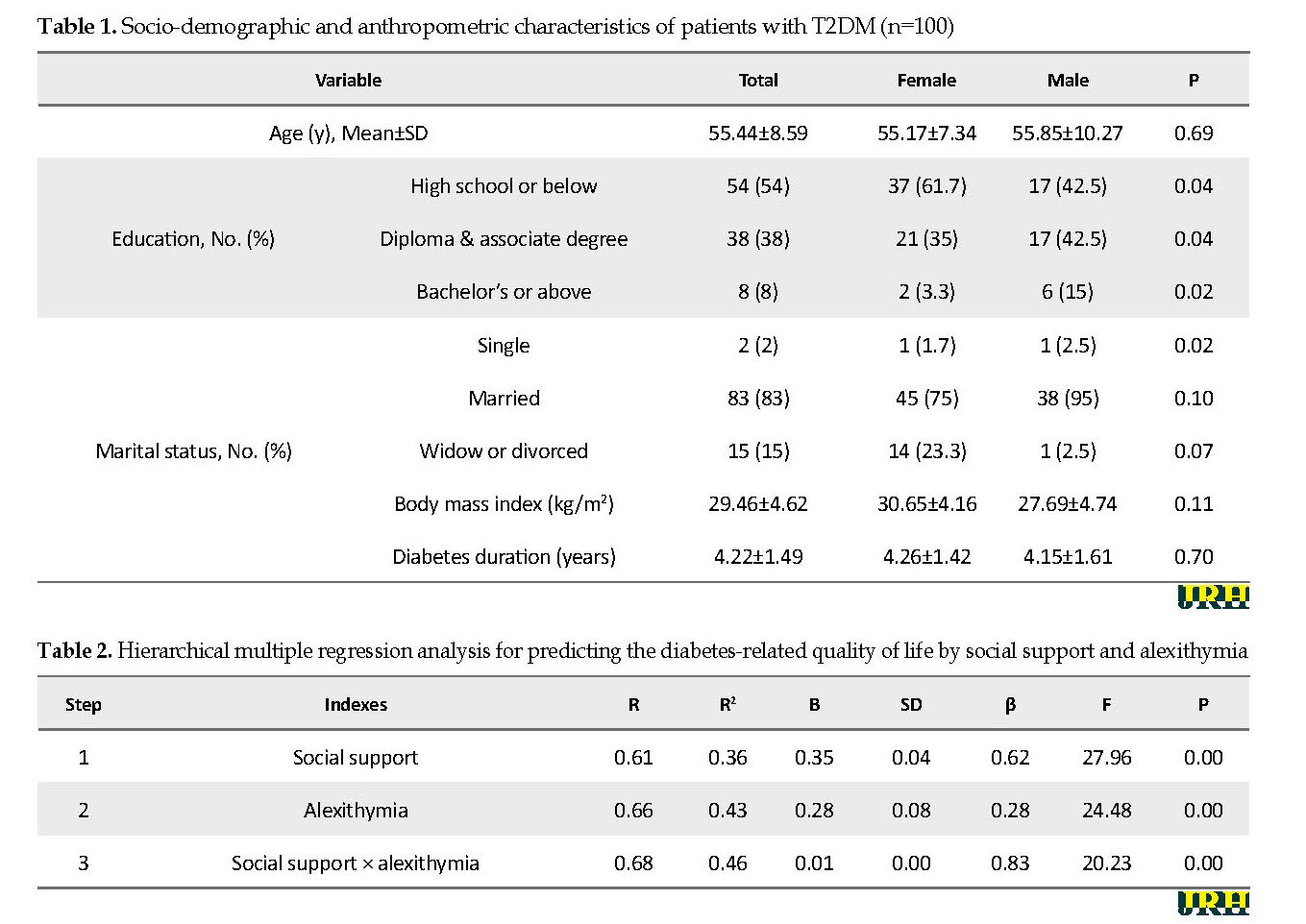
Demographic and anthropometric characteristics of 100 patients with T2DM (60% females) with the mean±SD age of 55.44±8.59 years are listed in Table 1. In total, 83% of the study samples were married, and 54% had primary school education. In addition, 72% were prescribed with oral glucose-lowering therapy to control blood glucose, 2% received insulin alone, and 25% used both medication and insulin. Table 2 presents the result of hierarchical multiple regression analysis for predicting the diabetes-related quality of life by social support and alexithymia.
Type 2 Diabetes Mellitus (T2DM) is among the most prevalent chronic diseases and a major public health problem [1]. It has a high prevalence of approximately 6.8 in different regions of Iran [2] and 8.5 in the world [3]. Moreover, T2DM plays a substantial role in the patient’s quality of life [4]. The quality of life impacts adherence to medical treatment and self-management, including self-care activities and medicines taking [5]. Moreover, how a patient takes care of self influences glycated hemoglobin levels (HbA1c; as a reliable indicator for diabetes) [6]. Additionally, some studies indicated that other factors, like social and emotional parameters, affect these relationships [7]. Among social factors, perceived social support has a considerable role in this area [8, 9].
The perceived social support is the perception and actuality that one is cared for, has assistance available from other people, and that one is part of a supportive social network, such as a spouse, relatives or religious institutions, etc. [10]. The perceived social support, as an effective factor, protects people from biopsychological diseases [11, 12]. Additionally, as a “stress buffer,” it positively affects the health status of individuals through health protection against the harmful effects of stressful events and the reduction of the adverse effects of chronic illness [13]. Consequently, it directly and positively affects the quality of life [14]. In a meta-analysis study, Wang, Wu, and Liu investigated 182 studies in this field. They found that social support is a strong predictor of health in the patient’s life [15]. In addition to social support, one of the strongest predictors of optimal performance and improved health in diabetes patients is emotional competence, and especially emotion regulation [16]; previous studies have mentioned less than two issues of quality of life and social support.
Alexithymia is defined as the disability and difficulty in the cognitive processing of emotional information and emotion regulation. Alexithymia has three dimensions, as follows: difficulty in identifying feelings (DIF), difficulty in describing feelings (DDF), and externally oriented thinking (EOT); underlies the disease and is a sophisticated factor in managing some physical conditions [7]. People with alexithymia, overestimate normal physical feeling, misinterpret the physical symptoms of emotional arousal, demonstrate emotional helplessness by physical complaints, and seek to treat physical symptoms by therapeutic procedures [17].
The importance of considering the role of alexithymia in the mechanisms of development and maintenance of chronic diseases is increasing. This is because alexithymia characteristics (difficulty in identifying and describing feelings) is a significant risk factor for psychosomatic disorders [18]. Motan et al. argued that alexithymia is strongly related to the biopsychological health status of patients [19]. This is because the ability to perception and regulation of emotions leads to better management of chronic diseases [7]. Housiaux et al. also documented that alexithymia had a significant and positive association with glycated hemoglobin in people with diabetes; i.e. higher scores on the difficulty in the verbal descriptions of feelings are related to higher levels of glycated hemoglobin [7].
Numerous studies also reported that alexithymia is related to a low quality of life in different medical diseases, especially diabetes [20-22]. Alexithymia leads to a decreased perception of the quality of life by reducing the perceived social support and limiting social networks, and consequently, by creating defects in social skills [11]. The lack of ability to recognize and describe the feeling leads to decreased individual perception of social support. Moreover, the individual has deficits in recognizing the emotions of others and responding to them appropriately [23].
Studies revealed the effect of social support on the quality of life and glycated hemoglobin in patients with T2DM. Moreover, alexithymia impacts the process and severity of diabetes; therefore, it is expected to influence the relationship between social support and quality of life in patients. The present study determined the role of alexithymia on the relationship between social support, quality of life, and glycated hemoglobin in patients with T2DM. According to previous studies on the health moderators, it is hypothesized that alexithymia moderates the relationship between social support, quality of life, and glycated hemoglobin in T2DM.
methods
This was an analytical cross-sectional study. One hundred patients with T2DM (60% females) were selected by convenience sampling method between February 2013 and January 2014 from the Endocrine Clinic at Labbafinejad Hospital in Tehran City, Iran. The inclusion criteria were the age range of 40 to 60 years and providing an informed consent form. Exclusion criteria were hospitalization, diabetes complications (e.g. nephropathy or neuropathy, and emergency surgery). Free-of-charge blood tests were provided as an incentive for all study participations. This study was approved by the Ethics Committee of Shahid Beheshti University of Medical Sciences.
All study participants completed 4 questionnaires, including socio-demographic characteristics form, Multidimensional Scale of Perceived Social Support (MSPSS), The Audit of Diabetes-Dependent Quality of Life (ADDQoL), and Toronto Alexithymia Scale (TAS-20).
Multidimensional Scale of Perceived Social Support (MSPSS)
This is a 12-item self-report scale that assesses total perceived social support and its dimensions (family, friends, and significant others’ support) [24]. The scale’s psychometric properties are well established abroad with the coefficients of internal consistency of .85-.91 and test-retest reliabilities of 0.72-0.85 [25]. In Iran, the reliability coefficients for the total scale and each of its dimensions has been reported to be acceptable, 0.91, 0.87, and 0.83, and 0.89, respectively [26].
The Audit of Diabetes-Dependent Quality of Life (ADDQoL)
ADDQoL assessed the quality of life of people with diabetes and reflects how every aspect of diabetes affects the patient’s life [27]. This specific scale has 19 items. Each item is scored on a 5-point scale, and the scoring is from +1 (positive effect) to -3 (negative effect). Moreover, to normalize the values and for the ability to compare the raw scores of quality of life, the score rank of each person must be multiplied by its importance [28]. This scale has appropriate validity and reliability [29]. Its calculated Cronbach’s alpha coefficient was equal to 0.91 for the Persian version and 0.69 in retesting (P˂0.001), suggesting its desirable reliability [30]. In the present study, its Cronbach’s alpha coefficient was obtained as 0.95.
Toronto Alexithymia Scale (TAS-20)
This is a 20-item self-report scale [31]. Each item is evaluated on a 5-point Likert-type scale (from 1 to 5). Five items are reverse scored. This scale has three dimensions. Seven items for Difficulty Identifying Feelings (DIF), which assesses the respondent’s ability to identify feelings, and to distinguish between feelings and bodily sensations of emotional arousal (e.g. “I am often confused about the emotions I feel”) Five items belong to Difficulty Describing Feelings (DDF), which reflects difficulty in communicating feelings with other people (e.g. “I can easily describe my feelings”) Eight items are dedicated to Externally Oriented Thinking (EOT) style, which estimates the degree to which respondents are more concerned with external, objective events than their inner psychological states (e.g. “I prefer to solve problems rather than describing them”). In samples of adult Iranian populations, reliability coefficients for total scale alexithymia scores, and its three factors were 0.85, 0.82, 0.75, and 0.72, respectively [32].
Glycated Hemoglobin Measurement (HbA1c)
Hemoglobin A1C provides an average value of blood glucose control over the past 2 to 3 months. It is an important blood test that suggests how well diabetes is being controlled. The normal range of glycated hemoglobin in healthy subjects is 4%-7% and the American Diabetes Association has defined levels <7% as appropriate glycemic control. High levels of glycated hemoglobin indicate poor control of blood glucose [33]. In this study, glycaemic hemoglobin values were measured using the HPLC method and DS5 HbA1c measurement system (Hb gold).
The Kolmogorov–Smirnov test was used for the distribution of continuous variables. Normally-distributed data were expressed by mean and standard deviation, and categorical data were expressed by frequency (percentage). The Independent Samples t-test was used to compare the mean score difference of continuous variables in two genders. Furthermore, the Chi-squared test was used to compare categorical data. To evaluate the role of alexithymia in the relationship between perceived social support, diabetes-related quality of life, and quality of life, two hierarchical multiple regression analyses were calculated, as follows:
In the first analysis, the diabetes-related quality of life was considered the criterion variable; first, social support was entered as the predictor variable, followed by the main effect alexithymia (second step) and interaction alexithymia × social support (third step). In the second analysis, HbA1c was the criterion variable; first, social support was entered as a predictor variable, followed by the main effect alexithymia (second step) and interaction alexithymia × social support (third step). All obtained data were analyzed in SPSS.
Results
Demographic and anthropometric characteristics of 100 patients with T2DM (60% females) with the mean±SD age of 55.44±8.59 years are listed in Table 1. In total, 83% of the study samples were married, and 54% had primary school education. In addition, 72% were prescribed with oral glucose-lowering therapy to control blood glucose, 2% received insulin alone, and 25% used both medication and insulin. Table 2 presents the result of hierarchical multiple regression analysis for predicting the diabetes-related quality of life by social support and alexithymia.
According to regression analysis results, 36% of the variance of diabetes-related quality of life was explained by social support; by adding alexithymia, it increased to %43. The third step, after entering the moderating effect of social support × alexithymia, explained 46% of the variance of diabetes-related quality of life (P<0.001). The moderating role of alexithymia increased by 10% of the R2 value, which was significant (P<0.05, df=4.68, and DR2=0.02). Moreover, to determine the effect of alexithymia dimensions (DIF, DDF & EOT) on the quality of life, in another analysis, stepwise regression analysis was used. Its obtained results indicated that DIF alone explained 30% of the variance of diabetes-related quality of life (P<0.001, β=0.54, F=41.03). Furthermore, the two other dimensions (DDF and EOT) were excluded from data analysis.
The hierarchical multiple regression analysis results for predicting glycated hemoglobin by social support and alexithymia are outlined in Table 3.
The hierarchical multiple regression analysis results for predicting glycated hemoglobin by social support and alexithymia are outlined in Table 3.
According to the regression analysis results, social support explained 23% of the variance of glycated hemoglobin; by adding alexithymia, this value increased to 31%. In the third step, the interactive effect of social support × alexithymia was included in the model and was statistically significant (P<0.001). Additionally, alexithymia moderated the effect of social support on glycaemic hemoglobin. The moderating role of alexithymia increased by 12% of the R2 value, which was significant (P<0.05, DF=5.62, DR2=0.04). Furthermore, to determine the effect of alexithymia dimensions (DIF, DDF & EOT) on glycated hemoglobin, stepwise regression analysis was used. Its relevant results revealed that DIF alone explained 34% of the variance of glycated hemoglobin (P<0.001, β=0.69, F=51.26). Moreover, the two other dimensions (DDF and EOT) were excluded from data analysis.
Discussion
The current study investigated the role of alexithymia in the relationship between perceived social support, quality of life,e and glycated hemoglobin in patients with T2DM. The obtained results indicated that social support in patients with T2DM has a significant positive correlation with the quality of life and a significant negative correlation with glycated hemoglobin. Moreover, there was a significant negative correlation between the quality of life and alexithymia. In other words, when patients perceived more effective social support, they reported a better quality of life, more appropriate hemoglobin levels, and a lower score of alexithymia.
These findings were in line with those of Tang et al. and Glasgow et al. who reported a significant positive relationship between social support and quality of life in patients with diabetes [34, 35]. Lumely et al. [11]and Meunier et al. [36] founded a significant negative relationship between social support and glycated hemoglobin in patients with diabetes. In addition, Bratis et al. [37] and Posse et al. [38] suggested a significant negative relationship between social support and alexithymia. This means that individuals with alexithymia, regardless of the perceived social support, have difficulty in establishing social relationships and using social support. This is because of their poor emotional awareness, including empathy and understanding of the experiences of others which is indispensable for the formation and development of intimate relationships and consequently encountering health issues [23].
Other studies suggested that social support and alexithymia in patients with T2DM were predictors of their life quality; this finding was in line with those of Liu et al. [39] and Tang et al. [34] who stated social support is a predictor of life quality in patients with diabetes. Grassi et al. [21] also documented that alexithymia is a predictor of the quality of life in patients.
Besides, the collected results revealed that alexithymia moderates the relationship between social support and quality of life, and glycated hemoglobin. In line with these findings, Schafer et al. reported that patients who had weaker family ties were less likely to comply with diabetes diet; thus, they had unfavorable metabolic control, leading to a negative effect on their quality of life [40]. In other words, the difficulty in identifying and describing feelings (DIF and DDF) leads to an inability to recognizing the individual requirements and expressing them to others. Consequently, it reduces social support perception and the use of health services. Therefore, their metabolic control would be reduced and consequently, glycated hemoglobin would be increased. These issues would harm the patients’ quality of life [7].
The results of measuring the dimensions of alexithymia by regression analysis suggested that the only DIF was a predictor of quality of life in patients. This finding is consistent with that of Housiaux et al. [7] who stated DIF interferes with the ability of patients to receive health services and their disease management. Meunier et al. in their study (n=45 patients with diabetes), demonstrated that DIF was associated with higher levels of blood glucose; therefore, it should be considered as a vulnerable factor in the intensity and change of quality of life in diabetes patients [36].
A limitation of this study was using self-report measures. The relatively small sample size also limited the generalizability of the research outcomes. Finally, to enrich the impact of future management research, we recommend applying multilevel designs to existing models and considering the effects of these variables in the treatment. Additionally, to enhance the effectiveness of therapeutic interventions in improving the quality of life and controlling blood glucose in patients with T2DM, we recommend considering the emotional aspects of the disease, especially alexithymia.
Conclusion
Diabetes management is complex and challenging. Consequently, controlling this process is a permanent challenge, influenced by the intertwined collection of biopsychosocial factors. Social support, as one of the factors influencing the quality of life and glycated hemoglobin, is effective in numerous diabetes-related interventions. Furthermore, alexithymia, as a psychological construct, plays a moderating role in the relationship between these factors. Understanding these factors and their relationships provides contexts for future studies and appropriate planning for more effective interventions in diabetes control. Improvement and development of quality of life in patients with diabetes are important and effective in promoting the therapeutic purposes of diabetes; these purposes would not be achieved without identifying psychosocial moderators and factors influencing the quality of life and glycemic control. Eventually, the high prevalence of alexithymia in patients with diabetes and its effect on their quality of life and glycated hemoglobin reflects the importance of this psychological construct in diabetes. Thus, it requires particular attention from health officials.
Ethical Considerations
Compliance with ethical guidelines
ethical approval for the study was obtained from the Ethics Committee of the Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences (code: 433EC).
Funding
this research was supported by the Social Determinants Endocrine Health & Obesity Research Center, Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences.
Authors' contributions
Study design: Zeinab Shayeghian, Parisa Amiri; Data collection and analysis: Elnaz Hajati, Safoora Gharibzadeh; Manuscript preparation: Zeinab Shayeghian, Parisa Amiri, Elnaz Hajati.
Conflict of interest
The authors declared no competing interests.
Acknowledgments
We thank Labafinejad Hospital staff and all patients who participated in this study.
References
Tuomilehto J, Schwarz P, Lindström J. Long-term benefits from lifestyle interventions for type 2 diabetes prevention: Time to expand the efforts. Diabetes Care. 2011; 34(2):S210-4. [DOI:10.2337/dc11-s222] [PMID] [PMCID]
Masoodi MR, Mahdi Nosratabadi M, Zohreh Halvaiepour Z, Yousefi S, Karimi M. [Exploring the empowerment index and its related factors in type 2 diabetes patients in Sirjan city (Persian)]. Med J Mashhad Univ Medical Sci. 2016; 59(1):56-63.
Mathers CD, Loncar D. Projections of global mortality and burden of disease from 2002 to 2030. PLoS Med. 2006; 3(11):1-20. [DOI:10.1371/journal.pmed.0030442] [PMID] [PMCID]
Wändell PE. Quality of life of patients with diabetes mellitus. An overview of research in primary health care in the Nordic countries. Scand J Prim Health Care. 2005; 23(2):68-74. [DOI:10.1080/02813430510015296] [PMID]
Zhang X, Norris SL, Chowdhury FM, Gregg EW, Zhang P. The effects of interventions on health-related quality of life among persons with diabetes: A systematic review. Med Care. 2007; 45(9):820-34. [DOI:10.1097/MLR.0b013e3180618b55] [PMID]
Boardbent E, Petrie KJ, Main J, Weinman J. The brief illness perception questionnaire. J Psychosom Res. 2006; 60(6):631-7. [DOI:10.1016/j.jpsychores.2005.10.020] [PMID]
Housiaux M, Luminet O, Van Broeck N, Dorchy H. Alexithymia is associated with glycaemic control of children with type 1 diabetes. Diabetes Metab. 2010; 36(6 Pt 1):455-62. [DOI:10.1016/j.diabet.2010.06.004] [PMID]
Helgeston VS, Cohen S. Social support and adjustment to cancer: reconciling descriptive, correlational and intervention research. Health Psychol. 1996; 15(2):135-48. [DOI:10.1037/0278-6133.15.2.135]
Stopford R, Winkley K, Ismail K. Social Support and glycemic control in type 2 diabetes: a systematic review of observation studies. Patient Educ Couns. 2013; 93(3):549-58. [DOI:10.1016/j.pec.2013.08.016] [PMID]
Taylor SE. Health psychology (5th ed.). New York: McGraw-Hill; 2003.
Lumley MA, Ovies T, Stettner L, Wehmer F, Lakey B. Alexithymia, Social Support and Health Problem. J Psychosom Res. 1996; 41(6):519-30. [DOI:10.1016/S0022-3999(96)00227-9]
Mcdowell TL, Serovich JM. The effect of perceived and actual social support on the mental health of HIV-positive persons. AIDS Care. 2007; 19(10):1223-9. [DOI:10.1080/09540120701402830] [PMID] [PMCID]
Kojima M, Hayano J, Tokudome S, Suzuki S, Ibuki K, Tomizawa H and et al. Independent associations of alexithymia and social support with depression in hemodialysis patients. J Psychosom Res. 2007; 63(4):349-56. [DOI:10.1016/j.jpsychores.2007.04.002] [PMID]
Göz F, Karaoz S, Goz M, Ekiz S, Cetin I. Effects of the diabetic patients’ perceived social support on their quality-of-life. J Clin Nurs. 2007; 16(7):1353-60. [DOI:10.1111/j.1365-2702.2007.01472.x] [PMID]
Wang HH, Wu SZ, Liu YY. Association between social support and health outcomes: a meta-analysis. Kaohsiung J Med Sci. 2003; 19(7):345-51. [DOI:10.1016/S1607-551X(09)70436-X]
Thompson RA, Meyer S. Socialization of emotion regulation in the family. In: Gross JJ, eds. Handbook of emotion regulation. New York: Guilford Press; 2007:249-68.
Taylor GJ, Bagby RM. New trends in alexithymia research. Psychother Psychosom. 2004; 73(2):68-77. [DOI:10.1159/000075537] [PMID]
Dubey A, Pandey R, Mishra K. Role of Emotion Regulation Difficulties and Positive/Negative Affectivity in Explaining Alexithymia- Health Relationship: An overview. Int J Soc Sci Res. 2010; 7(1):20-31
Motan I, Gencoz T. The relationship between the dimensions of alexithymia and the intensity of depression and anxiety. Turk Psikiyatri Derg. 2007; 18(4):333-43.
Pucheu S, Consoli SM, Francais P, Issad B, D’Auzac C. The relationship of quality of life with the severity of disease and non-expression of emotions in peritoneal dialysis. Perit Dial Int. 2004; 24(1):77-9.
Grassi L, Rossi E, Sabato S, Cruciani G, Zambelli M. Diagnostic criteria for psychosomatic research and psychosocial variables in breast cancer patients. Psychosomatics. 2004; 45(6):483-91. [DOI:10.1176/appi.psy.45.6.483] [PMID]
Topsever P, Filiz TM, Salman S, Sengul A, Sarac E, Topalli R, et al. Alexithymia in diabetes mellitus. Scott Med J. 2006; 51(3):15-20. [DOI:10.1258/RSMSMJ.51.3.15] [PMID]
Karukivi M, Joukamaa M, Hautala L, Kaleva O, Haapasalo-Pesu K, Liuksila P, et al. Does perceived social support and parental attitude relate to alexithymia? A study in Finnish late adolescents. Psychiatry Res. 2011; 187(1-2):254-60. [DOI:10.1016/j.psychres.2010.11.028] [PMID]
Zimet GD, Powell SS, Farley GK, Werkan S, Berkoff K. The multidimensional scale of perceived social support. J Person Assess. 1990; 52(3-4):610-7. [DOI:10.1080/00223891.1990.9674095] [PMID]
Edwards LM. Measuring perceived social support in mexican american youth: Psychometric properties of the multidimensional scale of perceived social support. Hisp J Behav Sci. 2004; 26(2):187-94 [DOI:10.1177/0739986304264374]
Besharat MA. [Psychometric properties and factor structure of the multidimensional scale perceived social support (Persian) (Research Report)]. Tehran: University of Tehran; 2003.
Speight J, Reaney MD, Barnard KD. Not all roads lead to Rome-a review of quality of life measurement in adults with diabetes. Diabet Med. 2009; 26(4):315-27. [DOI:10.1111/j.1464-5491.2009.02682.x] [PMID]
Bradley C, Speight J. Patient perceptions of diabetes and diabetes therapy: Assessing quality of life. Diabetes Metab Res Rev. 2002; 18(3):S64-9. [DOI:10.1002/dmrr.279] [PMID]
Garratt AM, Schmidt L, Fitzpatrick R. Patient-assessed health outcome measures for diabetes: A structured review. Diabet Med. 2002; 19(1):1-11. [DOI:10.1046/j.1464-5491.2002.00650.x] [PMID]
Poursharifi H. [Effectiveness of motivational interviewing on improving physical health outcomes in adults with Type II diabetes [Dissertation] (Persian)]. Tehran: University of Tehran; 2007.
Parker JDA, Taylor GJ, Bagby RM. The 20-item Toronto Alexithymia Scale: III reliability and factorial validity in a community population. J Psychosom Res. 2003; 55(3):269-75. [DOI:10.1016/S0022-3999(02)00578-0]
Besharat MA. Reliability and factorial validity of Farsi version of the Toronto Alexithymia Scale with a sample of Iranian students. Psychol Rep. 2007; 101: 209-20. [DOI:10.2466/PR0.101.5.209-220] [PMID]
Larsen ML, Horder M, Mogensen EF. Effect of long-term monitoring of glycosylated hemoglobin levels in insulin-dependent diabetes mellitus. N Engl J Med. 1990; 323(15):1021-5. [DOI:10.1056/NEJM199010113231503] [PMID]
Tang TS, Brown MB, Funnell MM, Anderson RM. Social support, quality of life, and self-care behaviors among African Americans with type 2 diabetes. Diabetes Educ. 2008; 34(2):266-76. [DOI:10.1177/0145721708315680] [PMID]
Glasgow RE, Barrera M Jr, McKay HG, Boles SM. Social support, self-management, and quality of life among participants in an internet-based diabetes support program: A multi-dimensional investigation. Cyberpsychol Behav. 1999; 2(4):271-81. [DOI:10.1089/cpb.1999.2.271] [PMID]
Meunier J, Dorchy H, Luminet O. Does family cohensiveness and parental alexithymia predict glycaemic control in children and adolescent with diabetes? Diabetes Metab. 2008; 34(5):473-81. [DOI:10.1016/j.diabet.2008.03.005] [PMID]
Bratis D, Tselebis A, Sikaras C, Moulou A, Giotakis K, Zoumakis E, et al. Alexithymia and its association with burnout, depression and family support among Greek nursing staff. Hum Resour Health. 2009; 7:72. [DOI:10.1186/1478-4491-7-72] [PMID] [PMCID]
Posse M, Hällström T, Backenroth-Ohsako G. Alexithymia, social support, psycho-social stress and mental health in a female population. Nord J Psychiatry. 2002; 56(5):329-34. [DOI:10.1080/080394802760322088] [PMID]
Liu Y, Maier M, Hao Y, Chen Y, Qin Y, Huo R. Factors related to quality of life for patients with type 2 diabetes with or without depressive symptoms - results from a community-based study in China. J Clin Nurs. 2013; 22 (1-2):80-8. [DOI:10.1111/jocn.12010] [PMID]
Schafer LC, Mccaul KD, Glasgow RE. Supportive and non supportive family behavior: Relationship to adherence and metabolic control in person with type 1 diabetes. Diabetes Care. 1986; 9(2):179-85. [DOI:10.2337/diacare.9.2.179] [PMID]
Discussion
The current study investigated the role of alexithymia in the relationship between perceived social support, quality of life,e and glycated hemoglobin in patients with T2DM. The obtained results indicated that social support in patients with T2DM has a significant positive correlation with the quality of life and a significant negative correlation with glycated hemoglobin. Moreover, there was a significant negative correlation between the quality of life and alexithymia. In other words, when patients perceived more effective social support, they reported a better quality of life, more appropriate hemoglobin levels, and a lower score of alexithymia.
These findings were in line with those of Tang et al. and Glasgow et al. who reported a significant positive relationship between social support and quality of life in patients with diabetes [34, 35]. Lumely et al. [11]and Meunier et al. [36] founded a significant negative relationship between social support and glycated hemoglobin in patients with diabetes. In addition, Bratis et al. [37] and Posse et al. [38] suggested a significant negative relationship between social support and alexithymia. This means that individuals with alexithymia, regardless of the perceived social support, have difficulty in establishing social relationships and using social support. This is because of their poor emotional awareness, including empathy and understanding of the experiences of others which is indispensable for the formation and development of intimate relationships and consequently encountering health issues [23].
Other studies suggested that social support and alexithymia in patients with T2DM were predictors of their life quality; this finding was in line with those of Liu et al. [39] and Tang et al. [34] who stated social support is a predictor of life quality in patients with diabetes. Grassi et al. [21] also documented that alexithymia is a predictor of the quality of life in patients.
Besides, the collected results revealed that alexithymia moderates the relationship between social support and quality of life, and glycated hemoglobin. In line with these findings, Schafer et al. reported that patients who had weaker family ties were less likely to comply with diabetes diet; thus, they had unfavorable metabolic control, leading to a negative effect on their quality of life [40]. In other words, the difficulty in identifying and describing feelings (DIF and DDF) leads to an inability to recognizing the individual requirements and expressing them to others. Consequently, it reduces social support perception and the use of health services. Therefore, their metabolic control would be reduced and consequently, glycated hemoglobin would be increased. These issues would harm the patients’ quality of life [7].
The results of measuring the dimensions of alexithymia by regression analysis suggested that the only DIF was a predictor of quality of life in patients. This finding is consistent with that of Housiaux et al. [7] who stated DIF interferes with the ability of patients to receive health services and their disease management. Meunier et al. in their study (n=45 patients with diabetes), demonstrated that DIF was associated with higher levels of blood glucose; therefore, it should be considered as a vulnerable factor in the intensity and change of quality of life in diabetes patients [36].
A limitation of this study was using self-report measures. The relatively small sample size also limited the generalizability of the research outcomes. Finally, to enrich the impact of future management research, we recommend applying multilevel designs to existing models and considering the effects of these variables in the treatment. Additionally, to enhance the effectiveness of therapeutic interventions in improving the quality of life and controlling blood glucose in patients with T2DM, we recommend considering the emotional aspects of the disease, especially alexithymia.
Conclusion
Diabetes management is complex and challenging. Consequently, controlling this process is a permanent challenge, influenced by the intertwined collection of biopsychosocial factors. Social support, as one of the factors influencing the quality of life and glycated hemoglobin, is effective in numerous diabetes-related interventions. Furthermore, alexithymia, as a psychological construct, plays a moderating role in the relationship between these factors. Understanding these factors and their relationships provides contexts for future studies and appropriate planning for more effective interventions in diabetes control. Improvement and development of quality of life in patients with diabetes are important and effective in promoting the therapeutic purposes of diabetes; these purposes would not be achieved without identifying psychosocial moderators and factors influencing the quality of life and glycemic control. Eventually, the high prevalence of alexithymia in patients with diabetes and its effect on their quality of life and glycated hemoglobin reflects the importance of this psychological construct in diabetes. Thus, it requires particular attention from health officials.
Ethical Considerations
Compliance with ethical guidelines
ethical approval for the study was obtained from the Ethics Committee of the Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences (code: 433EC).
Funding
this research was supported by the Social Determinants Endocrine Health & Obesity Research Center, Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences.
Authors' contributions
Study design: Zeinab Shayeghian, Parisa Amiri; Data collection and analysis: Elnaz Hajati, Safoora Gharibzadeh; Manuscript preparation: Zeinab Shayeghian, Parisa Amiri, Elnaz Hajati.
Conflict of interest
The authors declared no competing interests.
Acknowledgments
We thank Labafinejad Hospital staff and all patients who participated in this study.
References
Tuomilehto J, Schwarz P, Lindström J. Long-term benefits from lifestyle interventions for type 2 diabetes prevention: Time to expand the efforts. Diabetes Care. 2011; 34(2):S210-4. [DOI:10.2337/dc11-s222] [PMID] [PMCID]
Masoodi MR, Mahdi Nosratabadi M, Zohreh Halvaiepour Z, Yousefi S, Karimi M. [Exploring the empowerment index and its related factors in type 2 diabetes patients in Sirjan city (Persian)]. Med J Mashhad Univ Medical Sci. 2016; 59(1):56-63.
Mathers CD, Loncar D. Projections of global mortality and burden of disease from 2002 to 2030. PLoS Med. 2006; 3(11):1-20. [DOI:10.1371/journal.pmed.0030442] [PMID] [PMCID]
Wändell PE. Quality of life of patients with diabetes mellitus. An overview of research in primary health care in the Nordic countries. Scand J Prim Health Care. 2005; 23(2):68-74. [DOI:10.1080/02813430510015296] [PMID]
Zhang X, Norris SL, Chowdhury FM, Gregg EW, Zhang P. The effects of interventions on health-related quality of life among persons with diabetes: A systematic review. Med Care. 2007; 45(9):820-34. [DOI:10.1097/MLR.0b013e3180618b55] [PMID]
Boardbent E, Petrie KJ, Main J, Weinman J. The brief illness perception questionnaire. J Psychosom Res. 2006; 60(6):631-7. [DOI:10.1016/j.jpsychores.2005.10.020] [PMID]
Housiaux M, Luminet O, Van Broeck N, Dorchy H. Alexithymia is associated with glycaemic control of children with type 1 diabetes. Diabetes Metab. 2010; 36(6 Pt 1):455-62. [DOI:10.1016/j.diabet.2010.06.004] [PMID]
Helgeston VS, Cohen S. Social support and adjustment to cancer: reconciling descriptive, correlational and intervention research. Health Psychol. 1996; 15(2):135-48. [DOI:10.1037/0278-6133.15.2.135]
Stopford R, Winkley K, Ismail K. Social Support and glycemic control in type 2 diabetes: a systematic review of observation studies. Patient Educ Couns. 2013; 93(3):549-58. [DOI:10.1016/j.pec.2013.08.016] [PMID]
Taylor SE. Health psychology (5th ed.). New York: McGraw-Hill; 2003.
Lumley MA, Ovies T, Stettner L, Wehmer F, Lakey B. Alexithymia, Social Support and Health Problem. J Psychosom Res. 1996; 41(6):519-30. [DOI:10.1016/S0022-3999(96)00227-9]
Mcdowell TL, Serovich JM. The effect of perceived and actual social support on the mental health of HIV-positive persons. AIDS Care. 2007; 19(10):1223-9. [DOI:10.1080/09540120701402830] [PMID] [PMCID]
Kojima M, Hayano J, Tokudome S, Suzuki S, Ibuki K, Tomizawa H and et al. Independent associations of alexithymia and social support with depression in hemodialysis patients. J Psychosom Res. 2007; 63(4):349-56. [DOI:10.1016/j.jpsychores.2007.04.002] [PMID]
Göz F, Karaoz S, Goz M, Ekiz S, Cetin I. Effects of the diabetic patients’ perceived social support on their quality-of-life. J Clin Nurs. 2007; 16(7):1353-60. [DOI:10.1111/j.1365-2702.2007.01472.x] [PMID]
Wang HH, Wu SZ, Liu YY. Association between social support and health outcomes: a meta-analysis. Kaohsiung J Med Sci. 2003; 19(7):345-51. [DOI:10.1016/S1607-551X(09)70436-X]
Thompson RA, Meyer S. Socialization of emotion regulation in the family. In: Gross JJ, eds. Handbook of emotion regulation. New York: Guilford Press; 2007:249-68.
Taylor GJ, Bagby RM. New trends in alexithymia research. Psychother Psychosom. 2004; 73(2):68-77. [DOI:10.1159/000075537] [PMID]
Dubey A, Pandey R, Mishra K. Role of Emotion Regulation Difficulties and Positive/Negative Affectivity in Explaining Alexithymia- Health Relationship: An overview. Int J Soc Sci Res. 2010; 7(1):20-31
Motan I, Gencoz T. The relationship between the dimensions of alexithymia and the intensity of depression and anxiety. Turk Psikiyatri Derg. 2007; 18(4):333-43.
Pucheu S, Consoli SM, Francais P, Issad B, D’Auzac C. The relationship of quality of life with the severity of disease and non-expression of emotions in peritoneal dialysis. Perit Dial Int. 2004; 24(1):77-9.
Grassi L, Rossi E, Sabato S, Cruciani G, Zambelli M. Diagnostic criteria for psychosomatic research and psychosocial variables in breast cancer patients. Psychosomatics. 2004; 45(6):483-91. [DOI:10.1176/appi.psy.45.6.483] [PMID]
Topsever P, Filiz TM, Salman S, Sengul A, Sarac E, Topalli R, et al. Alexithymia in diabetes mellitus. Scott Med J. 2006; 51(3):15-20. [DOI:10.1258/RSMSMJ.51.3.15] [PMID]
Karukivi M, Joukamaa M, Hautala L, Kaleva O, Haapasalo-Pesu K, Liuksila P, et al. Does perceived social support and parental attitude relate to alexithymia? A study in Finnish late adolescents. Psychiatry Res. 2011; 187(1-2):254-60. [DOI:10.1016/j.psychres.2010.11.028] [PMID]
Zimet GD, Powell SS, Farley GK, Werkan S, Berkoff K. The multidimensional scale of perceived social support. J Person Assess. 1990; 52(3-4):610-7. [DOI:10.1080/00223891.1990.9674095] [PMID]
Edwards LM. Measuring perceived social support in mexican american youth: Psychometric properties of the multidimensional scale of perceived social support. Hisp J Behav Sci. 2004; 26(2):187-94 [DOI:10.1177/0739986304264374]
Besharat MA. [Psychometric properties and factor structure of the multidimensional scale perceived social support (Persian) (Research Report)]. Tehran: University of Tehran; 2003.
Speight J, Reaney MD, Barnard KD. Not all roads lead to Rome-a review of quality of life measurement in adults with diabetes. Diabet Med. 2009; 26(4):315-27. [DOI:10.1111/j.1464-5491.2009.02682.x] [PMID]
Bradley C, Speight J. Patient perceptions of diabetes and diabetes therapy: Assessing quality of life. Diabetes Metab Res Rev. 2002; 18(3):S64-9. [DOI:10.1002/dmrr.279] [PMID]
Garratt AM, Schmidt L, Fitzpatrick R. Patient-assessed health outcome measures for diabetes: A structured review. Diabet Med. 2002; 19(1):1-11. [DOI:10.1046/j.1464-5491.2002.00650.x] [PMID]
Poursharifi H. [Effectiveness of motivational interviewing on improving physical health outcomes in adults with Type II diabetes [Dissertation] (Persian)]. Tehran: University of Tehran; 2007.
Parker JDA, Taylor GJ, Bagby RM. The 20-item Toronto Alexithymia Scale: III reliability and factorial validity in a community population. J Psychosom Res. 2003; 55(3):269-75. [DOI:10.1016/S0022-3999(02)00578-0]
Besharat MA. Reliability and factorial validity of Farsi version of the Toronto Alexithymia Scale with a sample of Iranian students. Psychol Rep. 2007; 101: 209-20. [DOI:10.2466/PR0.101.5.209-220] [PMID]
Larsen ML, Horder M, Mogensen EF. Effect of long-term monitoring of glycosylated hemoglobin levels in insulin-dependent diabetes mellitus. N Engl J Med. 1990; 323(15):1021-5. [DOI:10.1056/NEJM199010113231503] [PMID]
Tang TS, Brown MB, Funnell MM, Anderson RM. Social support, quality of life, and self-care behaviors among African Americans with type 2 diabetes. Diabetes Educ. 2008; 34(2):266-76. [DOI:10.1177/0145721708315680] [PMID]
Glasgow RE, Barrera M Jr, McKay HG, Boles SM. Social support, self-management, and quality of life among participants in an internet-based diabetes support program: A multi-dimensional investigation. Cyberpsychol Behav. 1999; 2(4):271-81. [DOI:10.1089/cpb.1999.2.271] [PMID]
Meunier J, Dorchy H, Luminet O. Does family cohensiveness and parental alexithymia predict glycaemic control in children and adolescent with diabetes? Diabetes Metab. 2008; 34(5):473-81. [DOI:10.1016/j.diabet.2008.03.005] [PMID]
Bratis D, Tselebis A, Sikaras C, Moulou A, Giotakis K, Zoumakis E, et al. Alexithymia and its association with burnout, depression and family support among Greek nursing staff. Hum Resour Health. 2009; 7:72. [DOI:10.1186/1478-4491-7-72] [PMID] [PMCID]
Posse M, Hällström T, Backenroth-Ohsako G. Alexithymia, social support, psycho-social stress and mental health in a female population. Nord J Psychiatry. 2002; 56(5):329-34. [DOI:10.1080/080394802760322088] [PMID]
Liu Y, Maier M, Hao Y, Chen Y, Qin Y, Huo R. Factors related to quality of life for patients with type 2 diabetes with or without depressive symptoms - results from a community-based study in China. J Clin Nurs. 2013; 22 (1-2):80-8. [DOI:10.1111/jocn.12010] [PMID]
Schafer LC, Mccaul KD, Glasgow RE. Supportive and non supportive family behavior: Relationship to adherence and metabolic control in person with type 1 diabetes. Diabetes Care. 1986; 9(2):179-85. [DOI:10.2337/diacare.9.2.179] [PMID]
Type of Study: Orginal Article |
Subject:
● International Health
Received: 2019/04/13 | Accepted: 2019/09/9 | Published: 2020/01/1
Received: 2019/04/13 | Accepted: 2019/09/9 | Published: 2020/01/1
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |