Volume 10, Issue 4 (Jul & Aug 2020)
J Research Health 2020, 10(4): 257-266 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Hajibabaei H, Sadeghi Soghdel H, Faraji Dizaji S, Ahmadi A. Health Expenditures in Developing Countries: Determinants and Guidelines. J Research Health 2020; 10 (4) :257-266
URL: http://jrh.gmu.ac.ir/article-1-1415-en.html
URL: http://jrh.gmu.ac.ir/article-1-1415-en.html
1- Department of Economic Development Faculty of Management and Economics, Tarbiat Modares University,Tehran, Iran. , hamidreza.hajibabaei@yahoo.com
2- Department of Economic Development Faculty of Management and Economics, Tarbiat Modares University,Tehran, Iran.
2- Department of Economic Development Faculty of Management and Economics, Tarbiat Modares University,Tehran, Iran.
Full-Text [PDF 702 kb]
(1413 Downloads)
| Abstract (HTML) (2458 Views)
Full-Text: (2977 Views)
1. Introduction
The health care issue figures prominently among the millennium development goals set by the United Nations in September 2000 and signed by nearly 190 countries. Better health outcomes are crucial for improving economic welfare at micro and macro levels. A healthy population is bound to bring higher economic value added [1]. Improved quality of life in any country depends on the availability and accessibility to healthcare facilities at affordable costs [2]. Health expenditure is important for policymakers not only due to health outcome importance but also because of the gradual total health expenditure that has become a major concern [3]. In most countries, a rise in the growth rate of health expenditures and its share in the Gross Domestic Product (GDP) have been observed over time [4].
This increase (since the 1960s) raised concerns of financing this newly extended part of the economy. In light of continued cost pressures and strains on public finances, health systems across the countries are striving to increase the value of money. The financing of health care expenditure is therefore a predominant concern in any country, more so in developing countries where severe budget constraints apply and where health outcomes are not good enough. As the resources are scarce in developing countries, if the Ministry of Health can increase the allocation of budget in the health sector, individual spending as out-of-pocket expenditure is expected to reduce significantly. Therefore, out-of-pocket money expenditures in parallel with governing expenditures to render health services, have become a burning concern for developing countries [5]. That is why over the last couple of decades, it has been a point of debate, both for applied econometricians and health economists to analyze health expenditures and its determinants [6].
Himmelstein & Woolhandler [7] see even more role for health expenditures. They believe that a decline in public health spending can potentially undermine preventive measures and weaken responses to health inequalities and new health threats. Additionally, households with catastrophic health expenditures face challenges in offset by the potentially excessive health expenditure and may have been obliged to reduce consumption of other items [8]. These notions make it clear that health expenditure is not just related to the health sector and policymakers should see more roles for macro variables.
The global financial crisis of 2008 and 2009 has highlighted the significance of the relationship between economic growth rates and government expenditure, in general, and health expenditures in particular [4]. This recent downturn has emphasized the usefulness of macroeconomic analysis of health finance and a systematic approach to the development of the evidence-based policy. A recent OECD (Organization for Economic Co-operation and Development) publication noted that after recent slow GDP growth, public health expenditures continued to rise leading to an increase in the ratio of health expenditures to GDP in many countries [9].
These concepts show that health expenditure is not only important due to health outcomes but also because of macroeconomic matters. Macro variables like real per capita incomes, technological innovation, and the aging of the population are generally considered to exert important influences on the growth of health expenditures [10]. Overwhelmingly, studies find that non-medical factors of health consistently play a substantially larger role than medical factors [11]. The literature is full of studies dating back to the 1970s that indicate that poor social determinants of health are harmful to health both in the short- and long-term. Also, a growing body of literature demonstrates the positive impact of favorable social conditions on health outcomes. According to Bradley et al. [12], the ratio of social expenditures to health expenditures was significantly associated with better outcomes in infant mortality, life expectancy, and increased potential life years lost, after adjusting for the level of health expenditures and GDP. Analyses of differentials on health care expenditure by socioeconomic and demographic characteristics of a population can contribute towards a better understanding of existing variations and develop appropriate policies and models for new interventions [13].
Powerful drivers of health lie outside the conventional medical care delivery system, so we should not equate investment in clinical care with investment in health. Such policies, although not typically viewed as health policies, have the potential to improve the health and longevity and to reduce health disparities [14]. The best available evidence suggests that a health policy framework addressing macro determinants of health would achieve better population health, less inequality, and lower costs. Bradley and Taylor (2013) argue that residents of nations that have higher ratios of spending on social services than spending on health care services have better health and live longer [15].
Adler et al. (2016) asserted that the existence of health disparities and fluctuations in health and health inequalities in relation to policy-driven changes in social conditions point to the importance of policies that address social determinants. Such policies, although not typically viewed as health policies, have the potential to improve the health and longevity and reduce health disparities [14]. Zaman et al. (2017) found out that total health expenditure is more sensitive to the gross domestic product rather than life expectancy [5]. As David et al. (2017) put it forward, analyses of differentials on health care expenditure by socioeconomic characteristics could contribute towards a better understanding of existing variations in catastrophic health expenditures and impoverishment that could be used to develop appropriate policies and models to new interventions [13].
The trends and determinants of health expenditure in developed countries have been widely examined and revealed that the main determinants of health expenditure growth include income, the aging of the population, and technological progress. Much evidence is found in the contexts of developed nations and very little is seen in the context of developing nations [16]. WHO (December 2011) says the pace of health expenditures growth is different for countries at various levels of economic development. The financing of the internal organizations and political restraints of health care decision-making are country-specific and heterogeneous [17]. As countries become more developed and wealthier, they devote more public resources to health and spend proportionately more on health per capita [4]. So in this article, the homogeneity assumption is put away and developing countries’ determinants are found out. To do so, all credible determinants of health expenditures are mentioned, and eventually, by using the econometrics method, significant variables are determined and their coefficients are estimated. In this way, we can exactly say how much these variables affect health expenditures and answer three questions which have remained unclear about developing countries’ health expenditures:
Is the growth in health expenditures inevitable in these countries?
What are the determinants of health expenditures in developing countries?
Can we suggest any guidelines to deal with health expenditures?
Health expenditures and its determinants have been a point of debate for many reasons. On the one hand, there are in general the important issues of providing health at affordable costs, health expenditure growth, funding this newly extended part of the economy, and the impact of its funding on other sectors. On the other hand, there is, in particular, the necessity to know its determinants to enable policymakers to predict its development, especially in developing countries. Because these countries suffer from budget limitations, health policymakers and health economists should investigate health expenditure determinants and their coefficients to provide affordable health without putting much pressure on other sectors of the economy. Thus, probing health expenditures and its determinants can help governments enforce cost-containment measures, decrease expenditures, provide a better health system by saved money, and have a better understanding of expenditures trends to face future.
2. Methods
To estimate the health expenditures function, we used a panel data method which provides an increased degree of freedom and efficiency and decreases multicollinearity due to having access to more data. Eviews 8, World Bank, and UNDP data are used for this estimation. Iran, Turkey, Azerbaijan, Georgia, Jordan, Lebanon, Malaysia, Mexico, Costa Rica, Venezuela, and Cuba were chosen as crosses. These countries were selected due to having the same HDI (Human Development index). Not only the countries with the same HDI have the same human development (the most recent available comprehensive data for development) but also have the same income, education, and health indexes which are the determinants of health expenditures. All data of these countries have been collected for 5 years, from 2010 until 2014. To find out the determinants of health expenditures, all credible variables in the literature were investigated. There is extensive literature on the determinants of health expenditures. All of these studies have considered the approach of the demand function to specify their models. Specifically, health care expenditures are hypothesized to be a function of income and other non-income variables.
The health care issue figures prominently among the millennium development goals set by the United Nations in September 2000 and signed by nearly 190 countries. Better health outcomes are crucial for improving economic welfare at micro and macro levels. A healthy population is bound to bring higher economic value added [1]. Improved quality of life in any country depends on the availability and accessibility to healthcare facilities at affordable costs [2]. Health expenditure is important for policymakers not only due to health outcome importance but also because of the gradual total health expenditure that has become a major concern [3]. In most countries, a rise in the growth rate of health expenditures and its share in the Gross Domestic Product (GDP) have been observed over time [4].
This increase (since the 1960s) raised concerns of financing this newly extended part of the economy. In light of continued cost pressures and strains on public finances, health systems across the countries are striving to increase the value of money. The financing of health care expenditure is therefore a predominant concern in any country, more so in developing countries where severe budget constraints apply and where health outcomes are not good enough. As the resources are scarce in developing countries, if the Ministry of Health can increase the allocation of budget in the health sector, individual spending as out-of-pocket expenditure is expected to reduce significantly. Therefore, out-of-pocket money expenditures in parallel with governing expenditures to render health services, have become a burning concern for developing countries [5]. That is why over the last couple of decades, it has been a point of debate, both for applied econometricians and health economists to analyze health expenditures and its determinants [6].
Himmelstein & Woolhandler [7] see even more role for health expenditures. They believe that a decline in public health spending can potentially undermine preventive measures and weaken responses to health inequalities and new health threats. Additionally, households with catastrophic health expenditures face challenges in offset by the potentially excessive health expenditure and may have been obliged to reduce consumption of other items [8]. These notions make it clear that health expenditure is not just related to the health sector and policymakers should see more roles for macro variables.
The global financial crisis of 2008 and 2009 has highlighted the significance of the relationship between economic growth rates and government expenditure, in general, and health expenditures in particular [4]. This recent downturn has emphasized the usefulness of macroeconomic analysis of health finance and a systematic approach to the development of the evidence-based policy. A recent OECD (Organization for Economic Co-operation and Development) publication noted that after recent slow GDP growth, public health expenditures continued to rise leading to an increase in the ratio of health expenditures to GDP in many countries [9].
These concepts show that health expenditure is not only important due to health outcomes but also because of macroeconomic matters. Macro variables like real per capita incomes, technological innovation, and the aging of the population are generally considered to exert important influences on the growth of health expenditures [10]. Overwhelmingly, studies find that non-medical factors of health consistently play a substantially larger role than medical factors [11]. The literature is full of studies dating back to the 1970s that indicate that poor social determinants of health are harmful to health both in the short- and long-term. Also, a growing body of literature demonstrates the positive impact of favorable social conditions on health outcomes. According to Bradley et al. [12], the ratio of social expenditures to health expenditures was significantly associated with better outcomes in infant mortality, life expectancy, and increased potential life years lost, after adjusting for the level of health expenditures and GDP. Analyses of differentials on health care expenditure by socioeconomic and demographic characteristics of a population can contribute towards a better understanding of existing variations and develop appropriate policies and models for new interventions [13].
Powerful drivers of health lie outside the conventional medical care delivery system, so we should not equate investment in clinical care with investment in health. Such policies, although not typically viewed as health policies, have the potential to improve the health and longevity and to reduce health disparities [14]. The best available evidence suggests that a health policy framework addressing macro determinants of health would achieve better population health, less inequality, and lower costs. Bradley and Taylor (2013) argue that residents of nations that have higher ratios of spending on social services than spending on health care services have better health and live longer [15].
Adler et al. (2016) asserted that the existence of health disparities and fluctuations in health and health inequalities in relation to policy-driven changes in social conditions point to the importance of policies that address social determinants. Such policies, although not typically viewed as health policies, have the potential to improve the health and longevity and reduce health disparities [14]. Zaman et al. (2017) found out that total health expenditure is more sensitive to the gross domestic product rather than life expectancy [5]. As David et al. (2017) put it forward, analyses of differentials on health care expenditure by socioeconomic characteristics could contribute towards a better understanding of existing variations in catastrophic health expenditures and impoverishment that could be used to develop appropriate policies and models to new interventions [13].
The trends and determinants of health expenditure in developed countries have been widely examined and revealed that the main determinants of health expenditure growth include income, the aging of the population, and technological progress. Much evidence is found in the contexts of developed nations and very little is seen in the context of developing nations [16]. WHO (December 2011) says the pace of health expenditures growth is different for countries at various levels of economic development. The financing of the internal organizations and political restraints of health care decision-making are country-specific and heterogeneous [17]. As countries become more developed and wealthier, they devote more public resources to health and spend proportionately more on health per capita [4]. So in this article, the homogeneity assumption is put away and developing countries’ determinants are found out. To do so, all credible determinants of health expenditures are mentioned, and eventually, by using the econometrics method, significant variables are determined and their coefficients are estimated. In this way, we can exactly say how much these variables affect health expenditures and answer three questions which have remained unclear about developing countries’ health expenditures:
Is the growth in health expenditures inevitable in these countries?
What are the determinants of health expenditures in developing countries?
Can we suggest any guidelines to deal with health expenditures?
Health expenditures and its determinants have been a point of debate for many reasons. On the one hand, there are in general the important issues of providing health at affordable costs, health expenditure growth, funding this newly extended part of the economy, and the impact of its funding on other sectors. On the other hand, there is, in particular, the necessity to know its determinants to enable policymakers to predict its development, especially in developing countries. Because these countries suffer from budget limitations, health policymakers and health economists should investigate health expenditure determinants and their coefficients to provide affordable health without putting much pressure on other sectors of the economy. Thus, probing health expenditures and its determinants can help governments enforce cost-containment measures, decrease expenditures, provide a better health system by saved money, and have a better understanding of expenditures trends to face future.
2. Methods
To estimate the health expenditures function, we used a panel data method which provides an increased degree of freedom and efficiency and decreases multicollinearity due to having access to more data. Eviews 8, World Bank, and UNDP data are used for this estimation. Iran, Turkey, Azerbaijan, Georgia, Jordan, Lebanon, Malaysia, Mexico, Costa Rica, Venezuela, and Cuba were chosen as crosses. These countries were selected due to having the same HDI (Human Development index). Not only the countries with the same HDI have the same human development (the most recent available comprehensive data for development) but also have the same income, education, and health indexes which are the determinants of health expenditures. All data of these countries have been collected for 5 years, from 2010 until 2014. To find out the determinants of health expenditures, all credible variables in the literature were investigated. There is extensive literature on the determinants of health expenditures. All of these studies have considered the approach of the demand function to specify their models. Specifically, health care expenditures are hypothesized to be a function of income and other non-income variables.
• Income: Studies of health care expenditures have identified “income” as the dominant cause of health care spending as “over 90% of the variance in per capita medical expenditure is explained by variation in per capita GDP” [18].
The non-income factors have also been identified in the literature. So, what may affect the increase in health expenditures are the following:
• The demographic growth: Care consumption and age are linked. Indicators such as the proportion of the young (e.g. under 15 years old) and old people (e.g. above 65 or 75 years old) over the active or total population have been traditionally flagged as important factors in explaining variations of health care expenditure [19, 20]. However, while their effect is undeniable but little evidence exists about the significance of these variables [21].
• The technological progress: Since the works of Manning et al. and Newhouse [18, 22], the rapid technological progress has been known as a factor of supply and demand who explains the growth of health care expenditure. However, because of the difficulty of finding an appropriate proxy for the changes in medical care technology, few studies have attempted to study the relationship between technological progress and health care expenditure. Still, the literature has mentioned several proxies such as the surgical procedures and the number of specific medical equipment, the R&D spending specific to health care [23], life expectancy, and infant mortality [9].
• The role of real prices in determining the demand for health care [21]: Various studies on the determinants of health care services noted that a change in the volume of health expenditures is not sufficient to explain the evolution of the share of expenditure in the GDP. The increase in this price of heath expenditures may result in raising either the quantities of the consumed medical care or the prices of the health sector. The importance of any factor differs from one country to another. However, there is little empirical consensus on the effect of real prices on health care expenditure. This consensus may be explained by the increasing prices of health services compared to other prices since wages in low productivity sectors must keep up with those in high productivity ones. Hartwig [24] reported a positive and statistically significant effect, while Gerdtham et al. [25] reported an insignificant effect. Hartwig [24] asserted that “…we have to recognize that medical care price indices cannot probably be relied on as deflators or explanatory variables”. In other words, given the paucity of data on price, the diverse national schemes of price regulation, and unreliability in measuring the quality of health care in obtaining this medical price index, we decided not to use this variable in this empirical analysis.
• The medical density: It is defined by physicians as per thousand population and used to account for the supply of healthcare. It can be considered one of the causes of the increase in health expenditures [24, 26]. This fact led to the hypothesis of the induced demand, which reflects the excess supply of services due to an increase in demand initiated by patients. Theoretically, induced demand is generated by the monopoly of the medical knowledge of doctors associated with the low sensitivity of patients to prices. The excess supply of care can then contribute to higher health costs depending on different modes of organization of health care systems.
• Institutional factors: The rise of health expenditures could result from considering the institutional factors. Two approaches are used. The first distinguishes the effects of instructions on remuneration. The second distinguishes the effects of the type of national health system (e.g. contractual system or integrated system). According to Mahieu [27], the overall consideration of the specific institutional leads to larger gaps, the time trend is higher for the repayment system (1.52%) compared to the two other systems (0.59% for the integrated system, 0.68% for the contract system). Azizi and Pereira [28] confirmed that expenditure growth is stronger in countries where the method of repayment is dominant.
• Social characteristics: Factors such as the distribution of income, distribution of education, skills, jobs, opportunities, and expectations for the future could affect health expenditures, especially in developing countries as these variables are facing great changes [17, 19].
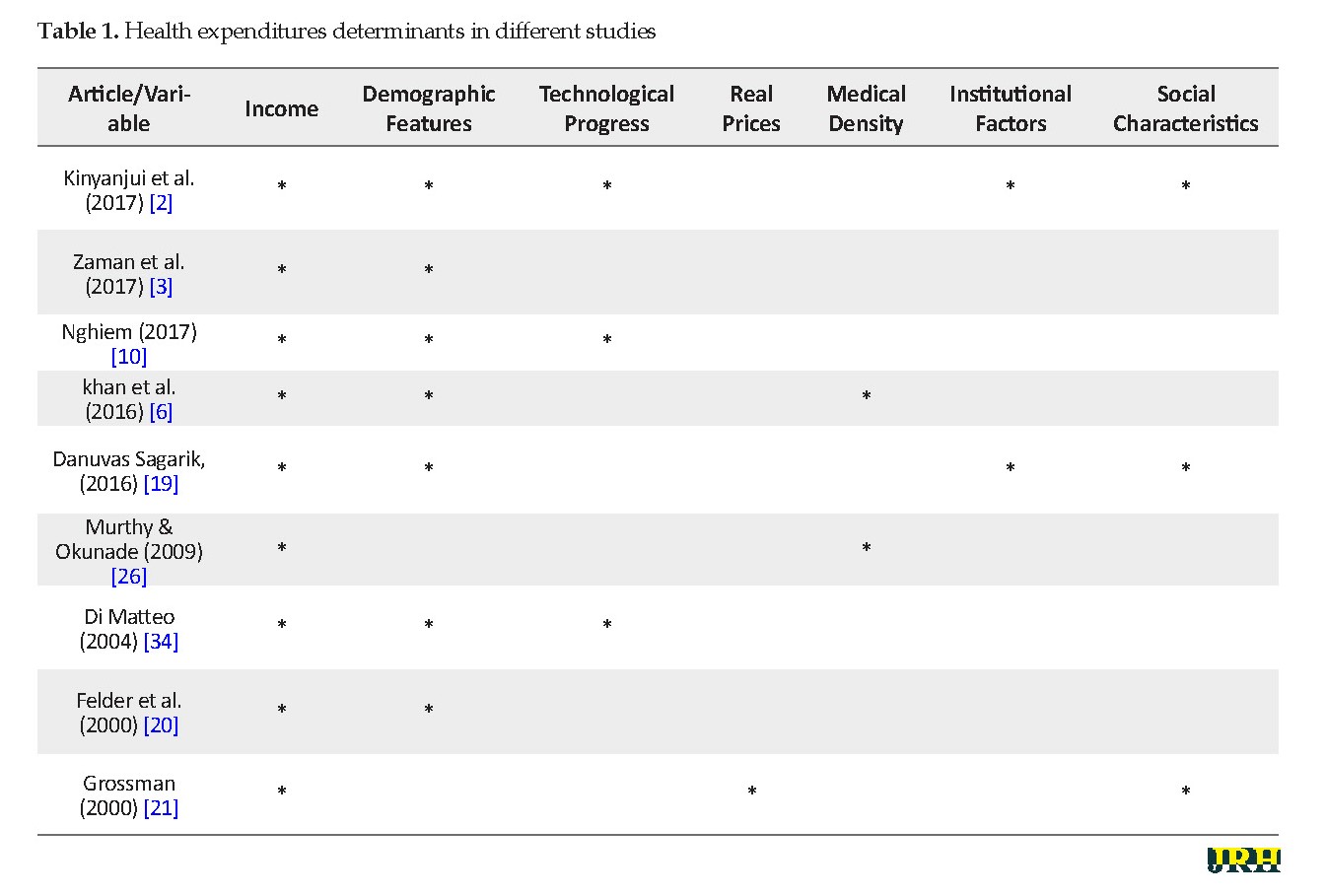
Table 1 summarizes various variables which are described as health expenditures determinants in different studies. The variables used in each article.
Although there are many variables in most studies on this subject, this model is essentially ad hoc and the choice of right-hand-side variables are influenced by the numerous contributions on the possible determinants of health care spending. Especially when the conditions change and health spending accelerates, the main response of governments consists of adopting a series of ad hoc cost containment measures. These measures were applied to both the supply and the demand sides of the market. On the supply side, they included expenditure ceilings through prospective budgets and price controls. On the demand side, they took the form of cost-sharing [29]. Indeed, in all studies, all the possible determinants are discussed but only a few of them that are significant are used in the model. So we have undertaken to examine the influence of specific factors on developing countries’ health expenditures.
3. Results
Data from developing countries reveal that macro variables have the most important effects on health expenditures. That is because, in developing countries, governments have to invest in infrastructures that affect the economy through macro variables. Like other countries all over the world, income is a variable that affects health expenditures. Demographic features, technological progress, and social characteristics were other significant variables in developing countries. Following Following Leu, 1987 [30] ; Cuyler, 1988 [31]; Mao and Xu, 2014 [32]; Ogura, Jakovljevic, 2014 [33]; Khan et al., 2015 [6]; we used old proportion as an index for demographic features, and following Grossman, 2000 [21]; Costa-Font J, Rico A, 2006 [17]; Murthy and Okunade, 2009 [26]; Danuvas Sagarik, 2016 [19]; we used education index for Social characteristics. Technological progress is one of the key factors to explain variations of HCE [34]. However, little attention has been paid to the research in order to study the effects of technological progress on HCE, due to the non-availability of an appropriate proxy to capture variations in the medical care technologies [18].
Innovations in technology were identified in studies as a main contributing factor in increasing health care cost [35] and application of technology in health care always tend to exhibit a positive impact on health expenditure [36], therefore its effects on health expenditures cannot be ignored. According to Hunter PR, Prüss-Ustün A., 2016 [37]; Zaman, K., Ahmad, A., Hamzah, T.A.A.T. et al., 2016 [38]; & G Hutton, L Haller, S Water., 2004 [39] we used improved sanitation facilities as an index for technological progress. In the developing world, sanitation still has considerable public health significance. Specially, During the 1980s and 1990s there was considerable investment in the provision of water supply and sanitation in developing countries. To extend sanitation, further resources are needed to be allocated to this process. And it causes to have significant effect on health expenditures [39]. Most of any health improvement will accrue as sanitation becomes universal [37] and inadequate water sanitation increases the healthcare expenditures [38].
Little attention has been paid to the research to study the effects of technological progress on HCE, due to the non-availability of an appropriate proxy to capture variations in the medical care technologies [18]. Innovations in technology were identified in studies as a main contributing factor in increasing health care cost [35] and the application of technology in health care always tend to exhibit a positive impact on health expenditure [36]; therefore, its effects on health expenditures cannot be ignored. Similar to Hutton, Haller, Water., Hunter, Prüss-Ustün, Zaman, Ahmad, and Hamzah, et al., [37-39], we used improved sanitation facilities as an index for technological progress. In the developing world, sanitation still has considerable public health significance. Specially, During the 1980s and 1990s, considerable investment was done in the provision of water supply and sanitation in developing countries. To extend sanitation, further resources should be allocated to this process that has a significant effect on health expenditures [39]. The health status will improve as sanitation becomes universal [37]but inadequate water sanitation increases healthcare expenditures [38].
Improved sanitation facilities, generally involve better access and safer disposal of excreta (septic tank, pour-flush, simple pit latrine, small-bore sewer, or ventilated improved pit-latrine). Income index is GNI per capita (2011 PPP International $, using natural logarithm) expressed as an index using a minimum value of $100 and a maximum value of $75000. Old proportion refers to the population aged 65 and above as a percentage of the total population. Population is based on the de facto definition of population, which counts all residents regardless of legal status or citizenship. Education index is an average of mean years of schooling (of adults) and expected years of schooling (of children), both expressed as an index obtained by scaling with the corresponding maxima.
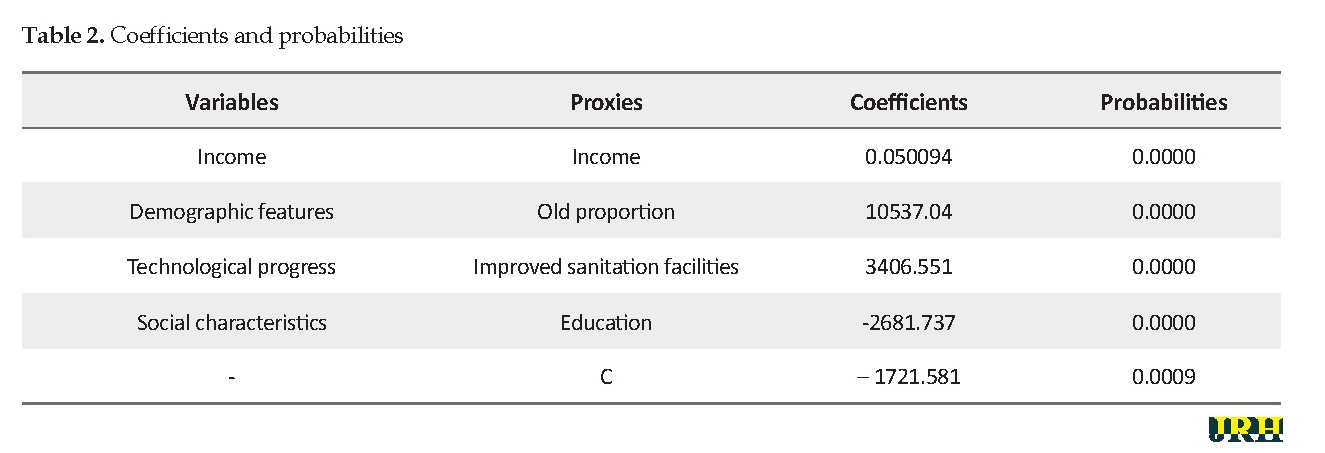
To find out the determinants of health expenditures, a linear model is used as follows: health expenditures = C + β1 income +β2 improved sanitation facilities + β3 education +β4 old proportion. The Chow test rejected the pool hypothesis and the Hausman test asserted that the random effect method should be used. The coefficients resulted from the estimation are presented in Table 2.
The non-income factors have also been identified in the literature. So, what may affect the increase in health expenditures are the following:
• The demographic growth: Care consumption and age are linked. Indicators such as the proportion of the young (e.g. under 15 years old) and old people (e.g. above 65 or 75 years old) over the active or total population have been traditionally flagged as important factors in explaining variations of health care expenditure [19, 20]. However, while their effect is undeniable but little evidence exists about the significance of these variables [21].
• The technological progress: Since the works of Manning et al. and Newhouse [18, 22], the rapid technological progress has been known as a factor of supply and demand who explains the growth of health care expenditure. However, because of the difficulty of finding an appropriate proxy for the changes in medical care technology, few studies have attempted to study the relationship between technological progress and health care expenditure. Still, the literature has mentioned several proxies such as the surgical procedures and the number of specific medical equipment, the R&D spending specific to health care [23], life expectancy, and infant mortality [9].
• The role of real prices in determining the demand for health care [21]: Various studies on the determinants of health care services noted that a change in the volume of health expenditures is not sufficient to explain the evolution of the share of expenditure in the GDP. The increase in this price of heath expenditures may result in raising either the quantities of the consumed medical care or the prices of the health sector. The importance of any factor differs from one country to another. However, there is little empirical consensus on the effect of real prices on health care expenditure. This consensus may be explained by the increasing prices of health services compared to other prices since wages in low productivity sectors must keep up with those in high productivity ones. Hartwig [24] reported a positive and statistically significant effect, while Gerdtham et al. [25] reported an insignificant effect. Hartwig [24] asserted that “…we have to recognize that medical care price indices cannot probably be relied on as deflators or explanatory variables”. In other words, given the paucity of data on price, the diverse national schemes of price regulation, and unreliability in measuring the quality of health care in obtaining this medical price index, we decided not to use this variable in this empirical analysis.
• The medical density: It is defined by physicians as per thousand population and used to account for the supply of healthcare. It can be considered one of the causes of the increase in health expenditures [24, 26]. This fact led to the hypothesis of the induced demand, which reflects the excess supply of services due to an increase in demand initiated by patients. Theoretically, induced demand is generated by the monopoly of the medical knowledge of doctors associated with the low sensitivity of patients to prices. The excess supply of care can then contribute to higher health costs depending on different modes of organization of health care systems.
• Institutional factors: The rise of health expenditures could result from considering the institutional factors. Two approaches are used. The first distinguishes the effects of instructions on remuneration. The second distinguishes the effects of the type of national health system (e.g. contractual system or integrated system). According to Mahieu [27], the overall consideration of the specific institutional leads to larger gaps, the time trend is higher for the repayment system (1.52%) compared to the two other systems (0.59% for the integrated system, 0.68% for the contract system). Azizi and Pereira [28] confirmed that expenditure growth is stronger in countries where the method of repayment is dominant.
• Social characteristics: Factors such as the distribution of income, distribution of education, skills, jobs, opportunities, and expectations for the future could affect health expenditures, especially in developing countries as these variables are facing great changes [17, 19].
Table 1 summarizes various variables which are described as health expenditures determinants in different studies. The variables used in each article.
Although there are many variables in most studies on this subject, this model is essentially ad hoc and the choice of right-hand-side variables are influenced by the numerous contributions on the possible determinants of health care spending. Especially when the conditions change and health spending accelerates, the main response of governments consists of adopting a series of ad hoc cost containment measures. These measures were applied to both the supply and the demand sides of the market. On the supply side, they included expenditure ceilings through prospective budgets and price controls. On the demand side, they took the form of cost-sharing [29]. Indeed, in all studies, all the possible determinants are discussed but only a few of them that are significant are used in the model. So we have undertaken to examine the influence of specific factors on developing countries’ health expenditures.
3. Results
Data from developing countries reveal that macro variables have the most important effects on health expenditures. That is because, in developing countries, governments have to invest in infrastructures that affect the economy through macro variables. Like other countries all over the world, income is a variable that affects health expenditures. Demographic features, technological progress, and social characteristics were other significant variables in developing countries. Following Following Leu, 1987 [30] ; Cuyler, 1988 [31]; Mao and Xu, 2014 [32]; Ogura, Jakovljevic, 2014 [33]; Khan et al., 2015 [6]; we used old proportion as an index for demographic features, and following Grossman, 2000 [21]; Costa-Font J, Rico A, 2006 [17]; Murthy and Okunade, 2009 [26]; Danuvas Sagarik, 2016 [19]; we used education index for Social characteristics. Technological progress is one of the key factors to explain variations of HCE [34]. However, little attention has been paid to the research in order to study the effects of technological progress on HCE, due to the non-availability of an appropriate proxy to capture variations in the medical care technologies [18].
Innovations in technology were identified in studies as a main contributing factor in increasing health care cost [35] and application of technology in health care always tend to exhibit a positive impact on health expenditure [36], therefore its effects on health expenditures cannot be ignored. According to Hunter PR, Prüss-Ustün A., 2016 [37]; Zaman, K., Ahmad, A., Hamzah, T.A.A.T. et al., 2016 [38]; & G Hutton, L Haller, S Water., 2004 [39] we used improved sanitation facilities as an index for technological progress. In the developing world, sanitation still has considerable public health significance. Specially, During the 1980s and 1990s there was considerable investment in the provision of water supply and sanitation in developing countries. To extend sanitation, further resources are needed to be allocated to this process. And it causes to have significant effect on health expenditures [39]. Most of any health improvement will accrue as sanitation becomes universal [37] and inadequate water sanitation increases the healthcare expenditures [38].
Little attention has been paid to the research to study the effects of technological progress on HCE, due to the non-availability of an appropriate proxy to capture variations in the medical care technologies [18]. Innovations in technology were identified in studies as a main contributing factor in increasing health care cost [35] and the application of technology in health care always tend to exhibit a positive impact on health expenditure [36]; therefore, its effects on health expenditures cannot be ignored. Similar to Hutton, Haller, Water., Hunter, Prüss-Ustün, Zaman, Ahmad, and Hamzah, et al., [37-39], we used improved sanitation facilities as an index for technological progress. In the developing world, sanitation still has considerable public health significance. Specially, During the 1980s and 1990s, considerable investment was done in the provision of water supply and sanitation in developing countries. To extend sanitation, further resources should be allocated to this process that has a significant effect on health expenditures [39]. The health status will improve as sanitation becomes universal [37]but inadequate water sanitation increases healthcare expenditures [38].
Improved sanitation facilities, generally involve better access and safer disposal of excreta (septic tank, pour-flush, simple pit latrine, small-bore sewer, or ventilated improved pit-latrine). Income index is GNI per capita (2011 PPP International $, using natural logarithm) expressed as an index using a minimum value of $100 and a maximum value of $75000. Old proportion refers to the population aged 65 and above as a percentage of the total population. Population is based on the de facto definition of population, which counts all residents regardless of legal status or citizenship. Education index is an average of mean years of schooling (of adults) and expected years of schooling (of children), both expressed as an index obtained by scaling with the corresponding maxima.
To find out the determinants of health expenditures, a linear model is used as follows: health expenditures = C + β1 income +β2 improved sanitation facilities + β3 education +β4 old proportion. The Chow test rejected the pool hypothesis and the Hausman test asserted that the random effect method should be used. The coefficients resulted from the estimation are presented in Table 2.
The first and second columns present variables and their proxies. Estimation results revealed that variables that affect health expenditures in developing countries are income, demographic features, social characteristics, and technological progress. The third column presents coefficients that indicate the effects of each determinant on health expenditures. The results show that the effects of the variables of old proportion as a proxy of demographic features, education as a proxy of social characteristics, and improved sanitation as a proxy of technological progress on the health expenditures are 0.050094, 10537.04, -2681.737, and 3406.551, respectively. These show the exact impact of a marginal increase in each of these variables on health expenditures. The last column proves the credibility of the estimation and conveys that all variables are significant.
Results indicate that a demographic feature is the most important variable which affects the health expenditures in developing countries. Technological progress, social characteristics, and income stand at the next footing. Therefore, to answer the second question that we asked in the introduction, we should say that demographic features, technological progress, social characteristics, and income are the determinants of health expenditures in developing countries. Furthermore, the coefficients show the exact effects of changes in any determinants of health expenditures. All variables have positive effects on health expenditures except education which decreases health expenditure so it is rational to urge governments to invest in education or more generally in human capital to contain cost increase. Income has a coefficient that is low and shows that health income elasticity is less than one in developing countries so health is not a luxury good in these countries.
So in these countries, health expenditures increase is not a natural outcome of economic growth rather is a natural consequence of demographic features, technological progress, and social characteristics. All these variables are not under the direct control of the government, especially The Health Ministry. So health expenditures increase is even more imminent. The high coefficients of demographic features and technological progress which is not under the direct control of the government, especially in the countries which usually suffer from lack of budget could be catastrophic without complete preparation. Policymakers should have a comprehensive view of health expenditures to be able to deal with this imminent event. So guidelines that are presented in the next part should be noticed. The answer to the first and third questions in the introduction part is positive. The increase in health expenditures is inevitable and there are some guidelines that we can suggest to deal with health expenditures.
4. Discussion
The results show that health expenditure is not a luxury issue in developing countries and health expenditure growth is not a natural consequence of income growth in these countries. Conventional rationalization attributes this high spending to the nature of the provision of Health Services which incites excessive private consumption at no direct cost to the consumer, who is not constrained by private budgetary considerations [29].
But more specific explanations are also offered, such as: 1. Improvements in high-cost medical technology (both equipment and drugs: OECD, 1977); 2. Increased effectiveness of medical diagnosis and more efficacious treatment, which expand the demand for health care by inducing patients to demand treatment by the latest equipment and method, regardless of cost; 3. The rising share of elderly in the population (from unweighted average 9.25% in 1960 to 13.6% in 1990 in the G7 countries) which is cost increasing; and 4. The spread of insurance that has steadily reduced price to the consumer and driven up demand for medical services. Governments are added to these recommendations that, often for political and social reasons, respond positively to the pressures of demand by increasing public health care spending. Similarly, the private suppliers of health care, who often benefit from tax subsidies, also contribute to the growth of health expenditures by promoting excessive investment and by inducing demand to protect their incomes [40].
In recent years, this growth in health expenditure besides, (i) slow economic growth, (ii) privatization and the trend for a smaller public sector, and (iii) policies to reduce the public sector borrowing and the public debt, have induced countries to adopt policies attempting to contain the rise of health expenditures. Therefore, we highly recommend that governments pursue cost containment measures.
Higher rates of birth and rapid growth of life expectancy in developing countries explain the higher coefficient of old proportion in developing countries. More elderly people increase health expenditure and it would not only jeopardize the feasibility of financing this newly extended part of the economy but also all social security schemes. Greater investments in health care without corresponding economic and tax revenue growth may result in fewer resources for state-funded social services, such as housing, nutrition, and income support programs-which may influence health outcomes in states. Results revealed that not only old proportion but also all determinants of health expenditure in developing countries, i.e. income, education, and improved sanitation facilities are macro variables and are not under the direct control of health sector policymakers.
Therefore, all policymakers in executive and legislative branches of government should participate in health improvement and health expenditures containment. For that matter, health improvement throws other sectors rather than the health sector can achieve better outcomes. This is what health economists and health policy researchers call it health in all policy. Even to the extent that health care investment crowds out social investment, substantial allocation of resources in clinical care may hurt overall health, particularly the health of the socially disadvantaged. Thus, health policies need to expand and address factors outside the medical system that promote or demote health [14].
In this article, these factors were discovered and their effects on health expenditures were estimated. Technological progress is the second determinant of health expenditures in developing countries. Further technologies demand money. In addition, higher life expectancy requires more health expenditure. Elderly population requires extra care and more sophisticated health-care services, which could result in higher health expenditure [3]. Nghiem 2017 [10] believes that technological progress is the main driver for health expenditure. Estimation results do not confirm technological progress as the most important determinant of health expenditure, but it is proved that technological progress is one of the most important determinants of health expenditure. This result is consistent with the studies of Khan et al., Smith et al., and Bodenheimer [6, 35, 36].
Education is the only determinant that decreases health expenditures. Better educational levels are also associated with health expenditure. Education is one of the factors for overcoming the barriers against health system improvement. Low adult literacy rates may interfere with the health improvement process. Information, Education, and Communication (IEC) programs are needed to inform the population, parallel to other preventive and control measures. Income had the least effect on health expenditures. It could be good news for developing countries because these countries due to catch up effects generally have faster income growth rates and this increase in income level will have little effects on rising health expenditures.
Studies show a wide variation in health expenditures with respect to economic development [4, 17]. This finding confirms this article’s method. Countries with higher GDP per capita, as distinct from developing countries, have higher proportions of total health expenditures financed from public sources because these countries by virtue of their high GDP per capita are more developed and have more sustainable public financing as a result of their more reliable revenue base [4]. Long-term care is provided by hospitals in some countries, by residential care in some others, and at home by some other countries.
As it is clarified in this article, these cross-country differences cause distinct results for distinct countries due to different development level and therefore, country-specific and heterogeneous differences according to development level should be taken into account [17]. Sandra Hopkins [4] says a variation of health expenditures from the norm is encountered with differences in institutional development. The more important point than the cause of this heterogeneity between developed and developing countries is its existence that is undeniable. This issue proves that determinants of health expenditure in developed and developing countries are distinct due to the different development levels.
5. Conclusion
Health care cost containment is not under the direct control of the government. This explains why in three decades of health care provision, health expenditures have continued to rise rapidly in developed countries. It is also remarkable that in developing countries, macro variables are the most important determinants of health expenditures. So it is reasonable to say that policymakers should invest more in human capital to enhance health care education with consequential benefits. Donor funding also should be noticed in developing countries to finance this sector.
There are also some organizational forms and payments systems which seem to function well from an expenditure and health outcomes viewpoint in some countries, such as GP (general practitioner) gatekeeper arrangements, but at the end, we should notice that nowadays it is obvious there is no magical formula for health system design.
Future work should include supplying side determinants of health expenditures. We should also take account of a possible structural break, particularly for the relative price of health care. It is also possible to examine expenditure spillovers across the geography of the country and the influence of the political ideology of parties involved in health care decision-making. A larger data set may also be beneficial in future research.
Ethical Considerations
Compliance with ethical guidelines
This study is based on the thesis with code number 2529989 which is approved on 20/12/2016 at Tarbiat Modares University and its publication is ethically confirmed.
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Study design, data collection and analysis, and manuscript preparation: Hamidreza Hajibabaei, Hosein Sadeghi; Presenting resources, consulting, sketching outline: Sajjad Faraji Dizaji, Alimohammad Ahmadi.
Conflict of interest
The authors declared no conflict of interest.
References:
Jaunky VC, Khadaroo AJ. Health care expenditure and gdp: An african perspective. Appl Econ Int Dev. 2008; 8(1):1. https://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=1&cad=rja&uact=8&ved=2ahUKEwjcy.
Kinyanjui D, Kimani D, Kinyanjui B. Determinants and distribution of catastrophic health expenditures and impoverishment in Kenya. J Public Health Res. 2017; 7(3):55-61.
Zaman S, Hossain N, Mehta V, Sharmin S, & Mahmood S. An association of total health expenditure with GDP and life expectancy. J Med Res Innov. 2017; 1(2):AU7-AU12. [DOI:10.15419/jmri.72]
Hopkins S. Health expenditure comparisons: Low, middle and high income countries. Open Health Serv Policy J. 2010;3:111-117. https://pdfs.semanticscholar.org/53e6/ccd75f6c1c87548d571f565798dddb5a2c65.pdf.
Zaman S, Hossain N. Universal health coverage: A burning need for developing countries. J Med Res Innov. 2017; 1(1):18-20. [DOI:10.15419/jmri.41]
Khan HN, Razali RB, Shafie AB. Modeling determinants of health expenditures in Malaysia: Evidence from time series analysis. Front Pharmacol. 2016; 7:69. [DOI:10.3389/fphar.2016.00069]
Himmelstein DU, Woolhandler S. Public health’s falling share of US health spending. Am J Public Health. 2016; 106(1):56-70. [DOI:10.2105/AJPH.2015.302908] [PMID] [PMCID]
Kim Y, Yang B. Relationship between catastrophic health expenditures and household incomes and expenditure patterns in South Korea. Health Policy. 2011; 100(2-3):239-46. [DOI:10.1016/j.healthpol.2010.08.008] [PMID]
Dreger C, Reimers H-E. Health care expenditures in OECD countries: A panel unit root and cointegration analysis. IZA 2005; Discussion Paper Series No. 1469. https://www.researchgate.net/publication/4811198_Health_Care_Expenditures_in_OECD_Countries_A_Panel_Unit_Root_and_Cointegration_Analysis
Nghiem SH, Connelly LB. Convergence and determinants of health expenditures in OECD countries. Health Econ Rev. 2017; 7(1):29. [DOI:10.1186/s13561-017-0164-4] [PMID] [PMCID]
Taylor LA, Tan AX, Coyle CE, et al. Leveraging the social determinants of health: What works? PLoS ONE. 2016; 11(8):e0160217. [DOI:10.1371/journal.pone.0160217] [PMID] [PMCID]
Bradley EH, Elkins BR, Herrin J, Elbel B. Health and social services expenditures: associations with health outcomes. BMJ Qual Saf. 2011; 20(10):826-31. [DOI:10.1136/bmjqs.2010.048363] [PMID]
David N, Kimani D, Kinyanjui B. Determinants and Distribution of Catastrophic Health Expenditures and Impoverishment in Kenya. Public Health Res. 2017; 7(3):5561.
Adler NE, Cutler DM., Jonathan JE., Galea S, Glymour M, Koh HK, et al. Addressing Social Determinants of Health and Health Disparities. Discussion Paper, Vital Directions for Health and Health Care Series. Washington, DC.: National Academy of Medicine; 2016. [DOI:10.31478/201609t]
Bradley E, Taylor L. The American health care paradox: Why spending more is getting us less. New York: Public Affairs; 2013.
Sinha R, Chatterjee K, Nair N, Tripathy P. Determinants of out-of-pocket and catastrophic health expenditure: A Cross-sectional Study. British J Med & Med Res. 2016; 11(8):1-11. [DOI:10.9734/BJMMR/2016/21470]
Costa-Font J, Rico A. Devolution and the interregional inequalities in health and healthcare in Spain. Reg Stud. 2006; 40(8):875-87. [DOI:10.1080/00343400600984346]
Newhouse JP. Medical care costs: how much welfare loss? J Econ Perspect. 1992; 6(3):3-21.
Danuvas S. Determinants of health expendituress in ASEAN region: theory and evidence. Millennial Asia. 2016; 7(1):1-19. [DOI:10.1177/0976399615624054.]
Felder S, Meier M, Schmitt H. Health care expenditure in the last months of life. J Health Econ. 2000; 19(5):679-95. [DOI:10.1016/S0167-6296(00)00039-4]
Grossman M. The human capital model. handbook of health economics. Amsterdam: Elsevier 2000. [DOI:10.1016/S1574-0064(00)80166-3]
Manning W, Newhouse J, Duan N, Keeler E, Leibowitz A. Health insurance and the demand for medical care: evidence from a randomized experiment. Am Econ Rev. 1987; 77(3):251-77.
Okunade AA, Murthy VNR. Technology as a “major driver” of health care costs: A cointegration analysis of the Newhouse conjecture. J Health Econ. 2002; 21(1):147-59. [DOI:10.1016/S0167-6296(01)00122-9]
Hartwig J. What drives health care expenditure? Baumol’s model of unbalanced growth revisited. J Health Econ. 2008; 27(3):603-23. [DOI:10.1016/j.jhealeco.2007.05.006] [PMID]
Gerdtham UG, Sogaardb J, Andersson F, Jonsson B. An econometric analysis of health care expenditure: A cross-section study of the OECD countries. J Health Econ. 1992; 11(1):63-84. [DOI:10.1016/0167-6296(92)90025-V]
Murthy VN, Okunade AA. The core determinants of health expenditures in the African context: Some econometric evidence for policy. Health Policy. 2009; 91(1):57-62. [DOI:10.1016/j.healthpol.2008.10.001] [PMID]
Mahieu R. [G2000 / 01 The determinants of health care expenditure: A macroeconomic approach (French)]. Lyon: Document de travail de la DESE numéro; 2000. http://www.epsilon.insee.fr/jspui/bitstream/1/5614/1/g2000-01.pdf
Azizi K, Pereira C. Comparaison internationale des dépenses de santé: une analyse des évolutions dans sept pays (1970-2002). Dossiers Solidarité et Santé 2005; 18:43-60.
Hitiris T. Prescription charges in the United Kingdom: A critical review. United Kingdom: Department of Economics and Related Studies University of York Heslington York; 2000.
Leu RR. “Public and private health services,” in chapter the public-private mix and international health care cost. Oxford: Basil Black well; 1987.
Cuyler AJ. Helath care expenditure in Canada: Myth and reality; past and future. Toronto: Canadian Tax Foundation; 1988. https://www.worldcat.org/title/health-care-expenditures-in-canada-myth-and-reality-past-and-future/oclc/21196440
Mao R, Xu J. Population aging, consumption budget allocation and sectorial growth. China Econ. Rev. 2014; 30:44-65. [DOI:10.1016/j.chieco.2014.05.004]
Ogura S, Jakovljevic M. Health financing constrained by population aging-an opportunity to learn from Japanese experience. Serbian J Exp Clin Res. 2014; 15(4):175-8110.. [DOI:10.2478/sjecr-2014-0022]
Di Matteo L. What drives provincial health expenditures? Can Tax J. 2004; 52(4):1102-20.
Bodenheimer T. High and rising health care costs. Part2: Technologic innovation. Ann Intern Med 2005; 17(142):932-7. [DOI:10.7326/0003-4819-142-11-200506070-00012] [PMID]
Smith S, Newhouse JP, Freeland MS. Income, insurance, and technology: Why does health spending outpace economic growth? Health Aff (Millwood). 2009; 28(5):1276-84. [DOI:10.1377/hlthaff.28.5.1276] [PMID]
Hunter PR, Prüss-Ustün A. Have we substantially underestimated the impact of improved sanitation coverage on child health? A generalized additive model panel analysis of global data on child mortality and malnutrition. PLoS ONE. 2016; (10):e0164571. [DOI:10.1371/journal.pone.0164571] [PMID] [PMCID]
Zaman K, Ahmad A, Hamzah TA, Yusoff MM. Environmental factors affecting health indicators in sub-saharan African countries: Health is wealth. Soc Indic Res. 2016; 129(1):215-28.
Hutton G, Haller L, Water S, World Health Organization. Evaluation of the costs and benefits of water and sanitation improvements at the global level. Geneva, Switzerland: World Health Organization; 2004.
Pruss-Ustun A, Corvalán CF, World Health Organization. Preventing disease through healthy environments: towards an estimate of the environmental burden of disease. Geneva, Switzerland: World Health Organization; 2006.
Results indicate that a demographic feature is the most important variable which affects the health expenditures in developing countries. Technological progress, social characteristics, and income stand at the next footing. Therefore, to answer the second question that we asked in the introduction, we should say that demographic features, technological progress, social characteristics, and income are the determinants of health expenditures in developing countries. Furthermore, the coefficients show the exact effects of changes in any determinants of health expenditures. All variables have positive effects on health expenditures except education which decreases health expenditure so it is rational to urge governments to invest in education or more generally in human capital to contain cost increase. Income has a coefficient that is low and shows that health income elasticity is less than one in developing countries so health is not a luxury good in these countries.
So in these countries, health expenditures increase is not a natural outcome of economic growth rather is a natural consequence of demographic features, technological progress, and social characteristics. All these variables are not under the direct control of the government, especially The Health Ministry. So health expenditures increase is even more imminent. The high coefficients of demographic features and technological progress which is not under the direct control of the government, especially in the countries which usually suffer from lack of budget could be catastrophic without complete preparation. Policymakers should have a comprehensive view of health expenditures to be able to deal with this imminent event. So guidelines that are presented in the next part should be noticed. The answer to the first and third questions in the introduction part is positive. The increase in health expenditures is inevitable and there are some guidelines that we can suggest to deal with health expenditures.
4. Discussion
The results show that health expenditure is not a luxury issue in developing countries and health expenditure growth is not a natural consequence of income growth in these countries. Conventional rationalization attributes this high spending to the nature of the provision of Health Services which incites excessive private consumption at no direct cost to the consumer, who is not constrained by private budgetary considerations [29].
But more specific explanations are also offered, such as: 1. Improvements in high-cost medical technology (both equipment and drugs: OECD, 1977); 2. Increased effectiveness of medical diagnosis and more efficacious treatment, which expand the demand for health care by inducing patients to demand treatment by the latest equipment and method, regardless of cost; 3. The rising share of elderly in the population (from unweighted average 9.25% in 1960 to 13.6% in 1990 in the G7 countries) which is cost increasing; and 4. The spread of insurance that has steadily reduced price to the consumer and driven up demand for medical services. Governments are added to these recommendations that, often for political and social reasons, respond positively to the pressures of demand by increasing public health care spending. Similarly, the private suppliers of health care, who often benefit from tax subsidies, also contribute to the growth of health expenditures by promoting excessive investment and by inducing demand to protect their incomes [40].
In recent years, this growth in health expenditure besides, (i) slow economic growth, (ii) privatization and the trend for a smaller public sector, and (iii) policies to reduce the public sector borrowing and the public debt, have induced countries to adopt policies attempting to contain the rise of health expenditures. Therefore, we highly recommend that governments pursue cost containment measures.
Higher rates of birth and rapid growth of life expectancy in developing countries explain the higher coefficient of old proportion in developing countries. More elderly people increase health expenditure and it would not only jeopardize the feasibility of financing this newly extended part of the economy but also all social security schemes. Greater investments in health care without corresponding economic and tax revenue growth may result in fewer resources for state-funded social services, such as housing, nutrition, and income support programs-which may influence health outcomes in states. Results revealed that not only old proportion but also all determinants of health expenditure in developing countries, i.e. income, education, and improved sanitation facilities are macro variables and are not under the direct control of health sector policymakers.
Therefore, all policymakers in executive and legislative branches of government should participate in health improvement and health expenditures containment. For that matter, health improvement throws other sectors rather than the health sector can achieve better outcomes. This is what health economists and health policy researchers call it health in all policy. Even to the extent that health care investment crowds out social investment, substantial allocation of resources in clinical care may hurt overall health, particularly the health of the socially disadvantaged. Thus, health policies need to expand and address factors outside the medical system that promote or demote health [14].
In this article, these factors were discovered and their effects on health expenditures were estimated. Technological progress is the second determinant of health expenditures in developing countries. Further technologies demand money. In addition, higher life expectancy requires more health expenditure. Elderly population requires extra care and more sophisticated health-care services, which could result in higher health expenditure [3]. Nghiem 2017 [10] believes that technological progress is the main driver for health expenditure. Estimation results do not confirm technological progress as the most important determinant of health expenditure, but it is proved that technological progress is one of the most important determinants of health expenditure. This result is consistent with the studies of Khan et al., Smith et al., and Bodenheimer [6, 35, 36].
Education is the only determinant that decreases health expenditures. Better educational levels are also associated with health expenditure. Education is one of the factors for overcoming the barriers against health system improvement. Low adult literacy rates may interfere with the health improvement process. Information, Education, and Communication (IEC) programs are needed to inform the population, parallel to other preventive and control measures. Income had the least effect on health expenditures. It could be good news for developing countries because these countries due to catch up effects generally have faster income growth rates and this increase in income level will have little effects on rising health expenditures.
Studies show a wide variation in health expenditures with respect to economic development [4, 17]. This finding confirms this article’s method. Countries with higher GDP per capita, as distinct from developing countries, have higher proportions of total health expenditures financed from public sources because these countries by virtue of their high GDP per capita are more developed and have more sustainable public financing as a result of their more reliable revenue base [4]. Long-term care is provided by hospitals in some countries, by residential care in some others, and at home by some other countries.
As it is clarified in this article, these cross-country differences cause distinct results for distinct countries due to different development level and therefore, country-specific and heterogeneous differences according to development level should be taken into account [17]. Sandra Hopkins [4] says a variation of health expenditures from the norm is encountered with differences in institutional development. The more important point than the cause of this heterogeneity between developed and developing countries is its existence that is undeniable. This issue proves that determinants of health expenditure in developed and developing countries are distinct due to the different development levels.
5. Conclusion
Health care cost containment is not under the direct control of the government. This explains why in three decades of health care provision, health expenditures have continued to rise rapidly in developed countries. It is also remarkable that in developing countries, macro variables are the most important determinants of health expenditures. So it is reasonable to say that policymakers should invest more in human capital to enhance health care education with consequential benefits. Donor funding also should be noticed in developing countries to finance this sector.
There are also some organizational forms and payments systems which seem to function well from an expenditure and health outcomes viewpoint in some countries, such as GP (general practitioner) gatekeeper arrangements, but at the end, we should notice that nowadays it is obvious there is no magical formula for health system design.
Future work should include supplying side determinants of health expenditures. We should also take account of a possible structural break, particularly for the relative price of health care. It is also possible to examine expenditure spillovers across the geography of the country and the influence of the political ideology of parties involved in health care decision-making. A larger data set may also be beneficial in future research.
Ethical Considerations
Compliance with ethical guidelines
This study is based on the thesis with code number 2529989 which is approved on 20/12/2016 at Tarbiat Modares University and its publication is ethically confirmed.
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Study design, data collection and analysis, and manuscript preparation: Hamidreza Hajibabaei, Hosein Sadeghi; Presenting resources, consulting, sketching outline: Sajjad Faraji Dizaji, Alimohammad Ahmadi.
Conflict of interest
The authors declared no conflict of interest.
References:
Jaunky VC, Khadaroo AJ. Health care expenditure and gdp: An african perspective. Appl Econ Int Dev. 2008; 8(1):1. https://www.google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=1&cad=rja&uact=8&ved=2ahUKEwjcy.
Kinyanjui D, Kimani D, Kinyanjui B. Determinants and distribution of catastrophic health expenditures and impoverishment in Kenya. J Public Health Res. 2017; 7(3):55-61.
Zaman S, Hossain N, Mehta V, Sharmin S, & Mahmood S. An association of total health expenditure with GDP and life expectancy. J Med Res Innov. 2017; 1(2):AU7-AU12. [DOI:10.15419/jmri.72]
Hopkins S. Health expenditure comparisons: Low, middle and high income countries. Open Health Serv Policy J. 2010;3:111-117. https://pdfs.semanticscholar.org/53e6/ccd75f6c1c87548d571f565798dddb5a2c65.pdf.
Zaman S, Hossain N. Universal health coverage: A burning need for developing countries. J Med Res Innov. 2017; 1(1):18-20. [DOI:10.15419/jmri.41]
Khan HN, Razali RB, Shafie AB. Modeling determinants of health expenditures in Malaysia: Evidence from time series analysis. Front Pharmacol. 2016; 7:69. [DOI:10.3389/fphar.2016.00069]
Himmelstein DU, Woolhandler S. Public health’s falling share of US health spending. Am J Public Health. 2016; 106(1):56-70. [DOI:10.2105/AJPH.2015.302908] [PMID] [PMCID]
Kim Y, Yang B. Relationship between catastrophic health expenditures and household incomes and expenditure patterns in South Korea. Health Policy. 2011; 100(2-3):239-46. [DOI:10.1016/j.healthpol.2010.08.008] [PMID]
Dreger C, Reimers H-E. Health care expenditures in OECD countries: A panel unit root and cointegration analysis. IZA 2005; Discussion Paper Series No. 1469. https://www.researchgate.net/publication/4811198_Health_Care_Expenditures_in_OECD_Countries_A_Panel_Unit_Root_and_Cointegration_Analysis
Nghiem SH, Connelly LB. Convergence and determinants of health expenditures in OECD countries. Health Econ Rev. 2017; 7(1):29. [DOI:10.1186/s13561-017-0164-4] [PMID] [PMCID]
Taylor LA, Tan AX, Coyle CE, et al. Leveraging the social determinants of health: What works? PLoS ONE. 2016; 11(8):e0160217. [DOI:10.1371/journal.pone.0160217] [PMID] [PMCID]
Bradley EH, Elkins BR, Herrin J, Elbel B. Health and social services expenditures: associations with health outcomes. BMJ Qual Saf. 2011; 20(10):826-31. [DOI:10.1136/bmjqs.2010.048363] [PMID]
David N, Kimani D, Kinyanjui B. Determinants and Distribution of Catastrophic Health Expenditures and Impoverishment in Kenya. Public Health Res. 2017; 7(3):5561.
Adler NE, Cutler DM., Jonathan JE., Galea S, Glymour M, Koh HK, et al. Addressing Social Determinants of Health and Health Disparities. Discussion Paper, Vital Directions for Health and Health Care Series. Washington, DC.: National Academy of Medicine; 2016. [DOI:10.31478/201609t]
Bradley E, Taylor L. The American health care paradox: Why spending more is getting us less. New York: Public Affairs; 2013.
Sinha R, Chatterjee K, Nair N, Tripathy P. Determinants of out-of-pocket and catastrophic health expenditure: A Cross-sectional Study. British J Med & Med Res. 2016; 11(8):1-11. [DOI:10.9734/BJMMR/2016/21470]
Costa-Font J, Rico A. Devolution and the interregional inequalities in health and healthcare in Spain. Reg Stud. 2006; 40(8):875-87. [DOI:10.1080/00343400600984346]
Newhouse JP. Medical care costs: how much welfare loss? J Econ Perspect. 1992; 6(3):3-21.
Danuvas S. Determinants of health expendituress in ASEAN region: theory and evidence. Millennial Asia. 2016; 7(1):1-19. [DOI:10.1177/0976399615624054.]
Felder S, Meier M, Schmitt H. Health care expenditure in the last months of life. J Health Econ. 2000; 19(5):679-95. [DOI:10.1016/S0167-6296(00)00039-4]
Grossman M. The human capital model. handbook of health economics. Amsterdam: Elsevier 2000. [DOI:10.1016/S1574-0064(00)80166-3]
Manning W, Newhouse J, Duan N, Keeler E, Leibowitz A. Health insurance and the demand for medical care: evidence from a randomized experiment. Am Econ Rev. 1987; 77(3):251-77.
Okunade AA, Murthy VNR. Technology as a “major driver” of health care costs: A cointegration analysis of the Newhouse conjecture. J Health Econ. 2002; 21(1):147-59. [DOI:10.1016/S0167-6296(01)00122-9]
Hartwig J. What drives health care expenditure? Baumol’s model of unbalanced growth revisited. J Health Econ. 2008; 27(3):603-23. [DOI:10.1016/j.jhealeco.2007.05.006] [PMID]
Gerdtham UG, Sogaardb J, Andersson F, Jonsson B. An econometric analysis of health care expenditure: A cross-section study of the OECD countries. J Health Econ. 1992; 11(1):63-84. [DOI:10.1016/0167-6296(92)90025-V]
Murthy VN, Okunade AA. The core determinants of health expenditures in the African context: Some econometric evidence for policy. Health Policy. 2009; 91(1):57-62. [DOI:10.1016/j.healthpol.2008.10.001] [PMID]
Mahieu R. [G2000 / 01 The determinants of health care expenditure: A macroeconomic approach (French)]. Lyon: Document de travail de la DESE numéro; 2000. http://www.epsilon.insee.fr/jspui/bitstream/1/5614/1/g2000-01.pdf
Azizi K, Pereira C. Comparaison internationale des dépenses de santé: une analyse des évolutions dans sept pays (1970-2002). Dossiers Solidarité et Santé 2005; 18:43-60.
Hitiris T. Prescription charges in the United Kingdom: A critical review. United Kingdom: Department of Economics and Related Studies University of York Heslington York; 2000.
Leu RR. “Public and private health services,” in chapter the public-private mix and international health care cost. Oxford: Basil Black well; 1987.
Cuyler AJ. Helath care expenditure in Canada: Myth and reality; past and future. Toronto: Canadian Tax Foundation; 1988. https://www.worldcat.org/title/health-care-expenditures-in-canada-myth-and-reality-past-and-future/oclc/21196440
Mao R, Xu J. Population aging, consumption budget allocation and sectorial growth. China Econ. Rev. 2014; 30:44-65. [DOI:10.1016/j.chieco.2014.05.004]
Ogura S, Jakovljevic M. Health financing constrained by population aging-an opportunity to learn from Japanese experience. Serbian J Exp Clin Res. 2014; 15(4):175-8110.. [DOI:10.2478/sjecr-2014-0022]
Di Matteo L. What drives provincial health expenditures? Can Tax J. 2004; 52(4):1102-20.
Bodenheimer T. High and rising health care costs. Part2: Technologic innovation. Ann Intern Med 2005; 17(142):932-7. [DOI:10.7326/0003-4819-142-11-200506070-00012] [PMID]
Smith S, Newhouse JP, Freeland MS. Income, insurance, and technology: Why does health spending outpace economic growth? Health Aff (Millwood). 2009; 28(5):1276-84. [DOI:10.1377/hlthaff.28.5.1276] [PMID]
Hunter PR, Prüss-Ustün A. Have we substantially underestimated the impact of improved sanitation coverage on child health? A generalized additive model panel analysis of global data on child mortality and malnutrition. PLoS ONE. 2016; (10):e0164571. [DOI:10.1371/journal.pone.0164571] [PMID] [PMCID]
Zaman K, Ahmad A, Hamzah TA, Yusoff MM. Environmental factors affecting health indicators in sub-saharan African countries: Health is wealth. Soc Indic Res. 2016; 129(1):215-28.
Hutton G, Haller L, Water S, World Health Organization. Evaluation of the costs and benefits of water and sanitation improvements at the global level. Geneva, Switzerland: World Health Organization; 2004.
Pruss-Ustun A, Corvalán CF, World Health Organization. Preventing disease through healthy environments: towards an estimate of the environmental burden of disease. Geneva, Switzerland: World Health Organization; 2006.
Type of Study: Orginal Article |
Subject:
● International Health
Received: 2017/05/29 | Accepted: 2020/06/24 | Published: 2020/07/1
Received: 2017/05/29 | Accepted: 2020/06/24 | Published: 2020/07/1
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |