Volume 11, Issue 4 (Jul & Aug 2021)
J Research Health 2021, 11(4): 275-284 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Pourseyyed Mohammad M, Naderi F, Ehteshamzadeh P, Asgari P. The Relationship Between Mother-Child Interaction and Spiritual Well-being and Child Behavioral Disorders Through the Moderating Role of Mental Health in Mothers of Children With Hearing Impairment. J Research Health 2021; 11 (4) :275-284
URL: http://jrh.gmu.ac.ir/article-1-1923-en.html
URL: http://jrh.gmu.ac.ir/article-1-1923-en.html
1- Department of Psychology, Ahvaz Branch, Islamic Azad University, Ahvaz, Iran.
2- Department of Psychology, Ahvaz Branch, Islamic Azad University, Ahvaz, Iran. , naderifa2@gmail.com
2- Department of Psychology, Ahvaz Branch, Islamic Azad University, Ahvaz, Iran. , naderifa2@gmail.com
Keywords: Hearing impairment, Mental health, Child-mother interaction, Spiritual and mental disorders
Full-Text [PDF 771 kb]
(476 Downloads)
| Abstract (HTML) (1609 Views)
Full-Text: (638 Views)
1. Introduction
Partial Hearing (PH) and Hard-of-Hearing (HOH) are the most obvious sensorineural defects in humans. There is evidence that 7 per 1000 adults suffer from severe or profound PH and 1 per 750 children have a dominant bilateral hearing impairment (greater than 40 dB) [1]. Severe and profound PH is associated with negative developmental consequences in communicative, cognitive, and social-emotional areas of the life of deaf children and their parents [2]. However, the type and intensity of consequences are influenced by the level of Hearing Loss (HL), hearing functionality via a hearing aid or cochlear implement, parental resources, task sharing in family, Intelligence Quotient (IQ), multiple disabilities, level of disability, and educational efforts [3].
HL can be recognized based on the presence of certain symptoms, known as syndromic hearing, or can be diagnosed based on the presence of the disease without causing any symptoms, known as non-syndromic HL [4] because children with PH or HOH fail to control or manipulate their surrounding environment, they are unable to fulfill their demands or carry them out to attract attention, and are likely to display symptoms of behavioral disorders due to starvation, tiredness, and sadness [5]. Children with HOH experience more severe behavioral disorders and more slowly behavioral improvement than their peers with normal hearing [6]. Behavioral disorders have a higher incidence in the second year of children’s life, typically when they start to learn the language and are good at understanding speech but not at present the words. Assuming the language delay in the majority of children with PH or HOH, anger and frustration can be expected from them due to the lack of connection with their thoughts or feelings or feeling of confusion when they fail to reach parents’ expectations [7].
Many variables affect the behavioral disorders in HOH children, including mother-child interaction. Bratton & Landreth introduced the Child-Parent Relationship Therapy (CPRT) model [8]. The mother-child interaction plays a major role in different domains of mother-child relations; for example, gaining acceptance and understanding of mothers about their children [9]. Different aspects of family life, including emotional, social, or economic aspects are strongly affected by a disability of a child, especially a hearing problem. Parents often respond to the child’s problem by denying reality, avoiding the acceptance of the hearing problem, displaying aggression leading to developing depression and feeling guilty in the child [10]. In turn, the lack of internal adaptation of the parents fades and evokes their feeling of responsibility about their children; however, parents are not properly aware of such responsibility, the child disability causes disrupted mother-child interactions and affects the child’s characteristics [11]. In this situation, they encounter the extra needs of the children arising from their disability.
Many studies on mother-child interaction confirm its association with children’s behavioral disorders [12-19]. Also, many investigations, mothers’ religious beliefs fall into the category of factors affecting child behavioral issues. For instance, in humans, reasonable religious beliefs fulfill a broad range of fundamental needs and fill the moral, spiritual, and emotional gaps [20]. Spiritual well-being in mothers involves being tolerant of stresses in the hearing impairment of their child [21]. Spiritual well-being has two components of spirit and well-being with two aspects, including religious well-being and existential well-being [22, 23]. Religious well-being refers to a relationship with superior power, i.e., God. Existential well-being is defined as a psychosocial factor that explains individual feelings about who am I, what am I doing and why, and where do I belong to. Both aspects encompass transcendence and moving to a superior state [24, 25].
Nevertheless, mother-child interaction and spiritual well-being can influence child behavioral disorders by affecting the mother’s mental health. Typically, HOH is a problem, which faces parents with a variety of fundamental challenges regarding caring for children [26]. This sensory problem sometimes causes some affective-emotional issues for mothers, such as mental health problems [27]. Besides, unfulfilled hopes of parents of having a healthy child lead to the incidence of psychological reactions in parents, including shocks, denial, depression, feeling guilty, aggression, distress, anxiety, and feeling of shame, which affect family members’ functionality [28]. Evidence suggests that parents of children with hearing impairment suffer from poor psychological states and experience a high level of stress and mental health issues compared with the parents of children with normal hearing [29]. The association between mothers’ mental health and behavioral disorders of their children has been confirmed in different studies [12, 19, 30-32].
Numerous negative consequences of psychological well-being problems have been widely reported and described by mothers of children with PH or HOH after diagnosis of the children’s disorder. The majority of these mothers were involved in recurrent deep sorrow and prolonged depression [33], and experience confusion, loss, and a considerable degree of hardship. Therefore, it is important to overcome problems the mothers of PH or HOH children are facing, regarding the mothers’ crucial role in promoting the socio-psychological state of the family and the problems and issues caused by the children hearing impairment. Therefore, based on the issues outlined above, the main objective of the current study was to investigate the relationship between mother-child interaction and spiritual well-being and child behavioral disorders through the mediation role of mental health in mothers of children with hearing impairment.
2. Methods
The descriptive correlational study performed used path analysis. The statistical population included 1580 mothers of children with hearing impairment in Tehran in 2019. The sample size was determined using Morgan’s sample size table (n=310 if N> 1600). The samples were selected based on stratified random sampling. To collect the required data, 310 questionnaires based on the research variables were provided to the participants. The inclusion criteria were the age range of 27-48 years, having at least a middle school education, and having no mental disorders. The exclusion criterion was no complete answer to the questions. A total of 284 questionnaires were analyzed following the elimination of incomplete questionnaires.
Research instruments
The Behavior Disorders Questionnaire: The Rutter Children Behavior Questionnaire that is answered by parents is a valid and reliable survey to measure behavior problems in children. The original questionnaire items were increased from 26 to 30 items by adding 6 more items and integrating 2 of them due to their similarities. The questionnaire is rated on a 3-point Likert scale from 0 to 2. The overall score for the questionnaire ranges from 0 to 60. In research by Khodam [34], this questionnaire was standardized and its validity was accepted. Bardideh et al. [35] reported the reliability of this questionnaire equal to 0.94 based on Cronbach’s alpha coefficient. In the present study, Cronbach’s alpha coefficient was 0.86 for the questionnaire.
Child-Parent Interaction Questionnaire: The 33-item Child-Parent Interaction Questionnaire was designed by Pianta in 1994 and measured the parental perceptions of their relationships with children. The questionnaire consists of three components, namely closeness, dependency, and conflict. Scoring the questionnaire is based on a 5-point Likert scale from 1: totally disagree to 5: strongly agree, and the total score of this test is obtained by summing up the scores of 33 questions. The total score of the test was used in the present study. Content validity of the questionnaire was desired according to Abareshi et al. [36] and the total test reliability was 0.86. Kabiri and Kalantari [37] reported a Cronbach’s alpha of 0.82 for the whole questionnaire. In the present study, the reliability of this questionnaire was measured by Cronbach’s alpha that was 0.82 for the entire questionnaire.
The Spiritual Well-being Questionnaire: The Spiritual Well Being Scale (SWBS), designed by Paloutzian and Ellison in 1982, is a 20-item questionnaire, which consists of two subscales, including spiritual well-being and existential well-being. The former subscale measures the relationship with a superior power while the latter, as a social-psychological element, evaluates individuals’ feelings about who they are, what are they doing and why, and where do they belong to. Items are scored on a 6-point Likert scale from 1 (strongly disagree) to 6 (strongly agree). Positively worded items are rated on a 1-6 scale from strongly disagree to strongly agree, respectively. Negatively worded items are reverse-scored (Items 1, 2, 5, 6, 9, 12, 13, 16, and 18). The score of all items is summed as the overall score of the SWBS [38]. Jafari et al. [39] reported a Cronbach’s alpha of 0.81 for the whole questionnaire. In the present study, Cronbach’s alpha coefficient was 0.83 for the questionnaire.
The Mental Health Questionnaire: The mental health questionnaire (SCL-25) consists of 25 items made by Dragatis and Zickelsurak in 1972. Items are rated on a 5-point Likert scale: 1=not at all, 2=a little, 3=some, 4=a lot, and 5=a great deal. The questionnaire consists of 9 subscales on psychiatric symptoms, including physical complaints, obsessional thoughts and acts, interpersonal sensitivity, anxiety, depression, paranoia and psychosis, phobic disorder and hostility, and aggression. The questionnaire asks about patients’ experience of any conditions during the past week. Along with the above-mentioned subscales, the items also mainly assess three dimensions, including phobic disorder symptoms, Global Severity Index (GSI), standard distress index, Positive Symptom Distress Index (PSDI), and Phobic Symptoms Total (PST). The cutoff point of 2.5 was applied to identify the prevalence of psychiatric symptoms in all 9 subscales. The mean cutoff value of 2.5 and higher in each subscale indicates a phobic condition. A cutoff point of 1.3 was applied for the phobic disorder index. In the present study, Cronbach’s alpha coefficient was 0.87 for the questionnaire.
Statistical analyses
Data were analyzed by descriptive and inferential statistics, such as Mean±SD and Pearson correlation coefficient. The path analysis was used to assess the proposed model. SPSS v. 24 and AMOS software was used for analyzing the data.
3. Results
The participants included 284 mothers of children with hearing impairment with the age range of 27-34 (17%), 34-41 (57%), and 41-48 (26%) years. In terms of the level of education, the participants had a middle school degree (49%), diploma (34%), and bachelor’s and master’s degrees (17%). Among these mothers, 60.60% were housewives and 39.40% were employed. Descriptive statistics, including Mean±SD and Pearson correlation coefficient of the research variables, are presented in Table 1.

According to the data of Table 2, the Root Means Square Error Of Approximation (RMSEA=0.502) showed that the initial model required modification. Therefore, the non-significant relationship between mother-child interaction and child behavioral disorders was removed. Figure 1 shows the final model, in which the RMSEA of 0.001, χ2/df of 0.659, and Comparative Fit Index (CFI) of 1.00 indicated a good model fit.

.PNG)
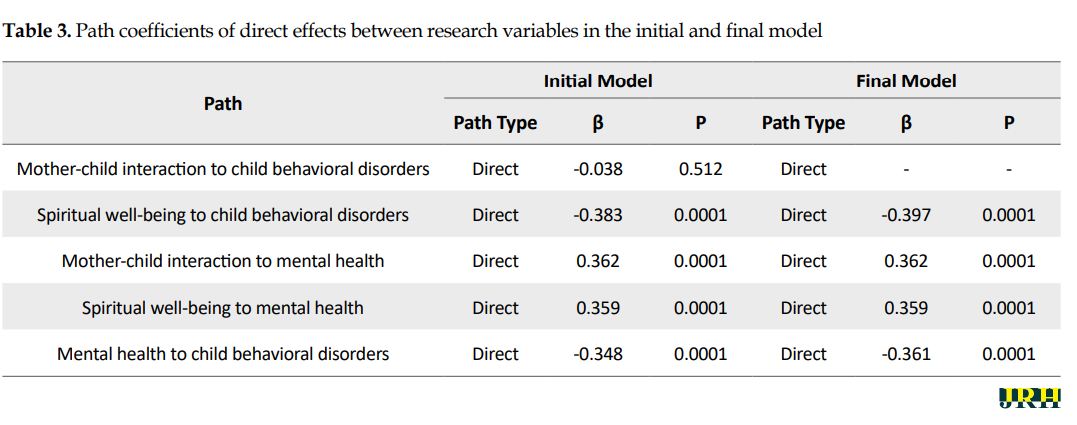
The results showed that the direct effect of spiritual well-being on the child’s behavioral disorders was significant (β=-0.383, P<0.01). Mother-child interaction did not have a significant direct effect on child behavioral disorders (β=-0.038, P>0.05). Moreover, mother-child interaction had a significant direct impact on mental health (β=0.362, P<0.01). The direct effect of spiritual well-being on mental health was significant (β=0.359, P<0.01). However, mental health significantly affected the child behavioral disorders in a direct manner (β=-0.348, P<0.01) (Table 3). The Bootstrap method was used to determine the significance of intermediary relationships.
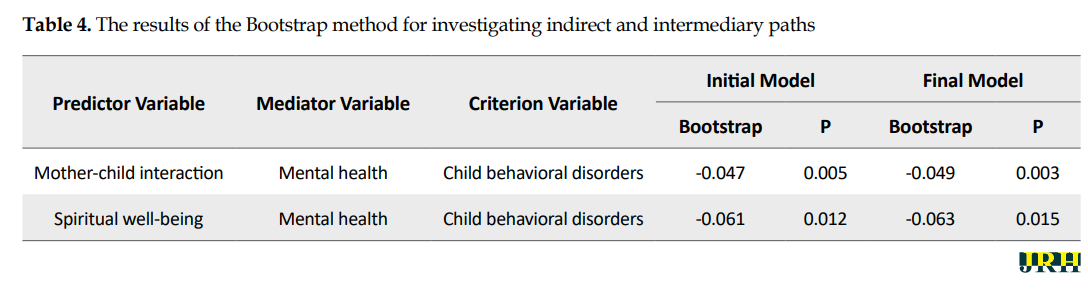
The indirect path of mother-child interaction towards child behavioral disorders was statistically significant according to the mediating role of mental health (β=0.049, P<0.01). Furthermore, the indirect path of spiritual well-being towards child behavioral disorders through the mediating role of mental health was significant (β=-0.063, P<0.05) (Table 4).
4. Discussion
The present study was done to investigate the relationship between mother-child interaction and spiritual well-being and child behavioral disorders through the mediating role of mental health in mothers of children with hearing impairment. All variables that were directly related to children’s behavioral disorders showed significant results except mother-child interaction. Indirect links also showed significant values via a mental health mediation. The results suggest that the proposed model provided a good fit to the data, representing an important step toward the identification of factors influencing the behavioral disorders in children with PH or HOH. The proposed model also offers an appropriate framework for designing a program that prevents the stresses experienced by mothers of PH or HOH children and reduces behavioral disorders in the children.
There was no direct relationship between mother-child interaction and behavioral disorders of children. This finding is inconsistent with the results of previous research [12, 13, 18, 19]. In the above-referenced studies, the association of mother-child interaction with children’s behavioral disorder has been determined via correlation coefficient and regression, and significant values were obtained. The present study, however, performed a link analysis of variables and showed a significant association between mother-child interaction and behavior disorders using Pearson’s correlation test. Yet, the proposed model uses a mediating variable, which defines the strong impact of the mother-child interaction on behavioral disorders (i.e. an indirect link). In other words, mother-child interaction indirectly influenced behavior problems in children. This finding indicates that mother-child interaction plays an indirect role in the behavioral disorders and mental health of their children, which is consistent with the results from prior studies. These investigations used different statistical populations.
The family plays a fundamental role in promoting health and developing an illness and is considered a critical institution to maintain the health of both individuals and society. One of the most significant factors associated with mental and social development is the relationship between parents and children, which also plays an important role during the development. Ineffective disciplinary styles used by parents, as well as inappropriate parent-child interaction, are both related to communicative problems in children, which increases their vulnerability to certain disorders, such as anxiety, behavioral problems, and psychological trauma. A parent-child relationship refers to a combination of unique emotions, behaviors, and expectations, which involves high-quality time, physical affection, and verbal communication between parents and their children.
There was a positive relationship between mother-child interaction and the mental health of children. This finding implies that the interaction between mother and child promotes the mother’s mental health, which is a prerequisite to the quality of mother-child interaction. The interactions between these two refer to the mother’s parenting styles, which are used during mutual interactions. In other words, interaction is a mutual exchange as mothers’ input influences child development and the child’s characteristic indicates the consequences of parenting styles, as well as parent’s communicative patterns and mother’s mental health status [15].
The present study also evidenced a significant positive association between spiritual well-being and children’s behavioral disorders. This implies that the spiritual well-being of mothers plays a major role in behavioral disorders of children as mothers’ beliefs and religious practices help them via providing cognitive, emotional, and physiological solutions to overcome problems and stresses. Besides, the spiritual well-being of mothers contributes to accepting the responsibilities of their thoughts and behaviors for conflicts and struggles, and encourages mothers to change these. Furthermore, from the interpersonal perspective, the spiritual well-being of mothers provides conditions, through which they pay more attention to the existence of God and seek His help during conflicts and sufferings and for their child’s hearing condition. Accordingly, they can cope with difficulties more calmly and solve them. Because spiritual well-being increases the ability to have a relationship with God, it paves the way for mothers to take control of the environment and communicate with others effectively.
Moreover, there was a positive relationship between spiritual well-being and mental health. As mothers’ spiritual well-being increases, their mental health will be improved. This finding is consistent with the results of previous research [39, 40]. Regarding this finding, it should be noted that spiritual well-being increases the ability of self-regulation and the management of negative emotions, such as worry, stress, and anger. Generally speaking, spiritual well-being can have a positive effect on mental health by facilitating more intimate relationships as well as decreasing the conflicts of mothers, who have deaf children, and reduce the conflicts between parents and their children. One of the features of the parents with high spiritual well-being ability is that they have complete attention to their interactions, thoughts, and feelings, wives, and children. Furthermore, they receive these feelings more correctly leading to a decrease in conflicts and disagreements. Therefore, they experience more mental health; on the other hand, the relationship with God and spiritual well-being has a compensatory and interactive role in family member relationships. In general, spirituality is an organized system of beliefs, including the individual’s moral values, which leads to cooperation in the religious community to believe more firmly in God or a superior power [40].
Another finding of this study was a positive relationship between mental health and child behavioral disorders. Therefore, by the improvement of mothers’ mental health, the child’s behavioral disorder will be reduced. This finding is consistent with the results of previous research [12, 19, 30-32]. Mental health implies situations, in which individuals treat environmental and interpersonal desires and requirements appropriately and desirably. One of the sources of making stress in mothers is the deaf child’s birth. These children impose exclusive stress on parents, particularly on mothers.
The most important mothers’ issues and problems are the difficulties to accept the child’s disability, the fatigue resulting from nursing and care, issues related to leisure, family financial problems, and medicine and treatment issues. The high levels of stress of parents are associated with the poor function of the family, child behavioral disorder, and the weak correlation and coherence of communication. Reducing stress is linked to the problem-oriented coping strategy, the desired function of the family, and the sense of meaningfulness in life, which all reduce the child and mother’s suitable interaction and increase their behavioral disorders [30].
In families with deaf children, some factors, such as how to use the coping strategies, the generalization of parental self-efficacy, the cohesion and coherence of the family, and sense of meaningfulness in life affect the weak mother-child interactions and the child’s behavioral disorders. Making mothers aware of their negative feelings and emotions, such as anxiety and stress will also result in improving their mental health and reducing children’s behavioral disorders. These measures can increase the concentration and attention of mothers who have hard of hearing and deaf children; thus, they can keep their calm and get rid of the stress and its consequences.
Also, mental health had a mediating role in the mother-child interaction with child behavioral disorders. To elucidate this finding, we can say that positive mother-child interaction brings them higher mental and physical health. In other words, mother-child appropriate interaction affects the mental health of these mothers and decreases child behavioral disorders. One of the most important factors affecting mental and social development is the relationship between parents and children, which has an important role in the life of the growing child; thereby, the quality of these relationships in the early years of childhood establishes the future cognitive, social, and emotional development [36].
The family has a fundamental role in the health and disease of the family members, and it is the most important institution to maintain the individual and society’s health. Furthermore, it has a profound impact on forming the health and disease concepts and normal and abnormal behavior patterns [14]. Inefficient educational styles and inappropriate parent-child interaction during the development period result in creating problems in the relationship and consequently children’s vulnerability against disorders, such as anxiety, behavioral difficulties, and psychological damages [41].
Another finding of this research was the mediating role of mental health in spiritual well-being and child behavioral disorders. Regarding this finding, it should be noted that the spiritual well-being of mothers while facing environmental stresses, makes more self-control, higher adjustment, a positive attitude toward wife and child, and a more effective relationship with them. On the other hand, studies suggest that high levels of conflicts and low levels of cohesion exist in families with hard of hearing and deaf children. Furthermore, the feeling of inadequacy in parenting over time will extend to the other parts of the private life and marital relationships of the children’s mothers. Thus, it is not far-fetched that families with exceptional children may be affected by the child’s disorders’ symptoms, and parental problems, particularly in mothers is increased. Hence, the importance of spiritual well-being and management of negative affections and emotions become more and more evident. If an individual can acquire such a skill, he/she can be aware of problems and stresses, find proper solutions, and reduce the stressful relationship with his/her child. Furthermore, he/she can achieve an improvement in mental health as well as child behavioral disorders. Consequently, we can argue that mental health has a mediating role in spiritual well-being and child behavioral disorder.
Most of the children’s behavioral problems reflect the complicated interpersonal conditions of the family members, particularly parents. In other words, children’s behavioral problems existence represents defective relationships of family members with each other and it is tightly related to the parents’ wrong educational pattern and their defective interactions with children, as well. Strengthening the spiritual well-being of mothers can increase their mental health and reduce children’s behavioral disorders, subsequently.
5. Conclusion
Spiritual well-being and mental health in mothers had a direct and negative relationship with child behavioral disorders in children with hearing impairment. Spiritual well-being through mental health can have an indirect effect on child behavioral disorders; thus, by strengthening and improving mother-child interaction, spiritual well-being and mental health in mothers can improve the child behavioral disorders of children with hearing impairment. As a result, strengthening the spiritual well-being of mothers can increase their mental health and consequently, reduce children’s behavioral disorders.
Limitations
The statistical population of the research was exceptional children’s mothers in Tehran, which makes it difficult to generalize the results to the other communities. To this end, doing more research on other samples is suggested to generalize the results. Besides, we did not assess children’s fathers; thus, generalization of results to fathers will be difficult. Moreover, similar research should be done on fathers to solve the problem. Furthermore, it is suggested that holding educational workshops to strengthen the spiritual well-being of mothers to boost their trust and mental health and reduce children’s behavioral disorders.
Ethical Considerations
Compliance with ethical guidelines
The study was approved by the Ethical Committee of Islamic Azad University, Ahvaz Branch (Code: IR.IAU.AHVAZ.REC.1399.050).
Funding
This article was extracted from a the PhD. dissertation of the first author at the Department of Psychology, Ahvaz Branch, Islamic Azad University, Ahvaz.
Authors' contributions
Study concept and design, acquisition of data, analysis, and interpretation of data, and statistical analysis: Maryam Pourseyyed Mohammad; Administrative, technical, and material support and study supervision: Farah Naderi; Critical revision of the manuscript for important intellectual content: Parvin Ehteshamzadeh, Parviz Asgari; Approval of the final version: All authors.
Conflict of interest
The authors declared no competing interests.
Refrences:
Partial Hearing (PH) and Hard-of-Hearing (HOH) are the most obvious sensorineural defects in humans. There is evidence that 7 per 1000 adults suffer from severe or profound PH and 1 per 750 children have a dominant bilateral hearing impairment (greater than 40 dB) [1]. Severe and profound PH is associated with negative developmental consequences in communicative, cognitive, and social-emotional areas of the life of deaf children and their parents [2]. However, the type and intensity of consequences are influenced by the level of Hearing Loss (HL), hearing functionality via a hearing aid or cochlear implement, parental resources, task sharing in family, Intelligence Quotient (IQ), multiple disabilities, level of disability, and educational efforts [3].
HL can be recognized based on the presence of certain symptoms, known as syndromic hearing, or can be diagnosed based on the presence of the disease without causing any symptoms, known as non-syndromic HL [4] because children with PH or HOH fail to control or manipulate their surrounding environment, they are unable to fulfill their demands or carry them out to attract attention, and are likely to display symptoms of behavioral disorders due to starvation, tiredness, and sadness [5]. Children with HOH experience more severe behavioral disorders and more slowly behavioral improvement than their peers with normal hearing [6]. Behavioral disorders have a higher incidence in the second year of children’s life, typically when they start to learn the language and are good at understanding speech but not at present the words. Assuming the language delay in the majority of children with PH or HOH, anger and frustration can be expected from them due to the lack of connection with their thoughts or feelings or feeling of confusion when they fail to reach parents’ expectations [7].
Many variables affect the behavioral disorders in HOH children, including mother-child interaction. Bratton & Landreth introduced the Child-Parent Relationship Therapy (CPRT) model [8]. The mother-child interaction plays a major role in different domains of mother-child relations; for example, gaining acceptance and understanding of mothers about their children [9]. Different aspects of family life, including emotional, social, or economic aspects are strongly affected by a disability of a child, especially a hearing problem. Parents often respond to the child’s problem by denying reality, avoiding the acceptance of the hearing problem, displaying aggression leading to developing depression and feeling guilty in the child [10]. In turn, the lack of internal adaptation of the parents fades and evokes their feeling of responsibility about their children; however, parents are not properly aware of such responsibility, the child disability causes disrupted mother-child interactions and affects the child’s characteristics [11]. In this situation, they encounter the extra needs of the children arising from their disability.
Many studies on mother-child interaction confirm its association with children’s behavioral disorders [12-19]. Also, many investigations, mothers’ religious beliefs fall into the category of factors affecting child behavioral issues. For instance, in humans, reasonable religious beliefs fulfill a broad range of fundamental needs and fill the moral, spiritual, and emotional gaps [20]. Spiritual well-being in mothers involves being tolerant of stresses in the hearing impairment of their child [21]. Spiritual well-being has two components of spirit and well-being with two aspects, including religious well-being and existential well-being [22, 23]. Religious well-being refers to a relationship with superior power, i.e., God. Existential well-being is defined as a psychosocial factor that explains individual feelings about who am I, what am I doing and why, and where do I belong to. Both aspects encompass transcendence and moving to a superior state [24, 25].
Nevertheless, mother-child interaction and spiritual well-being can influence child behavioral disorders by affecting the mother’s mental health. Typically, HOH is a problem, which faces parents with a variety of fundamental challenges regarding caring for children [26]. This sensory problem sometimes causes some affective-emotional issues for mothers, such as mental health problems [27]. Besides, unfulfilled hopes of parents of having a healthy child lead to the incidence of psychological reactions in parents, including shocks, denial, depression, feeling guilty, aggression, distress, anxiety, and feeling of shame, which affect family members’ functionality [28]. Evidence suggests that parents of children with hearing impairment suffer from poor psychological states and experience a high level of stress and mental health issues compared with the parents of children with normal hearing [29]. The association between mothers’ mental health and behavioral disorders of their children has been confirmed in different studies [12, 19, 30-32].
Numerous negative consequences of psychological well-being problems have been widely reported and described by mothers of children with PH or HOH after diagnosis of the children’s disorder. The majority of these mothers were involved in recurrent deep sorrow and prolonged depression [33], and experience confusion, loss, and a considerable degree of hardship. Therefore, it is important to overcome problems the mothers of PH or HOH children are facing, regarding the mothers’ crucial role in promoting the socio-psychological state of the family and the problems and issues caused by the children hearing impairment. Therefore, based on the issues outlined above, the main objective of the current study was to investigate the relationship between mother-child interaction and spiritual well-being and child behavioral disorders through the mediation role of mental health in mothers of children with hearing impairment.
2. Methods
The descriptive correlational study performed used path analysis. The statistical population included 1580 mothers of children with hearing impairment in Tehran in 2019. The sample size was determined using Morgan’s sample size table (n=310 if N> 1600). The samples were selected based on stratified random sampling. To collect the required data, 310 questionnaires based on the research variables were provided to the participants. The inclusion criteria were the age range of 27-48 years, having at least a middle school education, and having no mental disorders. The exclusion criterion was no complete answer to the questions. A total of 284 questionnaires were analyzed following the elimination of incomplete questionnaires.
Research instruments
The Behavior Disorders Questionnaire: The Rutter Children Behavior Questionnaire that is answered by parents is a valid and reliable survey to measure behavior problems in children. The original questionnaire items were increased from 26 to 30 items by adding 6 more items and integrating 2 of them due to their similarities. The questionnaire is rated on a 3-point Likert scale from 0 to 2. The overall score for the questionnaire ranges from 0 to 60. In research by Khodam [34], this questionnaire was standardized and its validity was accepted. Bardideh et al. [35] reported the reliability of this questionnaire equal to 0.94 based on Cronbach’s alpha coefficient. In the present study, Cronbach’s alpha coefficient was 0.86 for the questionnaire.
Child-Parent Interaction Questionnaire: The 33-item Child-Parent Interaction Questionnaire was designed by Pianta in 1994 and measured the parental perceptions of their relationships with children. The questionnaire consists of three components, namely closeness, dependency, and conflict. Scoring the questionnaire is based on a 5-point Likert scale from 1: totally disagree to 5: strongly agree, and the total score of this test is obtained by summing up the scores of 33 questions. The total score of the test was used in the present study. Content validity of the questionnaire was desired according to Abareshi et al. [36] and the total test reliability was 0.86. Kabiri and Kalantari [37] reported a Cronbach’s alpha of 0.82 for the whole questionnaire. In the present study, the reliability of this questionnaire was measured by Cronbach’s alpha that was 0.82 for the entire questionnaire.
The Spiritual Well-being Questionnaire: The Spiritual Well Being Scale (SWBS), designed by Paloutzian and Ellison in 1982, is a 20-item questionnaire, which consists of two subscales, including spiritual well-being and existential well-being. The former subscale measures the relationship with a superior power while the latter, as a social-psychological element, evaluates individuals’ feelings about who they are, what are they doing and why, and where do they belong to. Items are scored on a 6-point Likert scale from 1 (strongly disagree) to 6 (strongly agree). Positively worded items are rated on a 1-6 scale from strongly disagree to strongly agree, respectively. Negatively worded items are reverse-scored (Items 1, 2, 5, 6, 9, 12, 13, 16, and 18). The score of all items is summed as the overall score of the SWBS [38]. Jafari et al. [39] reported a Cronbach’s alpha of 0.81 for the whole questionnaire. In the present study, Cronbach’s alpha coefficient was 0.83 for the questionnaire.
The Mental Health Questionnaire: The mental health questionnaire (SCL-25) consists of 25 items made by Dragatis and Zickelsurak in 1972. Items are rated on a 5-point Likert scale: 1=not at all, 2=a little, 3=some, 4=a lot, and 5=a great deal. The questionnaire consists of 9 subscales on psychiatric symptoms, including physical complaints, obsessional thoughts and acts, interpersonal sensitivity, anxiety, depression, paranoia and psychosis, phobic disorder and hostility, and aggression. The questionnaire asks about patients’ experience of any conditions during the past week. Along with the above-mentioned subscales, the items also mainly assess three dimensions, including phobic disorder symptoms, Global Severity Index (GSI), standard distress index, Positive Symptom Distress Index (PSDI), and Phobic Symptoms Total (PST). The cutoff point of 2.5 was applied to identify the prevalence of psychiatric symptoms in all 9 subscales. The mean cutoff value of 2.5 and higher in each subscale indicates a phobic condition. A cutoff point of 1.3 was applied for the phobic disorder index. In the present study, Cronbach’s alpha coefficient was 0.87 for the questionnaire.
Statistical analyses
Data were analyzed by descriptive and inferential statistics, such as Mean±SD and Pearson correlation coefficient. The path analysis was used to assess the proposed model. SPSS v. 24 and AMOS software was used for analyzing the data.
3. Results
The participants included 284 mothers of children with hearing impairment with the age range of 27-34 (17%), 34-41 (57%), and 41-48 (26%) years. In terms of the level of education, the participants had a middle school degree (49%), diploma (34%), and bachelor’s and master’s degrees (17%). Among these mothers, 60.60% were housewives and 39.40% were employed. Descriptive statistics, including Mean±SD and Pearson correlation coefficient of the research variables, are presented in Table 1.

According to the data of Table 2, the Root Means Square Error Of Approximation (RMSEA=0.502) showed that the initial model required modification. Therefore, the non-significant relationship between mother-child interaction and child behavioral disorders was removed. Figure 1 shows the final model, in which the RMSEA of 0.001, χ2/df of 0.659, and Comparative Fit Index (CFI) of 1.00 indicated a good model fit.

.PNG)
The results showed that the direct effect of spiritual well-being on the child’s behavioral disorders was significant (β=-0.383, P<0.01). Mother-child interaction did not have a significant direct effect on child behavioral disorders (β=-0.038, P>0.05). Moreover, mother-child interaction had a significant direct impact on mental health (β=0.362, P<0.01). The direct effect of spiritual well-being on mental health was significant (β=0.359, P<0.01). However, mental health significantly affected the child behavioral disorders in a direct manner (β=-0.348, P<0.01) (Table 3). The Bootstrap method was used to determine the significance of intermediary relationships.

The indirect path of mother-child interaction towards child behavioral disorders was statistically significant according to the mediating role of mental health (β=0.049, P<0.01). Furthermore, the indirect path of spiritual well-being towards child behavioral disorders through the mediating role of mental health was significant (β=-0.063, P<0.05) (Table 4).

4. Discussion
The present study was done to investigate the relationship between mother-child interaction and spiritual well-being and child behavioral disorders through the mediating role of mental health in mothers of children with hearing impairment. All variables that were directly related to children’s behavioral disorders showed significant results except mother-child interaction. Indirect links also showed significant values via a mental health mediation. The results suggest that the proposed model provided a good fit to the data, representing an important step toward the identification of factors influencing the behavioral disorders in children with PH or HOH. The proposed model also offers an appropriate framework for designing a program that prevents the stresses experienced by mothers of PH or HOH children and reduces behavioral disorders in the children.
There was no direct relationship between mother-child interaction and behavioral disorders of children. This finding is inconsistent with the results of previous research [12, 13, 18, 19]. In the above-referenced studies, the association of mother-child interaction with children’s behavioral disorder has been determined via correlation coefficient and regression, and significant values were obtained. The present study, however, performed a link analysis of variables and showed a significant association between mother-child interaction and behavior disorders using Pearson’s correlation test. Yet, the proposed model uses a mediating variable, which defines the strong impact of the mother-child interaction on behavioral disorders (i.e. an indirect link). In other words, mother-child interaction indirectly influenced behavior problems in children. This finding indicates that mother-child interaction plays an indirect role in the behavioral disorders and mental health of their children, which is consistent with the results from prior studies. These investigations used different statistical populations.
The family plays a fundamental role in promoting health and developing an illness and is considered a critical institution to maintain the health of both individuals and society. One of the most significant factors associated with mental and social development is the relationship between parents and children, which also plays an important role during the development. Ineffective disciplinary styles used by parents, as well as inappropriate parent-child interaction, are both related to communicative problems in children, which increases their vulnerability to certain disorders, such as anxiety, behavioral problems, and psychological trauma. A parent-child relationship refers to a combination of unique emotions, behaviors, and expectations, which involves high-quality time, physical affection, and verbal communication between parents and their children.
There was a positive relationship between mother-child interaction and the mental health of children. This finding implies that the interaction between mother and child promotes the mother’s mental health, which is a prerequisite to the quality of mother-child interaction. The interactions between these two refer to the mother’s parenting styles, which are used during mutual interactions. In other words, interaction is a mutual exchange as mothers’ input influences child development and the child’s characteristic indicates the consequences of parenting styles, as well as parent’s communicative patterns and mother’s mental health status [15].
The present study also evidenced a significant positive association between spiritual well-being and children’s behavioral disorders. This implies that the spiritual well-being of mothers plays a major role in behavioral disorders of children as mothers’ beliefs and religious practices help them via providing cognitive, emotional, and physiological solutions to overcome problems and stresses. Besides, the spiritual well-being of mothers contributes to accepting the responsibilities of their thoughts and behaviors for conflicts and struggles, and encourages mothers to change these. Furthermore, from the interpersonal perspective, the spiritual well-being of mothers provides conditions, through which they pay more attention to the existence of God and seek His help during conflicts and sufferings and for their child’s hearing condition. Accordingly, they can cope with difficulties more calmly and solve them. Because spiritual well-being increases the ability to have a relationship with God, it paves the way for mothers to take control of the environment and communicate with others effectively.
Moreover, there was a positive relationship between spiritual well-being and mental health. As mothers’ spiritual well-being increases, their mental health will be improved. This finding is consistent with the results of previous research [39, 40]. Regarding this finding, it should be noted that spiritual well-being increases the ability of self-regulation and the management of negative emotions, such as worry, stress, and anger. Generally speaking, spiritual well-being can have a positive effect on mental health by facilitating more intimate relationships as well as decreasing the conflicts of mothers, who have deaf children, and reduce the conflicts between parents and their children. One of the features of the parents with high spiritual well-being ability is that they have complete attention to their interactions, thoughts, and feelings, wives, and children. Furthermore, they receive these feelings more correctly leading to a decrease in conflicts and disagreements. Therefore, they experience more mental health; on the other hand, the relationship with God and spiritual well-being has a compensatory and interactive role in family member relationships. In general, spirituality is an organized system of beliefs, including the individual’s moral values, which leads to cooperation in the religious community to believe more firmly in God or a superior power [40].
Another finding of this study was a positive relationship between mental health and child behavioral disorders. Therefore, by the improvement of mothers’ mental health, the child’s behavioral disorder will be reduced. This finding is consistent with the results of previous research [12, 19, 30-32]. Mental health implies situations, in which individuals treat environmental and interpersonal desires and requirements appropriately and desirably. One of the sources of making stress in mothers is the deaf child’s birth. These children impose exclusive stress on parents, particularly on mothers.
The most important mothers’ issues and problems are the difficulties to accept the child’s disability, the fatigue resulting from nursing and care, issues related to leisure, family financial problems, and medicine and treatment issues. The high levels of stress of parents are associated with the poor function of the family, child behavioral disorder, and the weak correlation and coherence of communication. Reducing stress is linked to the problem-oriented coping strategy, the desired function of the family, and the sense of meaningfulness in life, which all reduce the child and mother’s suitable interaction and increase their behavioral disorders [30].
In families with deaf children, some factors, such as how to use the coping strategies, the generalization of parental self-efficacy, the cohesion and coherence of the family, and sense of meaningfulness in life affect the weak mother-child interactions and the child’s behavioral disorders. Making mothers aware of their negative feelings and emotions, such as anxiety and stress will also result in improving their mental health and reducing children’s behavioral disorders. These measures can increase the concentration and attention of mothers who have hard of hearing and deaf children; thus, they can keep their calm and get rid of the stress and its consequences.
Also, mental health had a mediating role in the mother-child interaction with child behavioral disorders. To elucidate this finding, we can say that positive mother-child interaction brings them higher mental and physical health. In other words, mother-child appropriate interaction affects the mental health of these mothers and decreases child behavioral disorders. One of the most important factors affecting mental and social development is the relationship between parents and children, which has an important role in the life of the growing child; thereby, the quality of these relationships in the early years of childhood establishes the future cognitive, social, and emotional development [36].
The family has a fundamental role in the health and disease of the family members, and it is the most important institution to maintain the individual and society’s health. Furthermore, it has a profound impact on forming the health and disease concepts and normal and abnormal behavior patterns [14]. Inefficient educational styles and inappropriate parent-child interaction during the development period result in creating problems in the relationship and consequently children’s vulnerability against disorders, such as anxiety, behavioral difficulties, and psychological damages [41].
Another finding of this research was the mediating role of mental health in spiritual well-being and child behavioral disorders. Regarding this finding, it should be noted that the spiritual well-being of mothers while facing environmental stresses, makes more self-control, higher adjustment, a positive attitude toward wife and child, and a more effective relationship with them. On the other hand, studies suggest that high levels of conflicts and low levels of cohesion exist in families with hard of hearing and deaf children. Furthermore, the feeling of inadequacy in parenting over time will extend to the other parts of the private life and marital relationships of the children’s mothers. Thus, it is not far-fetched that families with exceptional children may be affected by the child’s disorders’ symptoms, and parental problems, particularly in mothers is increased. Hence, the importance of spiritual well-being and management of negative affections and emotions become more and more evident. If an individual can acquire such a skill, he/she can be aware of problems and stresses, find proper solutions, and reduce the stressful relationship with his/her child. Furthermore, he/she can achieve an improvement in mental health as well as child behavioral disorders. Consequently, we can argue that mental health has a mediating role in spiritual well-being and child behavioral disorder.
Most of the children’s behavioral problems reflect the complicated interpersonal conditions of the family members, particularly parents. In other words, children’s behavioral problems existence represents defective relationships of family members with each other and it is tightly related to the parents’ wrong educational pattern and their defective interactions with children, as well. Strengthening the spiritual well-being of mothers can increase their mental health and reduce children’s behavioral disorders, subsequently.
5. Conclusion
Spiritual well-being and mental health in mothers had a direct and negative relationship with child behavioral disorders in children with hearing impairment. Spiritual well-being through mental health can have an indirect effect on child behavioral disorders; thus, by strengthening and improving mother-child interaction, spiritual well-being and mental health in mothers can improve the child behavioral disorders of children with hearing impairment. As a result, strengthening the spiritual well-being of mothers can increase their mental health and consequently, reduce children’s behavioral disorders.
Limitations
The statistical population of the research was exceptional children’s mothers in Tehran, which makes it difficult to generalize the results to the other communities. To this end, doing more research on other samples is suggested to generalize the results. Besides, we did not assess children’s fathers; thus, generalization of results to fathers will be difficult. Moreover, similar research should be done on fathers to solve the problem. Furthermore, it is suggested that holding educational workshops to strengthen the spiritual well-being of mothers to boost their trust and mental health and reduce children’s behavioral disorders.
Ethical Considerations
Compliance with ethical guidelines
The study was approved by the Ethical Committee of Islamic Azad University, Ahvaz Branch (Code: IR.IAU.AHVAZ.REC.1399.050).
Funding
This article was extracted from a the PhD. dissertation of the first author at the Department of Psychology, Ahvaz Branch, Islamic Azad University, Ahvaz.
Authors' contributions
Study concept and design, acquisition of data, analysis, and interpretation of data, and statistical analysis: Maryam Pourseyyed Mohammad; Administrative, technical, and material support and study supervision: Farah Naderi; Critical revision of the manuscript for important intellectual content: Parvin Ehteshamzadeh, Parviz Asgari; Approval of the final version: All authors.
Conflict of interest
The authors declared no competing interests.
Refrences:
- McLean TJ, Ware RS, Heussler HS, Harris SM, Beswick R. Barriers to engagement in early intervention services by children with permanent hearing loss. Deafness Educ Int. 2019; 21(1):25-39. [DOI:10.1080/14643154.2018.1528745]
- Borders CM, Bock SJ, Giese K, Gardiner-Walsh S, Probst KM. Interventions for students who are deaf/hard of hearing. In: Obiakor FE, Bakken JP, editors. Viewpoints on interventions for learners with disabilities. Bingley: Emerald Publishing Limited; 2018. pp. 75-105. [DOI:10.1108/S0270-401320180000033005]
- Al-Hilawani YA. Hearing and deaf and hard of hearing: A comparison on metacognition, the mooney problem checklist, IQ, and gender. Volta Rev. 2017; 116(1-2):5-28. [DOI:10.17955/tvr.116.1.2.759]
- Millen K, Dorn B, Luckner JL. Friendships and self-determination among students who are deaf or hard of hearing. Am Ann Deaf. 2019; 163(5):576-95. [DOI:10.1353/aad.2019.0004]
- Benner GJ, Kutash K, Nelson JR, Fisher MB. Closing the achievement gap of youth with emotional and behavioral disorders through multi-tiered systems of support. Educ Treat Child. 2013; 36(3):15-29. [DOI:10.1353/etc.2013.0018]
- Bush ML. Behavioral disorders in children with hearing loss. Hearing J. 2019; 72(1):34-5. [DOI:10.1097/01.HJ.0000552753.74488.4e]
- Blackmer AB, Feinstein JA. Management of sleep disorders in children with neurodevelopmental disorders: A review. Pharmacotherapy. 2016; 36(1):84-98. [DOI:10.1002/phar.1686] [PMID]
- Bratton SC, Landreth GL. Child Parent Relationship Therapy (CPRT) treatment manual: A 10-session filial therapy model for training parents. New York: Routledge; 2006. [DOI:10.4324/9780203956793]
- Park S. Relationship between preschool child-mother interaction, child’s health status, health-related quality of life, and social development. Child Health Nurs Res. 2014; 20(4):255-63. [DOI:10.4094/chnr.2014.20.4.255]
- Konijnenberg C, Sarfi M, Melinder A. Mother-child interaction and cognitive development in children prenatally exposed to methadone or buprenorphine. Earl Hum Dev. 2016; 101:91-7. [DOI:10.1016/j.earlhumdev.2016.08.013] [PMID]
- Tzuriel D, Caspi R. Intervention for peer mediation and mother-child interaction: The effects on children’s mediated learning strategies and cognitive modifiability. Contemp Educ Psychol. 2017; 49:302-23. [DOI:10.1016/j.cedpsych.2017.03.005]
- Shiralinia K, Izadi M, Aslani K. [The role of mediators of parenting stress, the quality of mother-child relationship and mental health of mother in the relationship between mindful parenting and behavioral problems of children (Persian)]. Culture Couns. 2019; 10(38):135-46. [DOI:10.1016/j.cedpsych.2017.03.005]
- Sohrabi F, Asadzadeh H, Arabzadeh Z. [Effectiveness of Barkley’s parental education program in reducing the symptoms of oppositional defiant disorder on preschool children (Persian)]. J Sch Psychol Institutions. 2014; 3(2):82-103. http://jsp.uma.ac.ir/article_198_en.html
- Satorian A, Tahmasian K, Ahmadi MR. [The role of parenting dimensions and child-parent relationship in children’s internalized and externalized behavioral problems (Persian)]. J Fam Res. 2017; 12(4):683-705. http://jfr.sbu.ac.ir/article_97463.html?lang=en
- Khanjani Z, Peyamannia B, Hashemi T. [Prediction of quality of interaction mother-child with anxiety disorders in children According to cultural characteristics of Iranian mothers (Persian)]. J New Thought Educ. 2016; 12(2):239-60. [DOI:10.1016/j.cedpsych.2017.03.005]
- Savell SM, Womack SR, Wilson MN, Shaw DS, Dishion TJ. Considering the role of early discrimination experiences and the parent-child relationship in the development of disruptive behaviors in adolescence. Infant Ment Health J. 2019; 40(1):98-112. [DOI:10.1002/imhj.21752] [PMID]
- Oh A, Han M, Choi Y, Lau S, Shum MS. Exploring relationship among child maltreatment experience in childhood and behavior problems as young adults: Role of social support among college students in Hong Kong. Int Soc Work. 2019; 62(2):1011-24. [DOI:10.1177/0020872818762718]
- Ang KQP, Loh PR. Mental health and coping in parents of children with Autism Spectrum Disorder (ASD) in Singapore: An examination of gender role in caring. J Autism Dev Disord. 2019; 49(5):2129-45. [DOI:10.1007/s10803-019-03900-w] [PMID]
- Maiuolo M, Deane FP, Ciarrochi J. Parental authoritativeness, social support and help-seeking for mental health problems in adolescents. J Youth Adolesc. 2019; 48(6):1056-67. [DOI:10.1007/s10964-019-00994-4] [PMID]
- Büssing A, Waßermann U, Christian Hvidt N, Längler A, Thiel M. Spiritual needs of mothers with sick new born or premature infants-A cross sectional survey among German mothers. Women Birth. 2018; 31(2):e89-98. [DOI:10.1016/j.wombi.2017.08.002] [PMID]
- Yeh PM. The influences of family interaction and spiritual well-being on anxiety and depression among older adults in the United States. Health Aging Res. 2018; 7(3):1-8. [DOI:10.12715/har.2018.7.10]
- Shahabizadeh F, Behnamfar MJ. The application of nutritional patterns for developing a model for mental health through resorting to spiritual well-being: A structural equation modeling. J Res Health. 2019; 9(7):639-47. http://jrh.gmu.ac.ir/article-1-1277-en.html
- Siddall PJ, McIndoe L, Austin P, Wrigley PJ. The impact of pain on spiritual well-being in people with a spinal cord injury. Spinal Cord. 2017; 55(1):105-11. [DOI:10.1038/sc.2016.75] [PMID]
- Ahmadi Tahour Soltani M, Zareh H, Mohammadi T, Zoqi Pydar MR. Structural modeling pattern of relationships between goal orientation, hope, spiritual well-being and mental health of students. J Res Health. 2014; 4(4):911-9. http://jrh.gmu.ac.ir/article-1-390-en.html
- Unterrainer HF, Lewis AJ, Fink A. Religious/spiritual well-being, personality and mental health: A review of results and conceptual issues. J Relig Health. 2014; 53(2):382-92. [DOI:10.1007/s10943-012-9642-5] [PMID]
- Piotrowska PJ, Tully LA, Lenroot R, Kimonis E, Hawes D, Moul C. et al. Mothers, fathers, and parental systems: A conceptual model of parental engagement in programmes for child mental health-Connect, Attend, Participate, Enact (CAPE). Clin Child Fam Psychol Rev. 2017; 20(2):146-61. [DOI:10.1007/s10567-016-0219-9] [PMID]
- Akbari Booreng M. Relationship between perception of parental communication styles incompatibility amongst high school students. J Res Health. 2017; 7(3):877-84. http://jrh.gmu.ac.ir/article-1-513-en.html
- Kendig S, Keats JP, Hoffman MC, Kay LB, Miller ES, Moore Simas TA, et al. Consensus bundle on maternal mental health: Perinatal depression and anxiety. J Obstet Gynecol Neonatal Nurs. 2017; 46(2):272-81. [DOI:10.1097/AOG.0000000000001902] [PMID]
- Webb R, Ayers S. Postnatal mental health and mothers’ processing of infant emotion: An eye-tracking study. Anxiety Stress Coping. 2019; 32(5):484-97. [DOI:10.1080/10615806.2019.1620215] [PMID]
- Riahi F, Amini F, Salehi Veisi M. The children’s behavioral problems and their relationship with maternal mental health. J Jahrom Univ Med Sci. 2012; 10(1):46-52. [DOI:10.29252/jmj.10.1.46]
- León-del-Barco B, Mendo-Lázaro S, Polo-del-Río MI, López-Ramos VM. Parental psychological control and emotional and behavioral disorders among Spanish adolescents. Int J Environ Res Public Health. 2019; 16(3):507. [DOI:10.3390/ijerph16030507] [PMID]
- Pruitt MM, Rhoden M, Ekas NV. Relationship between the broad autism phenotype, social relationships and mental health for mothers of children with autism spectrum disorder. Autism. 2018; 22(2):171-80. [DOI:10.1177/1362361316669621] [PMID]
- Kuhn J, Ford K, Dawalt LS. Brief report: Mapping systems of support and psychological well-being of mothers of adolescents with autism spectrum disorders. J Autism Dev Disord. 2018; 48(3):940-6. [DOI:10.1007/s10803-017-3381-0] [PMID]
- Khodam H, Modanloo M, Ziyaie T, Keshtkar, A. Behavioral disorders and related factors in school age children of Gorgan. Iran J Nurs Res. 2009; 4(14):29-37. http://ijnr.ir/article-1-249-en.html
- Bardideh M, Mansor M, Karimpoor M. [Preparation and validation of behavioral disorders in autistic spectrum children (Parent Form) (Persian)]. J manag Syst. 2010; 1(1):15-26. http://jpmm.miau.ac.ir/article_1151.html?lang=en
- Abareshi Z, Tahmasian K, Mazaheri MA, Panaghi L. [The impact of psychosocial Child Development training program, done through improvement of mother-child interaction, on parental self-efficacy and relationship between mother and child under three (Persian)]. J Rese Psychol Health. 2009; 3(3):49-58. https://rph.khu.ac.ir/browse.php?a_id=115&sid=1&slc_lang=en
- Kabiri A, Kalantari M. [The effectiveness of group positive parenting program on parental stress and mother-child interaction of mother of children with nocturnal enuresis (Persian)]. Knowl Res Applied Psychol. 2018; 19(2):115-24. [DOI:10.1007/s10803-017-3381-0]
- Dehshiri GR, Najafi M, Sohrabi F, Taraghijah S. [Development and validation of the Spiritual Well-being Questionnaire among university students (Persian)]. J Psychol Stud. 2013; 9(4):73-98. [DOI:10.1007/s10803-017-3381-0]
- Jafari A, Hajloo N, Faghani R, Khazan K. [The relationship between spiritual well-being, hardiness, and mental health in the elderly (Persian)]. J Res Behav Sci. 2013; 10(6):431-40. http://rbs.mui.ac.ir/article-1-276-en.html
- Akbari Booreng M. Relationship between happiness and homesickness among students: Structural equation modeling. J Res Health. 2019; 9(2):181-6. [DOI:10.29252/jrh.9.2.181]
- Shokoohi-Yekta M, Parand A, Dargahi M.[ Family-based preventive interventions: Effects on parent-child relationship and parenting styles (Persian)]. J Child Ment Health. 2016; 3(2):55-63. http://childmentalhealth.ir/article-1-64-en.html
Type of Study: Orginal Article |
Subject:
● International Health
Received: 2020/12/9 | Accepted: 2021/01/26 | Published: 2021/08/1
Received: 2020/12/9 | Accepted: 2021/01/26 | Published: 2021/08/1
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |








