Volume 13, Issue 3 (May & Jun 2023)
J Research Health 2023, 13(3): 209-218 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Bahmani S, Kraskian Mujemnari A. Comparing Coping Strategies in People Between Inflammatory Bowel Disease and Healthy People in Terms of Health Locus of Control. J Research Health 2023; 13 (3) :209-218
URL: http://jrh.gmu.ac.ir/article-1-2114-en.html
URL: http://jrh.gmu.ac.ir/article-1-2114-en.html
1- Department of Psychology, Faculty of Humanities, Central Tehran Branch, Islamic Azad University, Tehran, Iran. , Sedigheh.bahmani1979@gmail.com
2- Department of Psychology, Faculty of Humanities, Roudehen Branch, Islamic Azad University, Roudehen, Iran.
2- Department of Psychology, Faculty of Humanities, Roudehen Branch, Islamic Azad University, Roudehen, Iran.
Full-Text [PDF 639 kb]
(508 Downloads)
| Abstract (HTML) (1350 Views)
Full-Text: (454 Views)
1. Introduction
Inflammatory bowel disease (IBD) is a group of chronic diseases of the digestive tract with severe symptoms such as urgent diarrhea, abdominal pain, and cramping. Crohn disease (CD) and ulcerative colitis (UC) are the most frequent types of IBD [1]. The pathogenesis of these complex multifactorial diseases has not been fully understood [2]. IBD has a relapsing and remitting phase and manifests with GI symptoms such as diarrhea, nausea, blood in the stool, abdominal pain, sometimes accompanied by joint or skin problems, and fatigue [3]. Complications include intestinal perforations, strictures, and fistulas. Also, anxiety disorders, depression, and bipolar disorder can affect the course of IBD [4].
Many studies have reported the disease’s profound impact on patients’ psychological well-being [5]. The health locus of control also seems to be a psychological construct influencing health and disease. It is an important construct that is less addressed compared to other factors. The health locus of control is a construct based on the control locus concept and social learning theory used in the health area. The health locus of control points out the individuals’ beliefs about factors impacting health [6]. In adults, internal locus of control (LOC) has been associated with positive health outcomes, such as reduced disease burden, increased self-rated health, adherence to treatment, and general health. Conversely, an external LOC indicates that a person believes outside factors such as doctors, other people, or chance determine health outcomes [7].
In the adult population, external LOC has been associated with negative outcomes, such as decreased quality of life, increased emergency department visits, and reduced acceptance of illness [8]. Helvik et al. investigated the relationship between two dimensions of coping (locus of control orientation and coping strategies/ways of coping) and health-related quality of life outcomes in two very different groups of older adults: One hospitalized with depression, the other living in the community without depression. There was no association between emotional- and problem-focused coping strategies and health-related quality-of-life outcomes in the depressed or non-depressed group [8, 9].
Hashemi Razini et al. [10] found a significant relationship between coping skills and locus of control with death anxiety. Emotional and avoidance coping strategies and external locus of control can predict the level of death anxiety [10]. Bjørkløf et al. found that depressed elderly people compared to non-depressed elderly, used more external locus of control [11]. Moreover, they used less problem-oriented coping strategies. Lazarus and Folkman [12] defined stress as a dynamic and mutual relationship between the person and the environment. According to this definition, coping strategies include intellectual, emotional, and behavioral efforts of a person used when facing psychological pressures to overcome, tolerate or minimize the effects of stress [12].
In a study by Polizzi et al. [13], maternal locus control was significantly associated with children’s coping strategies. Furthermore, their findings show positive and negative correlations between specific scales of maternal locus of control and children’s coping styles. Health psychology specialists, doctors, nurses in psychosomatic diseases, and researchers in this field will benefit from this study. IBD patients have several factors that play a role in their lives, especially since the source of health control is a two-dimensional concept [13]. According to previous studies about psychosomatic disorders and IBD, the place of control for coping strategies with stress is because psychosomatic disorders are absent in health psychology research literature. It reports that IBD could have such severe symptoms that the patient is often unaware of its stress roots and cannot cope with them. Therefore, the patient does not seek psychological or even cognitive treatments. Considering these factors and few studies in this field, the researchers assumed that cognitive factors such as problem-oriented and emotion-oriented coping strategies could be predicted and investigated based on internal and external control sources. The question is how a patient copes with and responds to the stress of being diagnosed with and the ongoing effects of IBD. This study aimed to compare the coping strategies of IBD patients and healthy people regarding health locus of control.
2. Methods
The study method was causal-comparative. The study population included all patients with inflammatory bowel disease referred to the Bowel Department of Jam Hospital in Tehran, Iran, from April to September 2020. The research sample included 200 subjects (87 healthy people and 113 people with inflammatory bowel disease) selected by the convenience and purposeful sampling method. Using the G*power tool with α=0.05 and power=80%, a sample size of 186 was determined to study 93 subjects in each group. Yet, considering the probability of loss, the sample size was increased to 200. The inclusion criteria included moderate IBD according to the Rome III criteria based on the diagnosis of a gastroenterologist (score range: 175-300), literacy for reading and writing to fill out questionnaires, age range within 15 to 60 years, access all participants on Instagram, informed consent to participate in the study, organic gastrointestinal disorders approved by a gastroenterologist, and no acute physical illness and psychological disorder under psychiatric treatment. The exclusion criteria were an incomplete questionnaire and the unwillingness to continue the study.
The researcher went to the educational center of the hospital. After obtaining the introduction sheet, he was referred to the treatment department for gastrointestinal diseases, colitis, and Crohn disease and the association of gastrointestinal patients. After obtaining permission from that authority, the researcher went to the center’s departments and coordinated with the department officials. Then, the researcher presented the questionnaires to the patients online through Instagram, and they agreed to answer them. The ethical considerations were getting informed consent from the participants, getting them to fill out the questionnaires, and keeping the information confidential. After coordinating with the authorities, establishing initial communication, and creating a sense of trust regarding the confidentiality of information among the patients and no need to mention names, the questionnaires were distributed. During the questionnaire implementation, more explanations were given if any question was incomprehensible or the patients had difficulty understanding them. Also, the test participation was voluntary and based on the participants’ wishes. After collecting the questionnaires, the raw scores were calculated using the scoring key. SPSS software, version 24 was used to run a two-way multivariate analysis of variance in the data. To test the normality of the data distribution resulting from the measurement of the research variables, we used the Kolmogorov-Smirnov, Levene’s, and Box tests with a significance level greater than 0.05. Additionally, a 2-variable Chi-square test was used to test the homogeneity of the 4 research subgroups in terms of the 3 demographic variables of gender, class, and level of education.
Research tools
The irritable bowel syndrome symptom index
This scale was developed by Francis, Morris, and Horoll and consists of 5 sections that examine the symptoms of IBS, including pain, defecation disorders, bloating, disease effects on daily activities, and extra-intestinal symptoms on an intensity scale [14]. The average score of each section is 100, and the total score of the questionnaire is 500. Mild, moderate, and severe cases are represented with score ranges of 75-175, 175-300, and higher than 300, respectively. The internal correlation coefficient and Cronbach α of the scale are 0.70 in the Iranian version [15].
Multidimensional health locus control
Multidimensional health locus control (MHLC) was first developed by Wallston, Stein, and Smith (1994) to determine the health locus of control [16]. The MHLC is composed of a total of 18 items, including the internal locus of control (items 13, 12, 7, 6, 1, and 17), the chance locus of control (items 15, 11, 9, 4, 2, and 16), and the powerful others locus of control (items 14, 10, 7, 5, 3, and 18). Participants should respond to items on a 6-point Likert scale from 1 to 6 (completely disagree, disagree, slightly disagree, slightly agree, agree, and completely agree). The reliability of this scale was reported by Cronbach α coefficient for internal control components as 0.68, chance control as 0.74, and other control as 0.51 [17]. In Iran, the concurrent validities of the questionnaire were 0.57, 0.49, and 0.53, respectively. The reliability of this scale using the Cronbach α coefficient was acceptable for internal (0.68), powerful others (0.72), and chance (0.66). The test-retest test reliability indices, after a time interval of 4 weeks, were 0.60 for internal, 0.58 for chance, and 0.74 for powerful others [18]. A Cronbach α coefficient of 0.751 was calculated for the MHLC, indicating the validity of the research tool.
Folkman and Lazarus coping strategies inventory
The questionnaire was developed to assess the specific ways in which people cope with stressors. This definition has four key elements. Coping is a process-oriented approach, not static [19]. The first version of “ways of Coping” [18] contained 68 items that were derived from the theoretical framework outlined by Lazarus and his colleagues [12]. The revised 66-item version differs from the original in that redundant and unclear was removed [19]. Further, the response format was changed from “yes-no” to a 4-point Likert scale so that respondents could indicate the frequency with which they use each strategy (0=does not apply and or not used, 1=used somewhat, 2=used quite a bit, 3=used a great deal). All questions are scored with the Likert scale of not at all=0, sometimes=1, quite a bit=2, and very much=3. The questionnaire has 8 subscales: Confrontation, withdrawal, self-control, social support, responsibility acceptance, escape avoidance, problem-solving, and positive reappraisal. Higher scores demonstrate more applications of the coping strategies. Folkman and Lazarus [19] reported Cronbach α coefficient for the social support, escape-avoidance, and problem-solving subscales as 0.76, 0.72, and 0.68, respectively [19]. In Iran, Padyab et al. [20] reported a reliability of 0.88 on the scale [20]. This research tool showed acceptable validity based on Cronbach α coefficient of 0.888.
3. Results
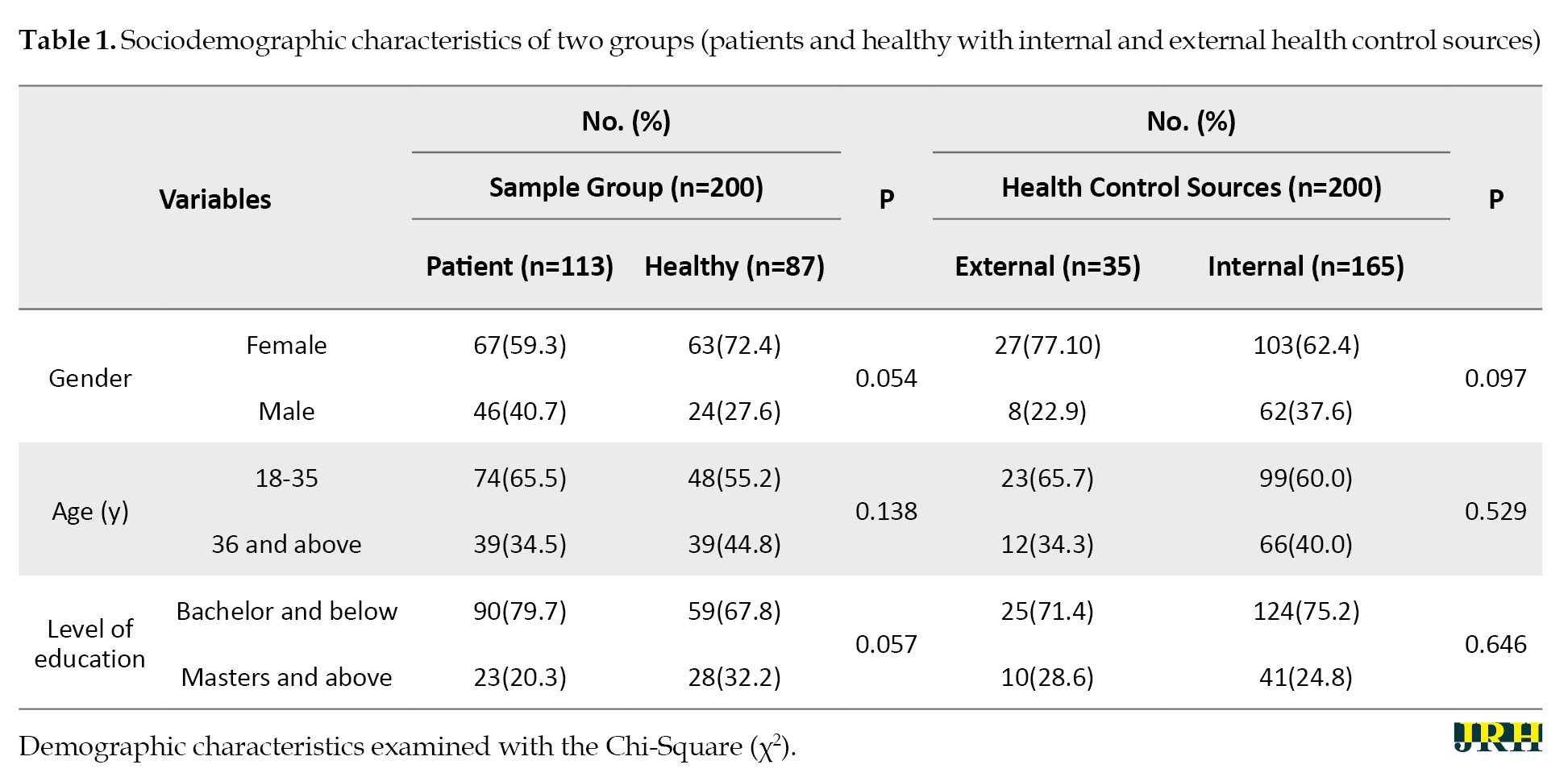
The sociodemographic characteristics of the research included the patients (n=113) and healthy control group (n=87) with internal health control source (n=165) and external health control source (n=35). The results showed 67 females (59.3%) and 46 males (40.7%) were patients. Furthermore, 63 participants (72.4%) were healthy females, and 24(27.6%) were healthy males. The highest patient frequency was found in the 35-35 years age group with n=74 (65.5%), while the lowest was found in patients over 36 years old and above. Thus, patients with bachelor’s degrees and below were more frequent at 79.7%, whereas healthy people were lower frequent at 28(32.2%) with master’s degrees and above (Table 1).
As presented in Table 2, the groups’ significant levels of observed F statistics indicate that between people with health control sources (internal/external), regarding the variables of responsibility, positive reappraisal, and direct copying.

There is a significant difference between social support seeking, escaping-avoiding, social support seeking, continence, and avoiding. Also, the observed F statistics of the control source is significant. This finding indicates a significant difference between people with irritable bowel syndrome and normal people regarding responsibility, positive reappraisal, direct coping, social support seeking, escaping-avoiding, social support seeking, continence, and avoiding. Moreover, the interaction between the group and the source has been significant. Therefore, there is a significant difference between the 4 groups regarding responsibility variables, positive reappraisal, direct confrontation, planning to solve the escape-avoidance problem, seeking social support, refraining, and avoidance (P<0.001). Considering the significance of the difference between the groups and the source of health control, a two-way analysis of variance was performed, the results of which are shown in Table 3.

As seen in Table 3, there is a significant difference between irritable bowel syndrome and normal people (P<0.001). Therefore, according to the results, people with irritable bowel syndrome are significantly higher than normal people in terms of positive reappraisal and responsibility. However, there is no significant difference in other coping strategies between irritable bowel syndrome and normal individuals (P>0.05).
Table 3 shows a significant difference between individuals with the source of internal and external control only regarding volatile variables (P<0.001). However, there is no significant difference between individuals with the source of internal and external control over other coping strategies (P>0.05). Therefore, according to Table 3, people with an internal control source are significantly higher than those with external control sources.
Also, as seen in Table 3, among individuals with irritable and ordinary intestinal syndromes with internal and external control sources, in terms of responsibility variables (P<0.001), positive reappraisal (P=0.004). Avoiding there is a meaningful difference (P<0.001). However, there is no significant difference between people with the irritable and ordinary intestinal syndrome with the source of internal and external control in terms of direct coping variables, searching for social support, and avoiding differences (P>0.05). In other words, the average coping skills in four groups of patients healthy with intestinal inflammation, with an internal and external locus of health control, are statistically the same.
4. Discussion
The study aimed to compare coping strategies in people with inflammatory bowel syndrome and healthy people according to internal and external sources of health control. Results showed that two problem-oriented coping strategies, i.e. positive reappraisal and responsibility, were seen more in people with IBD. Also, no difference was seen in other coping strategies between patients and healthy groups. This finding is not consistent with previous research results, which showed people with heart disease used an emotional coping style more than healthy people in dealing with problems [21]. Other research has demonstrated the use of emotion-oriented coping strategies in women with depression is significantly higher than in scores of non-depressed women [22]. Another study has shown that patients with irritable bowel syndrome use problem-oriented coping styles less than healthy people [23]. Arefi et al. emphasized the positive relationship between disease and emotion-oriented coping strategies [21]. Although Arafi et al. emphasized the positive relationship between disease and emotion-oriented coping strategies, in the present study, there was a difference in the use of emotion-oriented coping strategies, such as escape-avoidance strategies were not seen [21]. In explaining this finding, the medical characteristics of this disease and the psychological conditions of the patient should be mentioned. For example, due to the unknown cause of inflammatory bowel disease and especially the lack of definitive medical treatments, the patient is constantly involved with the stressful situation caused by the disease, and it is impossible to avoid this situation.
As a result, in such a situation, using the avoidance coping strategy (as one of the emotion-oriented strategies) to reduce the stress caused by the disease lacks many places. The participants in the present study were people suffering from inflammatory bowel disease who visited the hospital and were often treated. As a result, the avoidance coping strategy, which means denying a difficult situation and avoiding facing it, showed little in this population. This finding is consistent with Khaledian et al.’s study, which showed no significant difference between people with irritable bowel syndrome and healthy people using an escape-avoidance strategy [23]. Regarding the use of problem-oriented coping strategies, the results of the present study are also not consistent with previous studies [21-23] because these studies showed a significant difference between people with physical and psychological diseases and normal (healthy) people in using problem-oriented coping strategies, this difference is in favor of healthy people, so these people use more problem-oriented coping strategies compared to their peers. The present study showed that positive reappraisal strategies and responsibilities are higher in people with inflammatory bowel disease. According to the fact, the patients with inflammatory bowel syndrome who took part in the present study had been diagnosed with this disease for at least 2 years, they gradually take responsibility for the problems caused by the disease and by adjusting or correcting their beliefs and positive re-evaluation of one’s problems will help curb the disease and improve one’s coping status. However, no study has shown that people with physical and mental illnesses use problem-oriented coping strategies more than normal people.
Regarding the health control source variable, of 8 coping strategies, the only emotion-oriented coping strategy was avoidance in people with an internal control source. Thus, other coping strategies between these two groups, i.e. results, showed no difference between internal and external control sources. The average coping strategies in two groups of people with internal and external sources of health control were statistically the same. Patients on hemodialysis with an internal locus of control adjust and adapt better than those with an external locus of control. Their compliance with diet, acceptance of limitations, vocational adjustments, coping with seeking information, and adopting an active, problem-solving attitude is better. The internal health locus of control over time may be an important determinant of change for individuals with chronic illnesses [24]. The results of previous research about the relationship between health locus of control and coping strategies are different. Zhang et al. [25] showed higher use of problem-solving coping strategies by people with an internal locus of control. In comparison, Wilski et al. [26] showed higher use of problem-solving coping strategies by people with an external source of control and higher use of emotion-oriented and avoidance coping strategies by people with an internal source of control [26]. The present study is also in line with Cohen-Biton et al. [27] because they showed that people with an internal source of control use the emotion-oriented coping strategy of avoidance more than their peers. In the present study, people with an internal source of control preferred to control the stressful factor by distancing themselves from the stressful situation and conditions [27]. Also, the present study’s results are inconsistent with previous studies because they showed no difference between coping skills in two groups of people with internal and external sources of health control [28].
Research and data collection methods play a major role in explaining the disparity between the current study and previous studies’ findings. The self-assessment tools (questionnaires) used to measure people’s sources of control and people’s interest heavily influences coping strategies in self-presentation and impression management strategies. Thus, it is reasonable to speculate that people answered previous research questions unrealistically. In contrast to previous research, the collected data for this study were collected online and by virtual surveys. Because they are confident about the anonymity of their identity, respondents answer questions more honestly in such a situation.
5. Conclusion
According to research, coping strategies are statistically similar in 4 groups of inflammatory bowel disease patients and healthy people. Considering the lack of significant differences between the groups regarding the dominant components of coping strategies and locus of control, this finding is statistically logical and natural. The present study showed that two problem-oriented strategies, i.e. positive reappraisal and responsibility, are higher in people with inflammatory bowel disease than in healthy people. The present finding challenges the results of previous research for the first time. It creates a disparity in the research literature on this topic, which shows the necessity of conducting more research in this field.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered in this article. The current study observed subject-related ethical considerations (Ethical Code: IR.IAU.CTB.REC.1399.21).
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest
Acknowledgments
We appreciate the participants who were involved in this study.
References
Inflammatory bowel disease (IBD) is a group of chronic diseases of the digestive tract with severe symptoms such as urgent diarrhea, abdominal pain, and cramping. Crohn disease (CD) and ulcerative colitis (UC) are the most frequent types of IBD [1]. The pathogenesis of these complex multifactorial diseases has not been fully understood [2]. IBD has a relapsing and remitting phase and manifests with GI symptoms such as diarrhea, nausea, blood in the stool, abdominal pain, sometimes accompanied by joint or skin problems, and fatigue [3]. Complications include intestinal perforations, strictures, and fistulas. Also, anxiety disorders, depression, and bipolar disorder can affect the course of IBD [4].
Many studies have reported the disease’s profound impact on patients’ psychological well-being [5]. The health locus of control also seems to be a psychological construct influencing health and disease. It is an important construct that is less addressed compared to other factors. The health locus of control is a construct based on the control locus concept and social learning theory used in the health area. The health locus of control points out the individuals’ beliefs about factors impacting health [6]. In adults, internal locus of control (LOC) has been associated with positive health outcomes, such as reduced disease burden, increased self-rated health, adherence to treatment, and general health. Conversely, an external LOC indicates that a person believes outside factors such as doctors, other people, or chance determine health outcomes [7].
In the adult population, external LOC has been associated with negative outcomes, such as decreased quality of life, increased emergency department visits, and reduced acceptance of illness [8]. Helvik et al. investigated the relationship between two dimensions of coping (locus of control orientation and coping strategies/ways of coping) and health-related quality of life outcomes in two very different groups of older adults: One hospitalized with depression, the other living in the community without depression. There was no association between emotional- and problem-focused coping strategies and health-related quality-of-life outcomes in the depressed or non-depressed group [8, 9].
Hashemi Razini et al. [10] found a significant relationship between coping skills and locus of control with death anxiety. Emotional and avoidance coping strategies and external locus of control can predict the level of death anxiety [10]. Bjørkløf et al. found that depressed elderly people compared to non-depressed elderly, used more external locus of control [11]. Moreover, they used less problem-oriented coping strategies. Lazarus and Folkman [12] defined stress as a dynamic and mutual relationship between the person and the environment. According to this definition, coping strategies include intellectual, emotional, and behavioral efforts of a person used when facing psychological pressures to overcome, tolerate or minimize the effects of stress [12].
In a study by Polizzi et al. [13], maternal locus control was significantly associated with children’s coping strategies. Furthermore, their findings show positive and negative correlations between specific scales of maternal locus of control and children’s coping styles. Health psychology specialists, doctors, nurses in psychosomatic diseases, and researchers in this field will benefit from this study. IBD patients have several factors that play a role in their lives, especially since the source of health control is a two-dimensional concept [13]. According to previous studies about psychosomatic disorders and IBD, the place of control for coping strategies with stress is because psychosomatic disorders are absent in health psychology research literature. It reports that IBD could have such severe symptoms that the patient is often unaware of its stress roots and cannot cope with them. Therefore, the patient does not seek psychological or even cognitive treatments. Considering these factors and few studies in this field, the researchers assumed that cognitive factors such as problem-oriented and emotion-oriented coping strategies could be predicted and investigated based on internal and external control sources. The question is how a patient copes with and responds to the stress of being diagnosed with and the ongoing effects of IBD. This study aimed to compare the coping strategies of IBD patients and healthy people regarding health locus of control.
2. Methods
The study method was causal-comparative. The study population included all patients with inflammatory bowel disease referred to the Bowel Department of Jam Hospital in Tehran, Iran, from April to September 2020. The research sample included 200 subjects (87 healthy people and 113 people with inflammatory bowel disease) selected by the convenience and purposeful sampling method. Using the G*power tool with α=0.05 and power=80%, a sample size of 186 was determined to study 93 subjects in each group. Yet, considering the probability of loss, the sample size was increased to 200. The inclusion criteria included moderate IBD according to the Rome III criteria based on the diagnosis of a gastroenterologist (score range: 175-300), literacy for reading and writing to fill out questionnaires, age range within 15 to 60 years, access all participants on Instagram, informed consent to participate in the study, organic gastrointestinal disorders approved by a gastroenterologist, and no acute physical illness and psychological disorder under psychiatric treatment. The exclusion criteria were an incomplete questionnaire and the unwillingness to continue the study.
The researcher went to the educational center of the hospital. After obtaining the introduction sheet, he was referred to the treatment department for gastrointestinal diseases, colitis, and Crohn disease and the association of gastrointestinal patients. After obtaining permission from that authority, the researcher went to the center’s departments and coordinated with the department officials. Then, the researcher presented the questionnaires to the patients online through Instagram, and they agreed to answer them. The ethical considerations were getting informed consent from the participants, getting them to fill out the questionnaires, and keeping the information confidential. After coordinating with the authorities, establishing initial communication, and creating a sense of trust regarding the confidentiality of information among the patients and no need to mention names, the questionnaires were distributed. During the questionnaire implementation, more explanations were given if any question was incomprehensible or the patients had difficulty understanding them. Also, the test participation was voluntary and based on the participants’ wishes. After collecting the questionnaires, the raw scores were calculated using the scoring key. SPSS software, version 24 was used to run a two-way multivariate analysis of variance in the data. To test the normality of the data distribution resulting from the measurement of the research variables, we used the Kolmogorov-Smirnov, Levene’s, and Box tests with a significance level greater than 0.05. Additionally, a 2-variable Chi-square test was used to test the homogeneity of the 4 research subgroups in terms of the 3 demographic variables of gender, class, and level of education.
Research tools
The irritable bowel syndrome symptom index
This scale was developed by Francis, Morris, and Horoll and consists of 5 sections that examine the symptoms of IBS, including pain, defecation disorders, bloating, disease effects on daily activities, and extra-intestinal symptoms on an intensity scale [14]. The average score of each section is 100, and the total score of the questionnaire is 500. Mild, moderate, and severe cases are represented with score ranges of 75-175, 175-300, and higher than 300, respectively. The internal correlation coefficient and Cronbach α of the scale are 0.70 in the Iranian version [15].
Multidimensional health locus control
Multidimensional health locus control (MHLC) was first developed by Wallston, Stein, and Smith (1994) to determine the health locus of control [16]. The MHLC is composed of a total of 18 items, including the internal locus of control (items 13, 12, 7, 6, 1, and 17), the chance locus of control (items 15, 11, 9, 4, 2, and 16), and the powerful others locus of control (items 14, 10, 7, 5, 3, and 18). Participants should respond to items on a 6-point Likert scale from 1 to 6 (completely disagree, disagree, slightly disagree, slightly agree, agree, and completely agree). The reliability of this scale was reported by Cronbach α coefficient for internal control components as 0.68, chance control as 0.74, and other control as 0.51 [17]. In Iran, the concurrent validities of the questionnaire were 0.57, 0.49, and 0.53, respectively. The reliability of this scale using the Cronbach α coefficient was acceptable for internal (0.68), powerful others (0.72), and chance (0.66). The test-retest test reliability indices, after a time interval of 4 weeks, were 0.60 for internal, 0.58 for chance, and 0.74 for powerful others [18]. A Cronbach α coefficient of 0.751 was calculated for the MHLC, indicating the validity of the research tool.
Folkman and Lazarus coping strategies inventory
The questionnaire was developed to assess the specific ways in which people cope with stressors. This definition has four key elements. Coping is a process-oriented approach, not static [19]. The first version of “ways of Coping” [18] contained 68 items that were derived from the theoretical framework outlined by Lazarus and his colleagues [12]. The revised 66-item version differs from the original in that redundant and unclear was removed [19]. Further, the response format was changed from “yes-no” to a 4-point Likert scale so that respondents could indicate the frequency with which they use each strategy (0=does not apply and or not used, 1=used somewhat, 2=used quite a bit, 3=used a great deal). All questions are scored with the Likert scale of not at all=0, sometimes=1, quite a bit=2, and very much=3. The questionnaire has 8 subscales: Confrontation, withdrawal, self-control, social support, responsibility acceptance, escape avoidance, problem-solving, and positive reappraisal. Higher scores demonstrate more applications of the coping strategies. Folkman and Lazarus [19] reported Cronbach α coefficient for the social support, escape-avoidance, and problem-solving subscales as 0.76, 0.72, and 0.68, respectively [19]. In Iran, Padyab et al. [20] reported a reliability of 0.88 on the scale [20]. This research tool showed acceptable validity based on Cronbach α coefficient of 0.888.
3. Results
The sociodemographic characteristics of the research included the patients (n=113) and healthy control group (n=87) with internal health control source (n=165) and external health control source (n=35). The results showed 67 females (59.3%) and 46 males (40.7%) were patients. Furthermore, 63 participants (72.4%) were healthy females, and 24(27.6%) were healthy males. The highest patient frequency was found in the 35-35 years age group with n=74 (65.5%), while the lowest was found in patients over 36 years old and above. Thus, patients with bachelor’s degrees and below were more frequent at 79.7%, whereas healthy people were lower frequent at 28(32.2%) with master’s degrees and above (Table 1).

As presented in Table 2, the groups’ significant levels of observed F statistics indicate that between people with health control sources (internal/external), regarding the variables of responsibility, positive reappraisal, and direct copying.

There is a significant difference between social support seeking, escaping-avoiding, social support seeking, continence, and avoiding. Also, the observed F statistics of the control source is significant. This finding indicates a significant difference between people with irritable bowel syndrome and normal people regarding responsibility, positive reappraisal, direct coping, social support seeking, escaping-avoiding, social support seeking, continence, and avoiding. Moreover, the interaction between the group and the source has been significant. Therefore, there is a significant difference between the 4 groups regarding responsibility variables, positive reappraisal, direct confrontation, planning to solve the escape-avoidance problem, seeking social support, refraining, and avoidance (P<0.001). Considering the significance of the difference between the groups and the source of health control, a two-way analysis of variance was performed, the results of which are shown in Table 3.

As seen in Table 3, there is a significant difference between irritable bowel syndrome and normal people (P<0.001). Therefore, according to the results, people with irritable bowel syndrome are significantly higher than normal people in terms of positive reappraisal and responsibility. However, there is no significant difference in other coping strategies between irritable bowel syndrome and normal individuals (P>0.05).
Table 3 shows a significant difference between individuals with the source of internal and external control only regarding volatile variables (P<0.001). However, there is no significant difference between individuals with the source of internal and external control over other coping strategies (P>0.05). Therefore, according to Table 3, people with an internal control source are significantly higher than those with external control sources.
Also, as seen in Table 3, among individuals with irritable and ordinary intestinal syndromes with internal and external control sources, in terms of responsibility variables (P<0.001), positive reappraisal (P=0.004). Avoiding there is a meaningful difference (P<0.001). However, there is no significant difference between people with the irritable and ordinary intestinal syndrome with the source of internal and external control in terms of direct coping variables, searching for social support, and avoiding differences (P>0.05). In other words, the average coping skills in four groups of patients healthy with intestinal inflammation, with an internal and external locus of health control, are statistically the same.
4. Discussion
The study aimed to compare coping strategies in people with inflammatory bowel syndrome and healthy people according to internal and external sources of health control. Results showed that two problem-oriented coping strategies, i.e. positive reappraisal and responsibility, were seen more in people with IBD. Also, no difference was seen in other coping strategies between patients and healthy groups. This finding is not consistent with previous research results, which showed people with heart disease used an emotional coping style more than healthy people in dealing with problems [21]. Other research has demonstrated the use of emotion-oriented coping strategies in women with depression is significantly higher than in scores of non-depressed women [22]. Another study has shown that patients with irritable bowel syndrome use problem-oriented coping styles less than healthy people [23]. Arefi et al. emphasized the positive relationship between disease and emotion-oriented coping strategies [21]. Although Arafi et al. emphasized the positive relationship between disease and emotion-oriented coping strategies, in the present study, there was a difference in the use of emotion-oriented coping strategies, such as escape-avoidance strategies were not seen [21]. In explaining this finding, the medical characteristics of this disease and the psychological conditions of the patient should be mentioned. For example, due to the unknown cause of inflammatory bowel disease and especially the lack of definitive medical treatments, the patient is constantly involved with the stressful situation caused by the disease, and it is impossible to avoid this situation.
As a result, in such a situation, using the avoidance coping strategy (as one of the emotion-oriented strategies) to reduce the stress caused by the disease lacks many places. The participants in the present study were people suffering from inflammatory bowel disease who visited the hospital and were often treated. As a result, the avoidance coping strategy, which means denying a difficult situation and avoiding facing it, showed little in this population. This finding is consistent with Khaledian et al.’s study, which showed no significant difference between people with irritable bowel syndrome and healthy people using an escape-avoidance strategy [23]. Regarding the use of problem-oriented coping strategies, the results of the present study are also not consistent with previous studies [21-23] because these studies showed a significant difference between people with physical and psychological diseases and normal (healthy) people in using problem-oriented coping strategies, this difference is in favor of healthy people, so these people use more problem-oriented coping strategies compared to their peers. The present study showed that positive reappraisal strategies and responsibilities are higher in people with inflammatory bowel disease. According to the fact, the patients with inflammatory bowel syndrome who took part in the present study had been diagnosed with this disease for at least 2 years, they gradually take responsibility for the problems caused by the disease and by adjusting or correcting their beliefs and positive re-evaluation of one’s problems will help curb the disease and improve one’s coping status. However, no study has shown that people with physical and mental illnesses use problem-oriented coping strategies more than normal people.
Regarding the health control source variable, of 8 coping strategies, the only emotion-oriented coping strategy was avoidance in people with an internal control source. Thus, other coping strategies between these two groups, i.e. results, showed no difference between internal and external control sources. The average coping strategies in two groups of people with internal and external sources of health control were statistically the same. Patients on hemodialysis with an internal locus of control adjust and adapt better than those with an external locus of control. Their compliance with diet, acceptance of limitations, vocational adjustments, coping with seeking information, and adopting an active, problem-solving attitude is better. The internal health locus of control over time may be an important determinant of change for individuals with chronic illnesses [24]. The results of previous research about the relationship between health locus of control and coping strategies are different. Zhang et al. [25] showed higher use of problem-solving coping strategies by people with an internal locus of control. In comparison, Wilski et al. [26] showed higher use of problem-solving coping strategies by people with an external source of control and higher use of emotion-oriented and avoidance coping strategies by people with an internal source of control [26]. The present study is also in line with Cohen-Biton et al. [27] because they showed that people with an internal source of control use the emotion-oriented coping strategy of avoidance more than their peers. In the present study, people with an internal source of control preferred to control the stressful factor by distancing themselves from the stressful situation and conditions [27]. Also, the present study’s results are inconsistent with previous studies because they showed no difference between coping skills in two groups of people with internal and external sources of health control [28].
Research and data collection methods play a major role in explaining the disparity between the current study and previous studies’ findings. The self-assessment tools (questionnaires) used to measure people’s sources of control and people’s interest heavily influences coping strategies in self-presentation and impression management strategies. Thus, it is reasonable to speculate that people answered previous research questions unrealistically. In contrast to previous research, the collected data for this study were collected online and by virtual surveys. Because they are confident about the anonymity of their identity, respondents answer questions more honestly in such a situation.
5. Conclusion
According to research, coping strategies are statistically similar in 4 groups of inflammatory bowel disease patients and healthy people. Considering the lack of significant differences between the groups regarding the dominant components of coping strategies and locus of control, this finding is statistically logical and natural. The present study showed that two problem-oriented strategies, i.e. positive reappraisal and responsibility, are higher in people with inflammatory bowel disease than in healthy people. The present finding challenges the results of previous research for the first time. It creates a disparity in the research literature on this topic, which shows the necessity of conducting more research in this field.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered in this article. The current study observed subject-related ethical considerations (Ethical Code: IR.IAU.CTB.REC.1399.21).
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest
Acknowledgments
We appreciate the participants who were involved in this study.
References
- Salari-Moghaddam A, Keshteli AH, Esmaillzadeh A, Adibi P. Adherence to the pro-inflammatory diet in relation to prevalence of irritable bowel syndrome. Nutr J. 2019; 18(1):72. [DOI:10.1186/s12937-019-0487-6] [PMID] [PMCID]
- Berding A, Witte C, Gottschald M, Kaltz B, Weiland R, Gerlich C, et al. Beneficial effects of education on emotional distress, self-management, and coping in patients with inflammatory bowel disease: A prospective randomized controlled study. Inflamm Intest Dis. 2017; 1(4):182-90. [DOI:10.1159/000452989] [PMID] [PMCID]
- Seyedian SS, Nokhostin F, Malamir MD. A review of the diagnosis, prevention, and treatment methods of inflammatory bowel disease. J Med Life. 2019; 12(2):113-22. [DOI:10.25122/jml-2018-0075] [PMID] [PMCID]
- Bednarikova H, Kascakova N, Furstova J, Zelinkova Z, Falt P, Hasto J, et al. Life stressors in patients with inflammatory bowel disease: Comparison with a population-based healthy control group in the czech republic. Int J Environ Res Public Health. 2021; 18(6):3237. [DOI:10.3390/ijerph18063237] [PMID] [PMCID]
- McCombie AM, Mulder RT, Gearry RB. How IBD patients cope with IBD: A systematic review. J Crohns Colitis. 2013; 7(2):89-106. [DOI:10.1016/j.crohns.2012.05.021] [PMID]
- Cassidy T, Hilton S. Family health culture, health locus of control and health behaviours in older children. J Pediatr Med Care. 2017; 1(1):4-9. [Link]
- Nazareth M, Richards J, Javalkar K, Haberman C, Zhong Y, Rak E, et al. Relating health locus of control to health care use, adherence, and transition readiness among youths with chronic conditions, North Carolina, 2015. Prev Chronic Dis. 2016; 13:E93. [DOI:10.5888/pcd13.160046] [PMID] [PMCID]
- Helvik AS, Bjørkløf GH, Corazzini K, Selbæk G, Laks J, Østbye T, et al. Are coping strategies and locus of control orientation associated with health-related quality of life in older adults with and without depression? Arch Gerontol Geriatr. 2016; 64:130-7. [DOI:10.1016/j.archger.2016.01.014] [PMID]
- Pourhoseinzadeh M, Gheibizadeh M, Moradikalboland M. The relationship between health locus of control and health behaviors in emergency medicine personnel. Int J Community Based Nurs Midwifery. 2017; 5(4):397-407. [PMID] [PMCID]
- Hashemi Razini H, Baheshmat Juybari S, Ramshini M. [Relationship between coping strategies and locus of control with the anxiety of death in old people (Persian)]. Iran J Ageing. 2017; 12(2):232-41. [DOI:10.21859/sija-1202232]
- Bjørkløf GH, Engedal K, Selbæk G, Maia DB, Coutinho ES, Helvik AS. Locus of control and coping strategies in older persons with and without depression. Aging Ment Health. 2016; 20(8):831-9. [DOI:10.1080/13607863.2015.1040722] [PMID]
- Lazarus RS, Folkman S. Stress, appraisal, and coping. Berlin: Springer; 1984. [Link]
- Polizzi C, Fontana V, Perricone G, D'Angelo P, Jankovic M, Taormina C, et al. Coping strategies and locus of control in childhood leukemia: A multi-center research. Pediatr Rep. 2015; 7(2):5703. [DOI:10.4081/pr.2015.5703] [PMID] [PMCID]
- Francis CY, Morris J, Whorwell PJ. The irritable bowel severity scoring system: A simple method of monitoring irritable bowel syndrome and its progress. Aliment Pharmacol Ther. 1997 ; 11(2):395-402. [DOI:10.1046/j.1365-2036.1997.142318000.x] [PMID]
- Jafari P, Asadollahi Z, Moini M, Seyed Mirzaie M. Health related quality of life in Iranian patients with irritable bowel syndrome: Reliability and validity of the Persian version of the IBS-QOL. Iran Red Crescent Med J. 2013; 15(8):723-8. [DOI:10.5812/ircmj.4605] [PMID] [PMCID]
- Wallston KA, Stein MJ, Smith CA. Form C of the MHLC scales: A condition-specific measure of locus of control. J Pers Assess. 1994; 63(3):534-53. [DOI:10.1207/s15327752jpa6303_10] [PMID]
- Ubbiali A, Donati D, Chiorri C, Bregani V, Cattaneo E, Maffei C, et al. The usefulness of the multidimensional health locus of control form C (MHLC-C) for HIV+ subjects: An Italian study. AIDS Care. 2008; 20(4):495-502.[DOI:10.1080/09540120701867115] [PMID]
- Moshki M, Ghofranipour F, Hajizadeh E, Azadfallah P. Validity and reliability of the multidimensional health locus of control scale for college students. BMC Public Health. 2007; 7:295. [DOI:10.1186/1471-2458-7-295] [PMID] [PMCID]
- Folkman S, Lazarus RS. The relationship between coping and emotion: Implications for theory and research. Soc Sci Med. 1988; 26(3):309-17. [DOI:10.1016/0277-9536(88)90395-4] [PMID]
- Padyab M, Ghazinour M, Richter J. Factor structure of the Farsi version of the ways of coping questionnaire. J Appl Soc Psychol. 2012; 42(8):2006-18. [DOI:10.1111/j.1559-1816.2012.00928.x]
- Arefi M, Rahimi R, Gol Mohammadian M. [Review and compare personality traits and coping styles men and women with and without heart disease outpatient (Persian)]. J Sabzevar Univ Med Sci. 2016; 23(1):122-32. [Link]
- Ezzati A, Nouri R, Hasani J. [Structural relationship model between social support, coping strategies, stigma and depression in infertile women in Tehran, Iran, 2010 (Persian)]. Iran J Obstet Gynecol Infertil. 2013; 16(45):20-8. [DOI:10.22038/IJOGI.2013.683]
- Khaledian H, Parhizkar B, Shikhesmaeili F, Moradi M. [Comparison of the personality characteristics and coping strategies between the patients with irritable bowel syndrome and normal individuals (Persian)]. Sci J Kurdistan Univ Med Sci. 2019; 24(3):85-95. [DOI:10.29252/sjku.24.3.85]
- Kohli S, Batra P, Aggarwal HK. Anxiety, locus of control, and coping strategies among end-stage renal disease patients undergoing maintenance hemodialysis. Indian J Nephrol. 2011; 21(3):177-81. [DOI:10.4103/0971-4065.83729] [PMID] [PMCID]
- Zhang W, Liu H, Jiang X, Wu D, Tian Y. A longitudinal study of posttraumatic stress disorder symptoms and its relationship with coping skill and locus of control in adolescents after an earthquake in China. Plos One. 2014; 9(2):e88263.[DOI:10.1371/journal.pone.0088263] [PMID] [PMCID]
- Wilski M, Brola W, Tomczak M. Health locus of control and mental health in patients with multiple sclerosis: Mediating effect of coping strategies. Res Nurs Health. 2019; 42(4):296-305. [DOI:10.1002/nur.21955] [PMID]
- Cohen-Biton L, Buskila D, Nissanholtz-Gannot R. The effect of the fibrotherapy intervention program on the coping patterns of fibromyalgia patients. J Clin Rheumatol. 2022; 28(5):278-83. [DOI:10.1097/RHU.0000000000001866] [PMID] [PMCID]
- Shpakou A, Naumau IA, Krestyaninova TY, Znatnova AV, Lollini SV, Surkov S, et al. Physical activity, life satisfaction, stress perception and coping strategies of university students in Belarus during the COVID-19 pandemic. Int J Environ Res Public Health. 2022; 19(14):8629. [DOI:10.3390/ijerph19148629] [PMID] [PMCID]
Type of Study: Orginal Article |
Subject:
● Health Education
Received: 2022/09/10 | Accepted: 2023/01/25 | Published: 2023/05/28
Received: 2022/09/10 | Accepted: 2023/01/25 | Published: 2023/05/28
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |