Volume 13, Issue 3 (May & Jun 2023)
J Research Health 2023, 13(3): 163-174 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Kul Uçtu A, Kaplan V. Health Literacy in Turkish Pregnant Women in the Framework of Prenatal Attachment and Coping Styles With Stress. J Research Health 2023; 13 (3) :163-174
URL: http://jrh.gmu.ac.ir/article-1-2183-en.html
URL: http://jrh.gmu.ac.ir/article-1-2183-en.html
1- Department of Midwifery, Gulhane Faculty of Health Sciences, University of Health Sciences, Ankara, Turkey. , kularzu@gmail.com
2- Department of Nursing, Faculty of Health Science, Harran University, Şanlıurfa, Turkey.
2- Department of Nursing, Faculty of Health Science, Harran University, Şanlıurfa, Turkey.
Full-Text [PDF 861 kb]
(502 Downloads)
| Abstract (HTML) (1919 Views)
Full-Text: (555 Views)
1. Introduction
The concept of attachment was first defined by Bowlby (1969) as “a lasting psychological connectedness between human beings”. According to Bowlby, attachment begins in the prenatal period between mother and baby. It has an enormous and unique effect and will last a lifetime with the continuity of positive conditions [1, 2]. Thanks to this attachment, the mother adapts to pregnancy more easily and feels stronger in meeting the physiological and psychological needs of the baby [3, 4]. Prenatal attachment is an important and specific process for forming a secure bond between mother and baby [4].
Attachment in the prenatal period is affected by many variables, and among the most important determinants is the psychological wellbeing of the pregnant mother [5, 6]. Factors such as undertaking new roles and responsibilities during pregnancy, possible negative changes in body image, disruption of daily routines, and changes in social interactions can cause stress [7, 8]. It is thought that the positive effects of attachment in the face of these negative situations may protect and improve the psychological status and coping styles of mothers-to-be [9]. According to studies, women with a high level of prenatal attachment do not see pregnancy as stress and think the problems they experience are more manageable [10, 11]. In this context, it is noteworthy that prenatal attachment is of great importance in terms of the way pregnant women cope with stress. Self-confident, optimistic, and social support-seeking approaches are accepted as positive, while submissive and helpless approaches are negative coping methods [12]. It has been reported that the use of positive stress-coping methods by pregnant women has a positive effect on maintaining wellbeing [5, 13] and attachment [12, 14].
Maintaining the physical, psychological, and psychosocial wellbeing of maternal and infant health during pregnancy is associated with increasing the level of health literacy [15]. Health literacy is a concept that brings people together in the fields of health and literacy [16]. Health literacy addresses the capacity of individuals to obtain, process, and understand the basic health information and services they need to make the right health-related decisions [17].
Low health literacy is a global problem today [17, 18]. Low health literacy often means that people cannot effectively manage their health, access health services effectively, understand available information, and thus make sound decisions [16]. Pregnant women with low health literacy are more likely to understand prenatal screening tests inadequately [19]. A woman’s low health literacy affects her health knowledge, protective behavior, and ability to care for her child [20]. In a systematic review dealing with the effects of health literacy on female reproductive health, it is stated that health literacy level directly affects postpartum breastfeeding and infant health, starting from the pre-pregnancy period [21]. In this context, health literacy can influence attachment, an important infant and maternal health variable. Based on the literature, many studies mention the positive contribution of health literacy during pregnancy [19, 22, 23, 24]. However, there is no study on its effects on prenatal attachment. As a problem that needs to be examined, studies on the subject draw attention as a major deficiency in the literature. In this study, we aimed to examine the effect of prenatal attachment using structural equation modeling. The attachment is a dynamic process that can affect women during pregnancy and postpartum period in many aspects, such as health literacy and coping styles.
2. Methods
Study design
This was a descriptive, analytical, and cross-sectional study. Using structural equation modeling, we aimed to examine the effect of prenatal attachment during pregnancy and the postpartum period on health literacy and coping styles. We hope this study will greatly contribute to the literature on creating services that provide social awareness.
Study setting
The research was conducted face-to-face with future mothers in a university hospital of a province in the Southeastern Anatolia region of Turkey between May 15 and July 2022. To obtain significant data with the study measurement tools, the minimum number of samples was calculated with the G*power 3.1.3. According to the calculations, the study’s sample size was determined as 325, based on a one-way analysis of variance, at a significance level of 0.05, a power of 80%, and with a medium effect (0.18). Finally, the study was conducted on 420 women to more clearly detect the relationships between the variables.
Study sample
Between the study dates, 420 pregnant women who volunteered to participate in the research and met the inclusion criteria were included in the sample.
The inclusion criteria were as follows:
1) The women were over the age of 18 years,
2) Had a healthy pregnancy,
3) Was in the last trimester of pregnancy,
4) Had a healthy fetus,
5) Without any psychiatric diagnosis.
The exclusion criteria were as follows:
1) Being under the age of 18 years,
2) Had an unhealthy pregnancy,
3) Was in the first or second trimester of pregnancy,
4) Had an unhealthy fetus,
5) Having any psychiatric diagnosis.
Study measures
The study data were collected using a personal information form, prenatal attachment inventory (PAI), stress coping styles scale (SCSS), and health literacy survey (HLS).
Personal information form
The personal information form was developed by the researchers, consisting of 19 questions about the personal (age, education level, employment status, income level, etc.) and obstetric/general health (week of gestation, number of children, pregnancy-related health problem, history of previous miscarriage/stillbirth, type of birth, regular pregnancy control, etc.) information of future mothers.
Prenatal attachment inventory (PAI)
Prenatal Attachment Inventory (PAI) is a 21-item scale developed by Mary Muller in 1990 to assess the thoughts, feelings, and situations experienced by women during pregnancy and to investigate the level of attachment to the baby in the prenatal period [25]. It was adapted into Turkish by Yılmaz and Beji in 2013 [26]. Each item is scored a 4-point Likert type, from 1 to 4. A minimum of 21 and a maximum of 84 points can be obtained from the scale. The higher score obtained by the pregnant women indicates higher attachment levels. In this study, the Cronbach α coefficient of the PAI was found to be 0.903.
Stress coping styles scale (SCSS)
The Stress Coping Styles Scale (SCSS) was adapted into Turkish by Şahin and Durak. The scale consists of 30 items whose responses are rated on a 4-point Likert scale (0 to 3). The scale consists of 5 subscales: Self-confident approach, optimistic approach, helpless approach, submissive approach, and seeking social support. The points obtained from each subscale are divided by the number of items to get the subscale scores. A high score from the subscales indicates that the individual uses the approach mentioned above more [27]. The Cronbach α value was 0.669 in the present study.
Health literacy survey (HLS)
Nurses and other health professionals can use Health Literacy Survey (HLS) to evaluate the level of health literacy in diagnosing healthy or ill individuals to receive health services in all health institutions. It was developed by Toçi et al. in 2003 [28]. Aras and Bayık Temel determined that the Turkish version is valid and reliable. The survey is an easily applicable and understandable scale that can be used to determine the health literacy level of individuals [29]. The scale consists of 25 items and 4 subscales: Accessing information, understanding information, appraisal/evaluation, and application/use. The minimum scale score is 25, and the maximum score is 125. The scale items are scored on a 5-point Likert type: 5=I have no difficulty, 4=I have little difficulty, 3= I have some difficulty, 2=I have a lot of difficulties, 1=I am unable to do / I have no ability / impossible. All items of the scale are positively scored. The application time of the tool is on average 5-10 minutes. Low scores indicate insufficient, problematic and poor health literacy, while high scores indicate adequate and very good. The higher the score means the higher the individual’s health literacy level. In this study, the Cronbach α value was found to be 0.680.
Data collection
The study data were collected at the hospital. The research was conducted through face-to-face interviews with women who voluntarily accepted to participate in the study and met the inclusion criteria. Questionnaire forms were distributed to the women, explaining the purpose of the research and the importance of giving accurate answers to the questions. They were collected after an average of 15 minutes.
Evaluation of data
In the study, reliability and multicollinearity analyses were performed with the SPSS software, version 25. Then, path analysis with observed variables was performed, and structural equation modeling (SEM) was performed to see whether SCSS and HLS affected PAI with the AMOS 23 package program. Analyzes were performed at a significance level of 0.05.
Multiple normal distribution, confidence analysis, and multiple linear connection results
First, multiple normal distribution control was performed on the data to perform multivariate analysis. For the variables to show multiple normal distributions, the value obtained from the “a*(a+2)” formula must be greater than Mardia’s coefficient (Multivariate value in the AMOS program), where a is the number of observed variables. When the skewness and kurtosis values of the data were examined, it was seen that the variables met the ±2 limit. Thus, the data were normally distributed.
Path analysis with observed variables
The fact that SEM analysis offers the opportunity to test more than one relationship simultaneously is an important difference from traditional regression analysis. In SEM-based analyses where direct, indirect, or regulatory causality relationships between variables are tested, research is not always done on latent variables. The causality relationship between the variables can also be calculated by modeling the observed variables. Path analysis was performed by including the averages of the total scores obtained in testing the relationship between PAI, consisting of 21 items, SCSS, comprising 30 items, and HLS, comprising 25 items.
3. Results
The Mean±SD age of the pregnant women was 30.93±5.59 years; 34.8% were university graduates; 47.4% of their spouses were university graduates. About 57.4% of women were unemployed; 92.9% had a nuclear family, and 67.9% had a middle-income level (Table 1).


The Mean±SD number of pregnancies of the pregnant women was 2.38±1.45. The Mean±SD number of births was 1.15±1.20. About 66.7% had planned pregnancies, 75.7% planned their pregnancy, and 40.5% did not plan the mode of delivery. Finally, 76.4% had not participated in pregnancy education programs (Table 1).
When the fit indices were examined in the structural equation modeling, the following values were obtained: CMIN=13,702, df=4, CMIN/df=3.425, RMSEA=0.076, CFI=0.976 and GFI=0.987 (Table 2).

All fit indices were obtained within the desired limits, and each path shown in Figure 1 model was statistically significant (P<0.01). The data obtained from the analysis of the predictive relationships between the prenatal attachment of pregnant women, their coping styles with stress, and their health literacy levels are presented in Table 3.

As seen, prenatal attachment of pregnant women and their way of coping with stress are important factors. The coefficient for this factor was B0=0.352, and a strong positive correlation was found between prenatal attachment and stress coping levels (P<0.001). According to the analyses, a 1-unit increase in prenatal attachment level causes an increase of 0.352 in the stress coping styles mean score. Correlation analysis examined the relationship between this result and the subscales (Table 4).
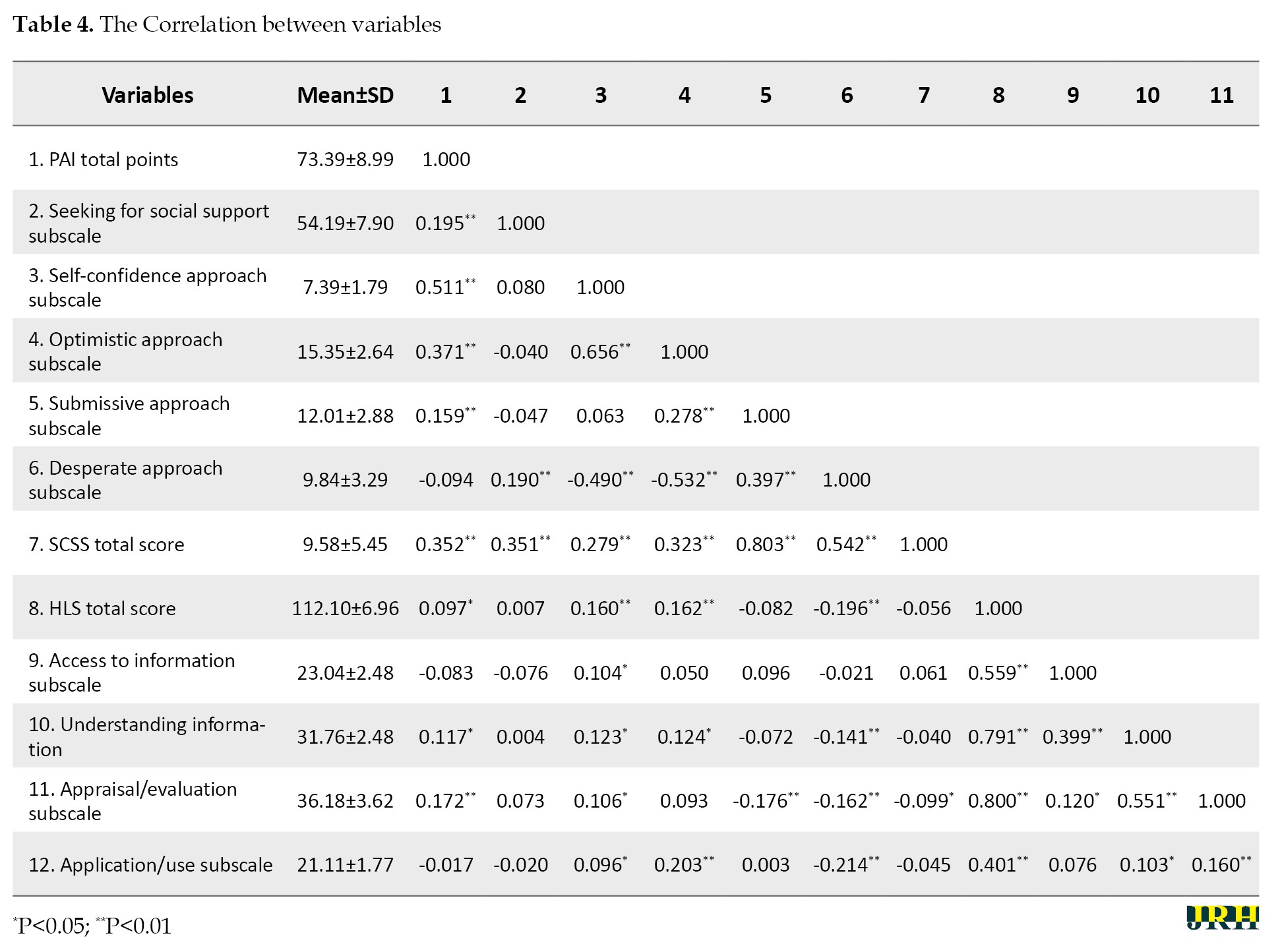
According to the analysis results, there was a positive correlation between the prenatal attachment levels of the pregnant women and the seeking of social support and submissive approach styles and weak, optimistic, and moderate approaches, and a strong positive relationship with self-confident approach styles (P<0.001).
In the model, health literacy is an important variable in the prenatal attachment of pregnant women. The correlation coefficient for this variable was B0=0.108 (Table 3). A strong positive correlation was found between the prenatal attachment of pregnant women and health literacy (P=0.016). According to the analysis, a 1-unit increase in health literacy causes an increase of 0.108 units in prenatal attachment. Correlation analysis was performed to examine the relationship of this effect between subscales (Table 4). According to the investigations, we found a weak positive correlation between the prenatal attachment levels of the pregnant women and the subscales of understanding the information and appraisal/evaluation of the health literacy scale (P<0.001).
In addition, the prenatal attachment of pregnant women and the number of pregnancies and births significantly affected the model. The correlation coefficient for the number of pregnancies was B0=0.135, and the correlation coefficient for the number of births was B0=-0.231 (Table 3). A strong positive correlation was found between the prenatal attachment levels of pregnant women and the number of pregnancies (P<0.001). According to the analysis, a 1-unit increase in the number of pregnancies causes an increase of 0.135 in prenatal attachment levels. According to the analysis, a 1-unit decrease in the number of births causes an increase of 0.231 in prenatal attachment levels (Table 3).
4. Discussion
Our research was carried out to examine the effects of prenatal attachment levels of pregnant women on their stress-coping style and health literacy using a structural equation modeling.
Our study found that the prenatal attachment of pregnant women and the number of pregnancies and births had significant relationships. A strong positive correlation was found between prenatal attachment levels and the number of pregnancies (P<0.001). Research results show that prenatal attachment increases as the number of pregnancies increase [30, 31]. However, some studies show that the increase in the number of pregnancies does not alone explain the anxiety level and that the prenatal attachment levels of women with two or more living children are lower [4, 32]. So, prenatal attachment cannot be explained by a single variable. Variables such as age, education, employment, family type, income level, spouse relationship, desire and planning of pregnancy, number of pregnancies, number of births, past experiences, psychosocial health, social support, receiving preconception care, antenatal controls, preparation for childbirth are effective on the prenatal attachment [33, 34, 35, 36]. Therefore, it is necessary to examine all the variables as much as possible for each pregnant woman.
Thanks to the structural equation modeling, we found a moderate positive correlation between the PAI of pregnant women and the SCSS self-confident approach subscale and a moderate positive correlation between the optimistic approach subscale (P<0.001). At the same time, there was a weak positive correlation with the submissive approach subscale and no relationship with the helpless approach subscale.
Women experience different stress levels during their mental and physical changes throughout pregnancy [37]. Coping with perceived stress affects the health of their babies. It causes some adverse events (such as low birth weight, premature birth, and difficulty bonding with their baby) that can be experienced from pregnancy to postpartum [38]. For this reason, in terms of evaluating the positive or negative consequences of their perceived stress coping styles, it is necessary to investigate them [12]. It is found that pregnant women who explore their self-confident approach, have an optimistic approach to seeking social support, adopt a positive stress coping style, and are more eager to maintain their wellbeing and find solutions to problems [5]. It has been reported that positive or negative coping styles with stress experienced during pregnancy directly affect prenatal attachment [12, 39]. Therefore, psychological preparation is an important factor while preparing for pregnancy. Evaluating pregnant women’s physical health and psychological state and providing support should be among the routines.
According to a study that evaluated the relationship between stress coping style and prenatal attachment during pregnancy, there is a positive relationship between the attachment levels of those who show a self-confident and optimistic approach to coping with stress [12]. Positive coping methods have been reported to contribute positively to prenatal attachment levels [14, 40]. Regarding the second question of the study, the structural equation modeling showed a strong positive correlation between the HLS and PAI scores of pregnant women. Also, a weak positive correlation existed between prenatal attachment levels, health literacy scale, understanding information, and appraisal/evaluation subscales. For this reason, pregnant women need access to the right source of information. In general, it is thought that women experience more stress during pregnancy and cannot cope with the stress they experience properly because they act with customary knowledge.
In this study, 47.4% of the pregnant women were university graduates, and their Mean±SD HLS score was 112.10 ± 6.96. So, there may be a proportional relationship between high education level and HLS, affecting prenatal attachment. Accessing health-related information through the right sources and understanding and interpreting the acquired knowledge effectively maintain wellbeing during pregnancy [18]. The improvement of maternal and infant health, reducing maternal mortality, increase in the quality of health care, and reducing postpartum problems are associated with an increase in the health literacy level of women [21]. Asadi et al. stated that the level of health literacy during pregnancy is an important determinant that increases healthcare quality [41]. Studies have shown that the increase in health literacy level during pregnancy positively affects participation in health in the preconception period, pregnancy, and postpartum [21, 41, 42]. It has been reported that the mother’s health literacy during pregnancy is affected by factors such as the mother’s psychosocial health status, income status, and education level [43].
Regarding the third question of the study, the structural equation modeling revealed the relationships between stress coping style, health literacy level, number of pregnancies and births, and prenatal attachment. SEM showed strong associations between prenatal attachment, coping styles with stress, and the number of births. As a result of the analysis, coping with stress, health literacy, and the number of pregnancies and births explained 15.7% of prenatal attachment.
Health literacy also effectively contributes to postpartum parenting roles and feeling self-sufficient [43]. In other words, increased health literacy during pregnancy positively affects coping with stress and is associated with prenatal attachment [18]. However, no studies examine the relationship between prenatal attachment, coping with stress, and health literacy. Some studies examined prenatal attachment and stress coping styles or the effects of stress in pregnant women [12, 30, 32, 34]. However, no study examined the relationship between prenatal attachment and health literacy. In a research that was carried out to investigate the relationship between functional health literacy of spouses and prenatal attachment, it is stated that the increase in the health literacy rate of the spouses of pregnant women is effective on their attachment [44]. The study by Aslantekin Özçoban, Ergün, and Erkal Aksoy found that as the level of health literacy increases during pregnancy, adjustment to pregnancy and self-efficacy increases, and the fear of childbirth decreases [42].
For future studies, examining the relationship between prenatal attachment and health literacy in larger sample groups with different races, origins, and socio-demographic characteristics is recommended for future studies.
5. Conclusion
Prenatal attachment levels are associated with coping styles and health literacy levels of pregnant women. As a result of the structural equation modeling, we found a strong positive relationship between the PAI of pregnant women and the SCSS self-confident approach subscale and a moderate positive relationship between the optimistic approach subscale. A weak positive correlation was found with the submissive approach subscale. No relationship was found between the helpless approach subscale and prenatal attachment. A strong positive correlation was found between health literacy and prenatal attachment. Also, there is a strong relationship between prenatal attachment, coping styles with stress, and the number of births. It was concluded that health literacy and stress coping styles were effective variables in prenatal attachment.
Strengths and limitations
There are limitations to this study. First, the study was conducted in a single center. Although the absence of an exemplary research sample is the study’s strength, there was a limitation in making comparisons in the discussion section. At the same time, this is a strong side of the study’s originality. Other limitations are that the pregnant women answered the questions themselves, and the majority of those did not want to participate in the study because they were in the last trimester.
In this context, psychosocial support services should be provided to women to control stress, an important variable that will adversely affect pregnancy as soon as pregnancy is planned. In the content of these services, developing health literacy knowledge and skills is necessary. Secure attachment is also an important point to work on. For this reason, content that will evaluate the psychological status of women during routine pregnancy controls should be prepared, and both the psychological and social needs of women should be determined.
Ethical Considerations
Compliance with ethical guidelines
Before conducting this study, ethical approval was obtained (No. of meetings: 2022/18, Date: 16.02.2022). The purpose of the present study, its duration, and the participant’s rights were explained to the pregnant women before the study.
Funding
This research received no grants from any funding agency in the public, commercial, or not-for-profit sectors.
Authors' contributions
All authors equally contributed to preparing this article: Design, execution, and analysis of the results and approved the final version.
Conflict of interest
The authors declared no conflicts of interest.
Acknowledgments
We want to thank all women who participated in the research.
References
The concept of attachment was first defined by Bowlby (1969) as “a lasting psychological connectedness between human beings”. According to Bowlby, attachment begins in the prenatal period between mother and baby. It has an enormous and unique effect and will last a lifetime with the continuity of positive conditions [1, 2]. Thanks to this attachment, the mother adapts to pregnancy more easily and feels stronger in meeting the physiological and psychological needs of the baby [3, 4]. Prenatal attachment is an important and specific process for forming a secure bond between mother and baby [4].
Attachment in the prenatal period is affected by many variables, and among the most important determinants is the psychological wellbeing of the pregnant mother [5, 6]. Factors such as undertaking new roles and responsibilities during pregnancy, possible negative changes in body image, disruption of daily routines, and changes in social interactions can cause stress [7, 8]. It is thought that the positive effects of attachment in the face of these negative situations may protect and improve the psychological status and coping styles of mothers-to-be [9]. According to studies, women with a high level of prenatal attachment do not see pregnancy as stress and think the problems they experience are more manageable [10, 11]. In this context, it is noteworthy that prenatal attachment is of great importance in terms of the way pregnant women cope with stress. Self-confident, optimistic, and social support-seeking approaches are accepted as positive, while submissive and helpless approaches are negative coping methods [12]. It has been reported that the use of positive stress-coping methods by pregnant women has a positive effect on maintaining wellbeing [5, 13] and attachment [12, 14].
Maintaining the physical, psychological, and psychosocial wellbeing of maternal and infant health during pregnancy is associated with increasing the level of health literacy [15]. Health literacy is a concept that brings people together in the fields of health and literacy [16]. Health literacy addresses the capacity of individuals to obtain, process, and understand the basic health information and services they need to make the right health-related decisions [17].
Low health literacy is a global problem today [17, 18]. Low health literacy often means that people cannot effectively manage their health, access health services effectively, understand available information, and thus make sound decisions [16]. Pregnant women with low health literacy are more likely to understand prenatal screening tests inadequately [19]. A woman’s low health literacy affects her health knowledge, protective behavior, and ability to care for her child [20]. In a systematic review dealing with the effects of health literacy on female reproductive health, it is stated that health literacy level directly affects postpartum breastfeeding and infant health, starting from the pre-pregnancy period [21]. In this context, health literacy can influence attachment, an important infant and maternal health variable. Based on the literature, many studies mention the positive contribution of health literacy during pregnancy [19, 22, 23, 24]. However, there is no study on its effects on prenatal attachment. As a problem that needs to be examined, studies on the subject draw attention as a major deficiency in the literature. In this study, we aimed to examine the effect of prenatal attachment using structural equation modeling. The attachment is a dynamic process that can affect women during pregnancy and postpartum period in many aspects, such as health literacy and coping styles.
2. Methods
Study design
This was a descriptive, analytical, and cross-sectional study. Using structural equation modeling, we aimed to examine the effect of prenatal attachment during pregnancy and the postpartum period on health literacy and coping styles. We hope this study will greatly contribute to the literature on creating services that provide social awareness.
Study setting
The research was conducted face-to-face with future mothers in a university hospital of a province in the Southeastern Anatolia region of Turkey between May 15 and July 2022. To obtain significant data with the study measurement tools, the minimum number of samples was calculated with the G*power 3.1.3. According to the calculations, the study’s sample size was determined as 325, based on a one-way analysis of variance, at a significance level of 0.05, a power of 80%, and with a medium effect (0.18). Finally, the study was conducted on 420 women to more clearly detect the relationships between the variables.
Study sample
Between the study dates, 420 pregnant women who volunteered to participate in the research and met the inclusion criteria were included in the sample.
The inclusion criteria were as follows:
1) The women were over the age of 18 years,
2) Had a healthy pregnancy,
3) Was in the last trimester of pregnancy,
4) Had a healthy fetus,
5) Without any psychiatric diagnosis.
The exclusion criteria were as follows:
1) Being under the age of 18 years,
2) Had an unhealthy pregnancy,
3) Was in the first or second trimester of pregnancy,
4) Had an unhealthy fetus,
5) Having any psychiatric diagnosis.
Study measures
The study data were collected using a personal information form, prenatal attachment inventory (PAI), stress coping styles scale (SCSS), and health literacy survey (HLS).
Personal information form
The personal information form was developed by the researchers, consisting of 19 questions about the personal (age, education level, employment status, income level, etc.) and obstetric/general health (week of gestation, number of children, pregnancy-related health problem, history of previous miscarriage/stillbirth, type of birth, regular pregnancy control, etc.) information of future mothers.
Prenatal attachment inventory (PAI)
Prenatal Attachment Inventory (PAI) is a 21-item scale developed by Mary Muller in 1990 to assess the thoughts, feelings, and situations experienced by women during pregnancy and to investigate the level of attachment to the baby in the prenatal period [25]. It was adapted into Turkish by Yılmaz and Beji in 2013 [26]. Each item is scored a 4-point Likert type, from 1 to 4. A minimum of 21 and a maximum of 84 points can be obtained from the scale. The higher score obtained by the pregnant women indicates higher attachment levels. In this study, the Cronbach α coefficient of the PAI was found to be 0.903.
Stress coping styles scale (SCSS)
The Stress Coping Styles Scale (SCSS) was adapted into Turkish by Şahin and Durak. The scale consists of 30 items whose responses are rated on a 4-point Likert scale (0 to 3). The scale consists of 5 subscales: Self-confident approach, optimistic approach, helpless approach, submissive approach, and seeking social support. The points obtained from each subscale are divided by the number of items to get the subscale scores. A high score from the subscales indicates that the individual uses the approach mentioned above more [27]. The Cronbach α value was 0.669 in the present study.
Health literacy survey (HLS)
Nurses and other health professionals can use Health Literacy Survey (HLS) to evaluate the level of health literacy in diagnosing healthy or ill individuals to receive health services in all health institutions. It was developed by Toçi et al. in 2003 [28]. Aras and Bayık Temel determined that the Turkish version is valid and reliable. The survey is an easily applicable and understandable scale that can be used to determine the health literacy level of individuals [29]. The scale consists of 25 items and 4 subscales: Accessing information, understanding information, appraisal/evaluation, and application/use. The minimum scale score is 25, and the maximum score is 125. The scale items are scored on a 5-point Likert type: 5=I have no difficulty, 4=I have little difficulty, 3= I have some difficulty, 2=I have a lot of difficulties, 1=I am unable to do / I have no ability / impossible. All items of the scale are positively scored. The application time of the tool is on average 5-10 minutes. Low scores indicate insufficient, problematic and poor health literacy, while high scores indicate adequate and very good. The higher the score means the higher the individual’s health literacy level. In this study, the Cronbach α value was found to be 0.680.
Data collection
The study data were collected at the hospital. The research was conducted through face-to-face interviews with women who voluntarily accepted to participate in the study and met the inclusion criteria. Questionnaire forms were distributed to the women, explaining the purpose of the research and the importance of giving accurate answers to the questions. They were collected after an average of 15 minutes.
Evaluation of data
In the study, reliability and multicollinearity analyses were performed with the SPSS software, version 25. Then, path analysis with observed variables was performed, and structural equation modeling (SEM) was performed to see whether SCSS and HLS affected PAI with the AMOS 23 package program. Analyzes were performed at a significance level of 0.05.
Multiple normal distribution, confidence analysis, and multiple linear connection results
First, multiple normal distribution control was performed on the data to perform multivariate analysis. For the variables to show multiple normal distributions, the value obtained from the “a*(a+2)” formula must be greater than Mardia’s coefficient (Multivariate value in the AMOS program), where a is the number of observed variables. When the skewness and kurtosis values of the data were examined, it was seen that the variables met the ±2 limit. Thus, the data were normally distributed.
Path analysis with observed variables
The fact that SEM analysis offers the opportunity to test more than one relationship simultaneously is an important difference from traditional regression analysis. In SEM-based analyses where direct, indirect, or regulatory causality relationships between variables are tested, research is not always done on latent variables. The causality relationship between the variables can also be calculated by modeling the observed variables. Path analysis was performed by including the averages of the total scores obtained in testing the relationship between PAI, consisting of 21 items, SCSS, comprising 30 items, and HLS, comprising 25 items.
3. Results
The Mean±SD age of the pregnant women was 30.93±5.59 years; 34.8% were university graduates; 47.4% of their spouses were university graduates. About 57.4% of women were unemployed; 92.9% had a nuclear family, and 67.9% had a middle-income level (Table 1).


The Mean±SD number of pregnancies of the pregnant women was 2.38±1.45. The Mean±SD number of births was 1.15±1.20. About 66.7% had planned pregnancies, 75.7% planned their pregnancy, and 40.5% did not plan the mode of delivery. Finally, 76.4% had not participated in pregnancy education programs (Table 1).
When the fit indices were examined in the structural equation modeling, the following values were obtained: CMIN=13,702, df=4, CMIN/df=3.425, RMSEA=0.076, CFI=0.976 and GFI=0.987 (Table 2).

All fit indices were obtained within the desired limits, and each path shown in Figure 1 model was statistically significant (P<0.01). The data obtained from the analysis of the predictive relationships between the prenatal attachment of pregnant women, their coping styles with stress, and their health literacy levels are presented in Table 3.

As seen, prenatal attachment of pregnant women and their way of coping with stress are important factors. The coefficient for this factor was B0=0.352, and a strong positive correlation was found between prenatal attachment and stress coping levels (P<0.001). According to the analyses, a 1-unit increase in prenatal attachment level causes an increase of 0.352 in the stress coping styles mean score. Correlation analysis examined the relationship between this result and the subscales (Table 4).

According to the analysis results, there was a positive correlation between the prenatal attachment levels of the pregnant women and the seeking of social support and submissive approach styles and weak, optimistic, and moderate approaches, and a strong positive relationship with self-confident approach styles (P<0.001).
In the model, health literacy is an important variable in the prenatal attachment of pregnant women. The correlation coefficient for this variable was B0=0.108 (Table 3). A strong positive correlation was found between the prenatal attachment of pregnant women and health literacy (P=0.016). According to the analysis, a 1-unit increase in health literacy causes an increase of 0.108 units in prenatal attachment. Correlation analysis was performed to examine the relationship of this effect between subscales (Table 4). According to the investigations, we found a weak positive correlation between the prenatal attachment levels of the pregnant women and the subscales of understanding the information and appraisal/evaluation of the health literacy scale (P<0.001).
In addition, the prenatal attachment of pregnant women and the number of pregnancies and births significantly affected the model. The correlation coefficient for the number of pregnancies was B0=0.135, and the correlation coefficient for the number of births was B0=-0.231 (Table 3). A strong positive correlation was found between the prenatal attachment levels of pregnant women and the number of pregnancies (P<0.001). According to the analysis, a 1-unit increase in the number of pregnancies causes an increase of 0.135 in prenatal attachment levels. According to the analysis, a 1-unit decrease in the number of births causes an increase of 0.231 in prenatal attachment levels (Table 3).
4. Discussion
Our research was carried out to examine the effects of prenatal attachment levels of pregnant women on their stress-coping style and health literacy using a structural equation modeling.
Our study found that the prenatal attachment of pregnant women and the number of pregnancies and births had significant relationships. A strong positive correlation was found between prenatal attachment levels and the number of pregnancies (P<0.001). Research results show that prenatal attachment increases as the number of pregnancies increase [30, 31]. However, some studies show that the increase in the number of pregnancies does not alone explain the anxiety level and that the prenatal attachment levels of women with two or more living children are lower [4, 32]. So, prenatal attachment cannot be explained by a single variable. Variables such as age, education, employment, family type, income level, spouse relationship, desire and planning of pregnancy, number of pregnancies, number of births, past experiences, psychosocial health, social support, receiving preconception care, antenatal controls, preparation for childbirth are effective on the prenatal attachment [33, 34, 35, 36]. Therefore, it is necessary to examine all the variables as much as possible for each pregnant woman.
Thanks to the structural equation modeling, we found a moderate positive correlation between the PAI of pregnant women and the SCSS self-confident approach subscale and a moderate positive correlation between the optimistic approach subscale (P<0.001). At the same time, there was a weak positive correlation with the submissive approach subscale and no relationship with the helpless approach subscale.
Women experience different stress levels during their mental and physical changes throughout pregnancy [37]. Coping with perceived stress affects the health of their babies. It causes some adverse events (such as low birth weight, premature birth, and difficulty bonding with their baby) that can be experienced from pregnancy to postpartum [38]. For this reason, in terms of evaluating the positive or negative consequences of their perceived stress coping styles, it is necessary to investigate them [12]. It is found that pregnant women who explore their self-confident approach, have an optimistic approach to seeking social support, adopt a positive stress coping style, and are more eager to maintain their wellbeing and find solutions to problems [5]. It has been reported that positive or negative coping styles with stress experienced during pregnancy directly affect prenatal attachment [12, 39]. Therefore, psychological preparation is an important factor while preparing for pregnancy. Evaluating pregnant women’s physical health and psychological state and providing support should be among the routines.
According to a study that evaluated the relationship between stress coping style and prenatal attachment during pregnancy, there is a positive relationship between the attachment levels of those who show a self-confident and optimistic approach to coping with stress [12]. Positive coping methods have been reported to contribute positively to prenatal attachment levels [14, 40]. Regarding the second question of the study, the structural equation modeling showed a strong positive correlation between the HLS and PAI scores of pregnant women. Also, a weak positive correlation existed between prenatal attachment levels, health literacy scale, understanding information, and appraisal/evaluation subscales. For this reason, pregnant women need access to the right source of information. In general, it is thought that women experience more stress during pregnancy and cannot cope with the stress they experience properly because they act with customary knowledge.
In this study, 47.4% of the pregnant women were university graduates, and their Mean±SD HLS score was 112.10 ± 6.96. So, there may be a proportional relationship between high education level and HLS, affecting prenatal attachment. Accessing health-related information through the right sources and understanding and interpreting the acquired knowledge effectively maintain wellbeing during pregnancy [18]. The improvement of maternal and infant health, reducing maternal mortality, increase in the quality of health care, and reducing postpartum problems are associated with an increase in the health literacy level of women [21]. Asadi et al. stated that the level of health literacy during pregnancy is an important determinant that increases healthcare quality [41]. Studies have shown that the increase in health literacy level during pregnancy positively affects participation in health in the preconception period, pregnancy, and postpartum [21, 41, 42]. It has been reported that the mother’s health literacy during pregnancy is affected by factors such as the mother’s psychosocial health status, income status, and education level [43].
Regarding the third question of the study, the structural equation modeling revealed the relationships between stress coping style, health literacy level, number of pregnancies and births, and prenatal attachment. SEM showed strong associations between prenatal attachment, coping styles with stress, and the number of births. As a result of the analysis, coping with stress, health literacy, and the number of pregnancies and births explained 15.7% of prenatal attachment.
Health literacy also effectively contributes to postpartum parenting roles and feeling self-sufficient [43]. In other words, increased health literacy during pregnancy positively affects coping with stress and is associated with prenatal attachment [18]. However, no studies examine the relationship between prenatal attachment, coping with stress, and health literacy. Some studies examined prenatal attachment and stress coping styles or the effects of stress in pregnant women [12, 30, 32, 34]. However, no study examined the relationship between prenatal attachment and health literacy. In a research that was carried out to investigate the relationship between functional health literacy of spouses and prenatal attachment, it is stated that the increase in the health literacy rate of the spouses of pregnant women is effective on their attachment [44]. The study by Aslantekin Özçoban, Ergün, and Erkal Aksoy found that as the level of health literacy increases during pregnancy, adjustment to pregnancy and self-efficacy increases, and the fear of childbirth decreases [42].
For future studies, examining the relationship between prenatal attachment and health literacy in larger sample groups with different races, origins, and socio-demographic characteristics is recommended for future studies.
5. Conclusion
Prenatal attachment levels are associated with coping styles and health literacy levels of pregnant women. As a result of the structural equation modeling, we found a strong positive relationship between the PAI of pregnant women and the SCSS self-confident approach subscale and a moderate positive relationship between the optimistic approach subscale. A weak positive correlation was found with the submissive approach subscale. No relationship was found between the helpless approach subscale and prenatal attachment. A strong positive correlation was found between health literacy and prenatal attachment. Also, there is a strong relationship between prenatal attachment, coping styles with stress, and the number of births. It was concluded that health literacy and stress coping styles were effective variables in prenatal attachment.
Strengths and limitations
There are limitations to this study. First, the study was conducted in a single center. Although the absence of an exemplary research sample is the study’s strength, there was a limitation in making comparisons in the discussion section. At the same time, this is a strong side of the study’s originality. Other limitations are that the pregnant women answered the questions themselves, and the majority of those did not want to participate in the study because they were in the last trimester.
In this context, psychosocial support services should be provided to women to control stress, an important variable that will adversely affect pregnancy as soon as pregnancy is planned. In the content of these services, developing health literacy knowledge and skills is necessary. Secure attachment is also an important point to work on. For this reason, content that will evaluate the psychological status of women during routine pregnancy controls should be prepared, and both the psychological and social needs of women should be determined.
Ethical Considerations
Compliance with ethical guidelines
Before conducting this study, ethical approval was obtained (No. of meetings: 2022/18, Date: 16.02.2022). The purpose of the present study, its duration, and the participant’s rights were explained to the pregnant women before the study.
Funding
This research received no grants from any funding agency in the public, commercial, or not-for-profit sectors.
Authors' contributions
All authors equally contributed to preparing this article: Design, execution, and analysis of the results and approved the final version.
Conflict of interest
The authors declared no conflicts of interest.
Acknowledgments
We want to thank all women who participated in the research.
References
- Bowlby J. The bowlby-ainsworth attachment theory. Behav Brain Sci. 2(4):637-8. [DOI:10.1017/S0140525X00064955]
- Bowlby J, Ainsworth M. The origins of attachment theory. Attachment theory. dev Psychol. 1992; 45(28):759-75.[Link]
- Ataş AN, Akın B. [The relationship of sense of coherence in pregnancy with prenatal attachment and perinatal anxiety (Turkish)]. Turk J Fam Med Prim Care. 2022; 16(1):161-70. [Link]
- Badem A, Zeyneloğlu S. [Determination of prenatal attachment levels of pregnant women and affecting factors (Turkish)]. Kırşehir Ahi Evran Üniversitesi Sağlık Bilimleri Dergisi. 2021; 1(1):37-47. [Link]
- Lau Y, Tha PH, Wong DF, Wang Y, Wang Y, Yobas PK. Different perceptions of stress, coping styles, and general well-being among pregnant Chinese women: A structural equation modeling approach. Arch Womens Ment Health. 2016; 19(1):71-8. [DOI:10.1007/s00737-015-0523-2] [PMID]
- Rollè L, Giordano M, Santoniccolo F, Trombetta T. Prenatal attachment and perinatal depression: A systematic review. Int J Environ Res Public Health. 2020; 17(8):2644. [DOI:10.3390/ijerph17082644] [PMID] [PMCID]
- Demir Alkin E, Beydağ KD. Relationship between perceived stress level and self-perception level of women who had three or more pregnancies. J Psychiatr Nurs. 2020; 11(3):228-38. [DOI:10.14744/phd.2020.72621]
- Elkin N. [Ways of coping with stress affecting factors of pregnant women (Turkish)]. Mersin Univ J Health Sci. 2015; 8(1):22-31. [Link]
- Bakır N, Ölçer Z, Oskay Ü. The levels and affecting factors of prenatal attachment ın hıgh rısk pregnant. Int Refereed J Gynaecol Dis Matern Child Health. 2014; 01(01):25-37. [Link]
- Atalay D, Özyürek A. [The relationship between prenatal attachment and depression, anxiety and stress on pregnants (Turkish)]. Int Anatolian J Soc Sci. 2022; 6(1):46-59. [DOI:10.47525/ulasbid.1029374]
- Tuncel N, Süt H. The effect of anxiety, depression and prenatal distress levels in pregnancy on prenatal attachment. J Gynecol Obstetr Neonatol. 2019; 16(1):9-17. [Link]
- Daglar G, Bilgic D, Cakir D. The correlation between levels of prenatal attachment and styles coping with stress in pregnant women. J Reprod Infant Psychol. 2022; 40(3):254-65. [DOI:10.1080/02646838.2021.2001795] [PMID]
- Karakoça H, Ozkanb H. The relationship with prenatal attachment of psychosocial health status of pregnant women. Int J Health Sci. 2017; 5(1):36-46. [DOI:10.15640/ijhs.v5n1a6]
- White O, McCorry NK, Scott‐Heyes G, Dempster M, Manderson J. Maternal appraisals of risk, coping and prenatal attachment among women hospitalised with pregnancy complications. J Reprod Infant Psychol. 2008; 26(2):74-85. [DOI:10.1080/02646830801918455]
- Phommachanh S, Essink DR, Wright PE, Broerse JEW, Mayxay M. Maternal health literacy on mother and child health care: A community cluster survey in two southern provinces in Laos. Plos One. 2021; 16(3):e0244181. [DOI:10.1371/journal.pone.0244181] [PMID] [PMCID]
- World Health Organization. Improving health literacy [Internet]. 2009 [Updated 2023 April 19]. Available from: [Link]
- Dadipoor S, Ramezankhani A, Alavi A, Aghamolaei T, Safari-Moradabadi A. Pregnant women's health literacy in the south of Iran. J Family Reprod Health. 2017; 11(4):211-8. [PMID] [PMCID]
- Solhi M, Abbasi K, Ebadi Fard Azar F, Hosseini A. Effect of health literacy education on self-care in pregnant women: A randomized controlled clinical trial. Int J Community Based Nurs Midwifery. 2019; 7(1):2-12. [DOI:10.30476/IJCBNM.2019.40841] [PMID] [PMCID]
- Cho RN, Plunkett BA, Wolf MS, Simon CE, Grobman WA. Health literacy and patient understanding of screening tests for aneuploidy and neural tube defects. Prenat Diagn. 2007; 27(5):463-7. [DOI:10.1002/pd.1712] [PMID]
- Shieh C, Halstead JA. Understanding the impact of health literacy on women's health. J Obstet Gynecol Neonatal Nurs. 2009; 38(5):601-10. [DOI:10.1111/j.1552-6909.2009.01059.x] [PMID]
- Kilfoyle KA, Vitko M, O'Conor R, Bailey SC. Health literacy and women's reproductive health: A systematic review. J Womens Health. 2016; 25(12):1237-55. [DOI:10.1089/jwh.2016.5810] [PMID] [PMCID]
- Mutlu C, Yorbik Ö, Tanju IA, Çelikel F, Sezer RG. [Association of prenatal, natal, and postnatal factors with maternal attachment (Turkish)]. Anatol J Psychiatry. 2015; 16(6):443-50. [DOI:10.5455/apd.172669]
- Akça E, Sürücü ŞG, Akbaş M. [Health perception, health literacy and related factors in pregnant women (Turkish)]. J Vocat Sch Health Serv. 2020; 8(3):630-42. [DOI:10.33715/inonusaglik.735467]
- Charoghchian Khorasani E, Peyman N, Esmaily H. Measuring maternal health literacy in pregnant women referred to the healthcare centers of Mashhad, Iran, in 2015. J Midwifery Reprod Health. 2018; 6(1):1157-62. [DOI:10.22038/JMRH.2017.9613]
- Müller ME, Ferketich S. Factor analysis of the maternal fetal attachment scale. Nurs Res. 1993; 42(3):144-7. [DOI:10.1097/00006199-199305000-00004]
- Yılmaz S, Beji NK. [Turkish version of prenatal attachment inventory: A study of reliability and validity (Turkish)]. Anatolian J Nurs Health Sci. 2013; 16(2):103-9. [Link]
- Şahin NH, Batıgün AD. [A brief coping styles inventory for university students (Turkish)]. Turk J Psychol. 1995; 10(34):56-73. [Link]
- Toçi E, Burazeri G, Sorensen K, Jerliu N, Ramadani N, Roshi E, et al. Health literacy and socioeconomic characteristics among older people in transitional Kosovo. J Adv Med Med Res. 2013; 3(4):1646-58. [DOI:10.9734/BJMMR/2013/3972]
- Temel AB, Aras Z. [Evaluation of validity and reliability of the turkish version of health literacy scale (Turkish)]. Florence Nightingale Hemşirelik Dergisi. 2017; 25(2):85-94. [DOI:10.17672/fnhd.94626]
- Hopkins J, Miller JL, Butler K, Gibson L, Hedrick L, Boyle DA. The relation between social support, anxiety and distress symptoms and maternal fetal attachment. J Reprod Infant Psychol. 2018; 36(4):381-92. [DOI:10.1080/02646838.2018.1466385] [PMID]
- Özkan TK, Şimşek Küçükkelepçe D, Özkan SA. [Relationship between prenatal attachment and body sense inpregnancy and affecting factors (Turkish)]. Celal Bayar Univ Health Sci Inst J. 2020; 7(1):49-54. [DOI:10.34087/cbusbed.587467]
- Yılmaz SD, Beji NK, Yılmaz SD, Beji NK. Levels of coping with stres, depression and prenatal attachment and affecting factors of pregnant women. Genel Tip Dergisi. 2010; 20(3):99-108.
- Kurnaz F, Türkmen Çevik F. [Prenatal attachment scale: Reliability and validity study (Turkish)]. Hacettepe Univ Fac Health Sci J. 2019; 6(2):112-38. [DOI:10.21020/husbfd.453796]
- McNamara J, Townsend ML, Herbert JS. A systemic review of maternal wellbeing and its relationship with maternal fetal attachment and early postpartum bonding. Plos One. 2019; 14(7):e0220032. [DOI:10.1371/journal.pone.0220032] [PMID] [PMCID]
- Ustunsoz A, Guvenc G, Akyuz A, Oflaz F. Comparison of maternal-and paternal-fetal attachment in Turkish couples. Midwifery. 2010; 26(2):e1-9. [DOI:10.1016/j.midw.2009.12.006] [PMID]
- Zhang L, Wang L, Cui S, Yuan Q, Huang C, Zhou X. Prenatal depression in women in the third trimester: Prevalence, predictive factors, and relationship with maternal-fetal attachment. Front Public Health. 2021; 8:602005. [DOI:10.3389/fpubh.2020.602005] [PMID] [PMCID]
- Yoon SH, Sung MH. Does family support mediate the effect of anxiety and depression on maternal-fetal attachment in high-risk pregnant women admitted to the maternal-fetal intensive care unit? Korean J Women Health Nurs. 2021; 27(2):104-12. [DOI:10.4069/kjwhn.2021.05.14] [PMID] [PMCID]
- Ko SY, Bae JG, Jung SW. A comparative study on the anxiety, depression, and maternal-fetal attachment of high-risk pregnant women and normal pregnant women. J Korean Soc Biol Ther Psychiatry. 2019; 25(2):117-26. [DOI:10.0000/jksbtp.2019.25.2.117]
- Srivastava A, Bhatnagar P. Maternal foetal attachment and perceived stress during pregnancy. Int J Reprod Contracept Obstet Gynecol. 2020; 8(9):3750-6. [DOI:10.18203/2320-1770.ijrcog20193810]
- Pakenham KI, Smith A, Rattan SL. Application of a stress and coping model to antenatal depressive symptomatology. Psychol Health Med. 2007; 12(3):266-77. [DOI:10.1080/13548500600871702] [PMID]
- Asadi L, Amiri F, Safinejad H. Investigating the effect of health literacy level on improving the quality of care during pregnancy in pregnant women covered by health centers. J Educ Health Promot. 2020; 9:286. [DOI:10.4103/jehp.jehp_204_20] [PMID] [PMCID]
- Aslantekin Özçoban F, Ergün S, Erkal Aksoy Y. Effects of health literacy education on adaptation to pregnancy, self-efficacy, fear of childbirth and health literacy in Turkish pregnant women: A randomized, controlled trial. Health Soc Care Community. 2022; 30(2):e537-49. [DOI:10.1111/hsc.13690] [PMID]
- Lee JY, Murry N, Ko J, Kim MT. Exploring the relationship between maternal health literacy, parenting self-efficacy, and early parenting practices among low-income mothers with infants. J Health Care Poor Underserved. 2018; 29(4):1455-71. [DOI:10.1353/hpu.2018.0106] [PMID] [PMCID]
- Kazemi M, Sadeghi N, Mosavi M. [Investigating the relationship between maternal and fetal attachment and spouses’ functional health literacy in mothers (Persian)]. Avicenna J Nurs Midwifery Care. 2022; 30(2):116-23. [DOI:10.32592/ajnmc.30.2.116]
Type of Study: Orginal Article |
Subject:
● Psychosocial Health
Received: 2022/11/29 | Accepted: 2023/01/24 | Published: 2023/05/28
Received: 2022/11/29 | Accepted: 2023/01/24 | Published: 2023/05/28
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |